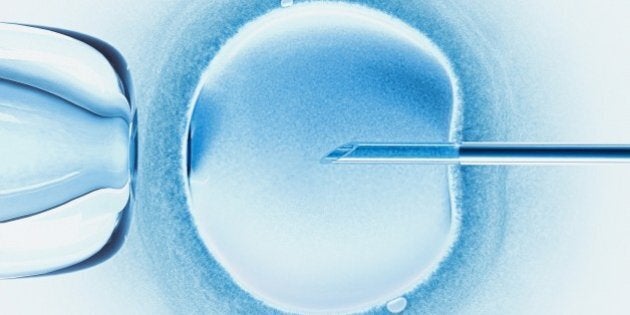
In a historic vote on February 3, 2015, the UK became the first country to allow a new, modified IVF technique called mitochondrial DNA transfer, which uses DNA from three people--two women and one man--to create a baby.
With headlines like "Three-parent babies!" exploding across the internet, it is easy to assume this new process will lead to the creation of children bearing the physical and psychological traits of three different people, but that is simply not the case. The amount of DNA transferred from the donor woman in the newly-legalized procedure is reportedly around 0.1 per cent, and does not affect things like height, eye colour, intelligence, musicality and so on. What it does affect, however, is the overall health of the egg and, prospectively, the health of the unborn child.
What is Mitochondrial DNA?
Mitochondria are vital to the functioning of the human body and are often referred to as the "powerhouse" of our cells. They are tiny compartments present in nearly every cell of the human body and they generate a type of energy that can be used by nearly every human cell.
Mitochondrial DNA contains vital information that allows mitochondria to create their energy, and when the DNA is mutated, or defective, severe genetic disorders such as brain damage, muscle wasting, heart failure and blindness can develop. Unfortunately, these disorders can only be diagnosed in retrospect and cannot be prospectively predicted in an unborn child unless a previous or existing family member has been affected.
What is this new procedure?
Defective mitochondria are only passed down from the mother, which means some women are unable to bring a healthy child to term. With "mitochondrial DNA transfer", the healthy mitochondria of a donor woman can replace damaged mitochondria in either a fertilized or unfertilized egg, which would prevent genetic diseases being passed from birth mother to child and thus to future generations. Up until this point, the only other option for women carrying the defective mitochondria trait was to use a donor egg that carried none of their genetic traits.
Mitochondrial DNA transfer has been hailed as a landmark in the Assisted Reproductive Technology world, and now begs new questions as to how else this procedure may help women who want to conceive. For instance, women are born with a limited number of eggs that age over time, which can make it more difficult to conceive later in life. Can mitochondrial DNA transfer provide a healthier energy source for older eggs by using the mitochondrial DNA of a younger individual who is more likely to conceive?
What's next?
This is a new science. We are still learning about it and it will take time to understand the full spectrum of repercussions--positive and negative--that result from this treatment and the children born of it.
In the meantime, there are things women can do right now to benefit their egg reserve and egg quality. In a recent study, Coenzyme Q10 was shown to improve egg quality, leading many doctors to recommend their patients take high doses of CO Q10 to support their fertility.
In addition, we always advise our patients to avoid smoking, pollutants, and toxins like bisphenols - all of which have been shown to negatively affect egg health. There is no approved way to stop a woman's eggs from aging, and new technologies remain in the early stages of development and testing. The best thing a prospective mother can do is stay healthy and educate herself on her fertility options.