Bill Pringle has attempted suicide eight times and police have always been the first to arrive at his home to save his life.
What he’s less sure of is how officers will treat him after the initial intervention, when he’s still deep in a mental health crisis triggered by the cyclical nature of bipolar disorder.
On some occasions, officers have remained indifferent, or acted like he was a criminal, said Pringle, the former chair of the Canadian Mental Health Association’s (CMHA) National Council of Persons with Lived Experience.
Watch: A timeline of violent police wellness checks in Canada. Story continues below.
In Vancouver years ago, police accused Pringle of attention-seeking and refused to call an ambulance. He said they handcuffed and transported him to the hospital in the back of their cruiser, and afterwards “dumped” him on the side of the road — kilometres away from home. He felt worthless, like a waste of their time.
“Many police officers still treat mental illness as though it’s a crime and that’s just wrong,” Pringle, 62, told HuffPost Canada.
Pringle moved to Saskatoon shortly after, where he said his experiences with police have been mixed depending on if the responding officers appear to be trained in assisting people in crisis.
The most positive encounter happened about five years ago during a suicide attempt, when Saskatoon’s Police and Crisis Team, which pairs a specially trained officer with a mental-health worker, arrived at the scene shortly after police. “An absolute godsend,” Pringle said.
“When the social worker started talking to me, the police officer stepped back so she could do her job properly. They were very compassionate.”
The team accompanied him to the hospital, and briefed the triage nurses on his condition. His recovery was significantly shorter — less than two weeks in hospital compared to previous stays of six weeks.

“When I didn’t have difficulty with police, my stays in hospital have always been shorter and recovery more complete,” he said. “Them being responsive to my needs more than the system’s needs made a significant difference.”
This alternative form of policing “should’ve been done years ago and universally,” said Pringle.
Police forces are experiencing an unprecedented surge in mental health-related calls, according to statistics HuffPost reviewed from eight services and all 13 RCMP divisions.
The RCMP is the country’s largest police force and it reported a substantial increase in mental health-related calls in every province and territory, including in Ontario and Quebec where it doesn’t do front-line contract policing, but has a federal policing mandate in the capital region of Ottawa and Gatineau, Que.
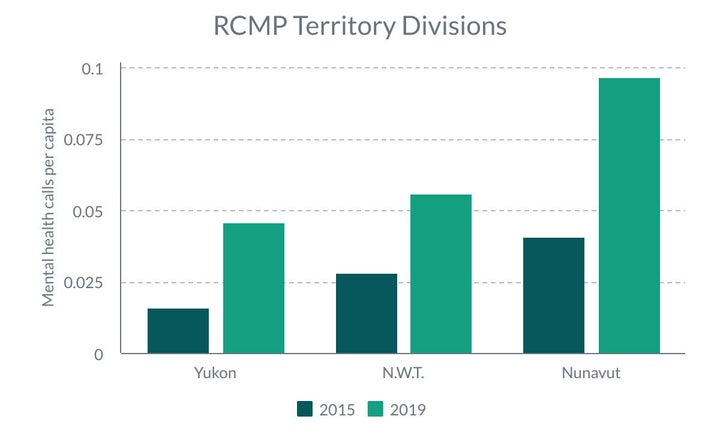
Some RCMP divisions reported a more than doubling in the number of calls compared to five years ago, such as in all three territories that experienced a total of 8,211 in 2019 from 3,342 in 2015, but where police have limited access to mental health expertise.
“In the course of their work [Northwest Territories] RCMP members work collaboratively and routinely with health care professionals, including nurses and social workers, but our division does not have a dedicated mental health crisis team,” the division said in a statement.
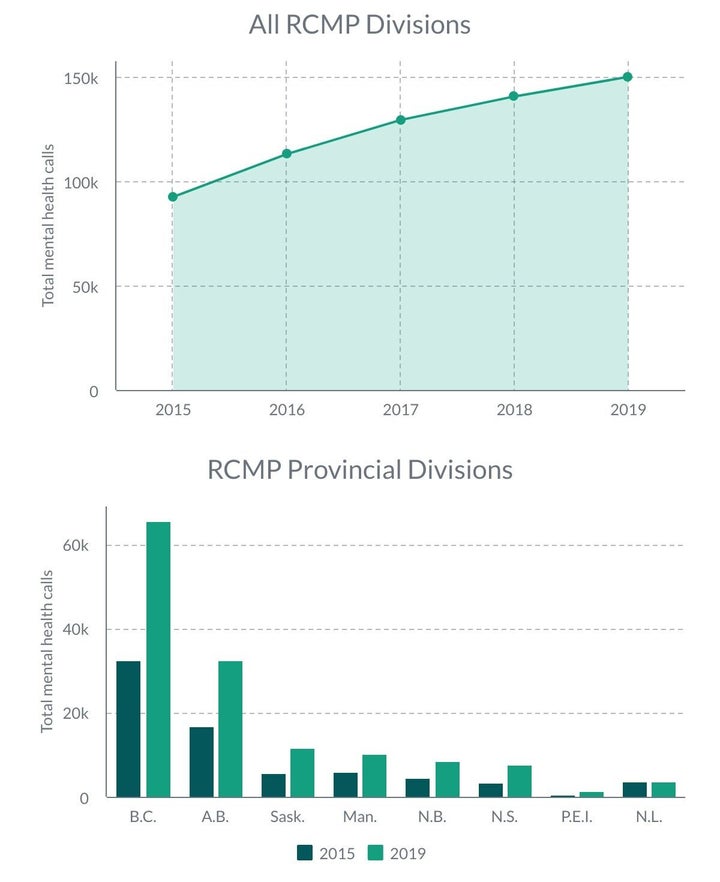
Municipal services have experienced a similar upward swing in calls, including those in St. John’s, Saskatoon, Calgary and Vancouver, and Toronto, Hamilton and the Durham Region in Ontario.
Police services in Halifax, Montreal, Winnipeg, Edmonton and Ontario’s Peel Region declined to provide information for this story without HuffPost filing a freedom of information (FOI) request that can take months to complete.
After HuffPost filed an FOI request for the number of mental health-related calls Montreal police have responded to in recent years, it said, “We regret to inform you that we have no document in relation with your request” and its computer system cannot retrieve that information.
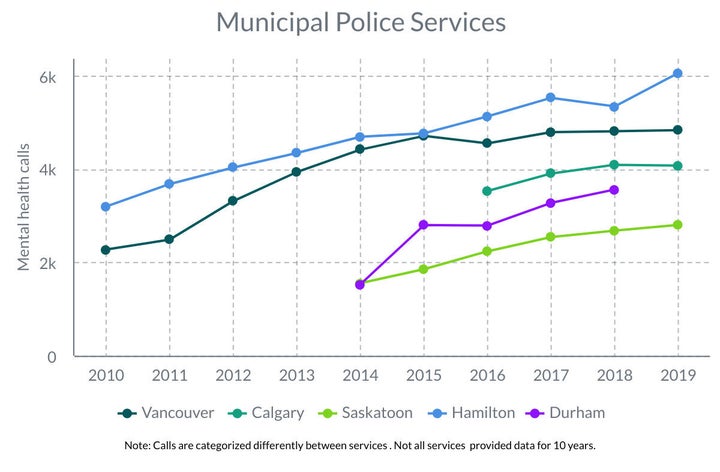
The data provided to HuffPost does not represent all police interactions with people suffering from mental illness, as some incidents may be filed as an assault, weapons complaint, suspicious occurrence, or noise complaint, among other situations. Police services and divisions log calls differently, which makes their statistics difficult to compare.
Mental health-related occurrences include officers enforcing their province’s Mental Health Act, or, in some jurisdictions, checking in on a person whose loved ones called police out of concern for their wellbeing. The legislation permits police to apprehend a person they determine is acting in a “disorderly manner,” or is at risk of harming themselves or others.
Some police forces have adapted to the demand for round-the-clock emergency mental health services by creating crisis teams that pair specially trained officers with psychiatric nurses or social workers from government health agencies. The units are considered secondary responders that will arrive at a scene after police have determined there’s not an imminent public safety threat.
It’s up to each police service, in consultation with local municipalities and the province, to decide what mental health support police will provide.
A patchwork of training, funding and partnerships with mental health agencies has resulted in some successes — such as in Hamilton, where its crisis intervention team assisted in close to half of mental health-related calls last year and is considered one of Canada’s best models for police crisis support.
For the most part, however, many communities are ill-equipped to help people in crisis without the use of force. Not all services have crisis intervention teams, and even where they do exist, the vast majority are not staffed 24 hours a day, and therefore cannot respond to all mental health-related calls determined to be non-violent.
“The commission’s reports have repeatedly found that this ‘command and control’ approach has led to the RCMP’s unreasonable use of force in apprehending persons in crisis.”
- Michelaine Lahaie, RCMP civilian oversight commission
On Tuesday, the RCMP’s civilian oversight commission released a statement that said in 14 confidential reports over five years it has highlighted concerns about police’s use of authoritative interventions when dealing with people who aren’t co-operating. These reports are about individual cases and haven’t been released publicly because of privacy reasons.
“The commission’s reports have repeatedly found that this ‘command and control’ approach has led to the RCMP’s unreasonable use of force in apprehending persons in crisis,” said Michelaine Lahaie, chairperson of the Civilian Review and Complaints Commission for the RCMP, in the statement.
The commission recommended this year that the RCMP work with provincial and territorial governments to create a way for health care professionals to lead the response for people in crisis and limit police involvement, Lahaie said, adding that she is waiting to hear back from RCMP Commissioner Brenda Lucki.
Justices and Ontario Ombudsman Paul Dube have reached similar conclusions in separate reports and reviews for other jurisdictions, such as Toronto, but change appears to be slow.
Out of 17 municipal police forces of different sizes across Canada, only London, Ont.’s has a crisis team that responds to emergency calls 24 hours a day, a recent study from the University of Western Ontario and Ontario Tech University found.
Toronto police’s mobile crisis intervention team operates 12 hours a day, and has recently come under fire for not responding to a call from a family whose daughter, Regis Korchinski-Paquet, was in crisis and ended up falling to her death from her balcony in May.
In response, Chief Mark Saunders told reporters that Toronto police does not send its crisis team to situations where there’s a “high probability of violence.”
Despite mental health-related calls increasing from 20,488 in 2013 to 30,689 in 2019, Toronto’s crisis team has never responded to more than 7,100 calls a year.
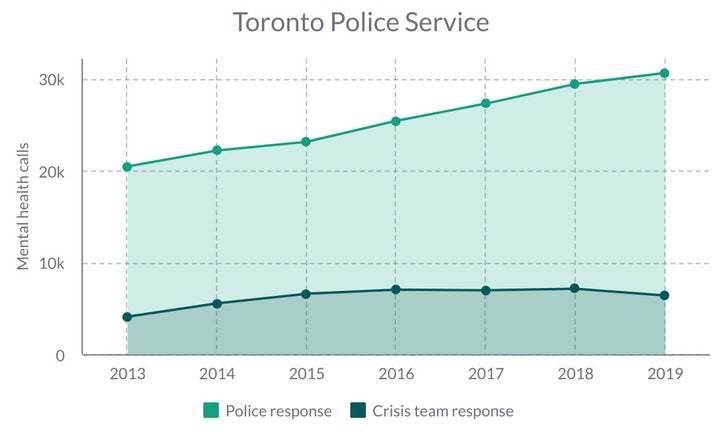
A lack of transparency has made it difficult for journalists, researchers and policymakers to determine how widespread crisis teams are and what’s working, said University of Toronto’s Erick Laming, a PhD candidate researching police use of force and accountability.
“There’s so much unknown about this area, we’ve barely even scratched the surface on it,” Laming said. “Police will always place the blame on the governments that they say didn’t give them the resources.”
The RCMP said the increase in mental health-related calls could be because Canadians and police are more aware of mental illnesses, and because of population increases.
Experts say the increase is also due to historically low funding for mental health support paired with the closing down of psychiatric institutions in the 1960s and ’70s. A lack of coordinated community services has left police to fill in the gaps, said Irwin Cohen, an associate criminology professor at the University of Fraser Valley and director of the Centre for Public Safety and Criminal Justice Research.
“I think they’re seriously playing catch up,” he said.
It’s a problem that’s been culminating for years. A 2003 study described patrol officers as “becoming the informal ‘first responders’ of our mental health system, and are filling this role without the necessary resources or support to carry it out properly,” warned the CMHA’s B.C. division.
“The result of this situation for people with mental illness can be long delays in receiving treatment, unnecessary trauma, violent incidents and criminalization that could have been prevented if care had been received earlier from the mental health system,” the report said.
One of five Canadians experience a mental illness, and more than 1.5 million are unable to access the care they need, such as counselling, according to a CMHA 2018 report. At 7.2 per cent of its health-care budget, Canada spends the lowest proportion of funds on mental health compared to all G7 countries.
“We’re still seeing the fallout of pulling back the social safety net,” said University of Regina Prof. Michelle Stewart, who researches policing practices, referring to when governments in the 1990s clawed back social spending.
“And we’re seeing this climate where it’s quite common for police services or the RCMP to get regular budget increases year to year because the demand does seem to be growing.”
Police operating expenses across Canada reached $15.1 billion in 2017-2018, according to Statistics Canada. The amount of taxpayer dollars spent on policing has increased consistently since 1986 from $294 per capita to $414, adjusted for inflation.
But a recent spate of violent police arrests, some of which ended in fatal shootings, has emboldened the public to demand parts of police budgets be reallocated to support community services, nurses and social workers who are also equipped to respond crises.
“Police officers simply do not have the skill set needed for these calls in the way the public is expecting them to,” said Stewart.
“We’re in a time period right now in Canada, where people are saying across the country that policing needs to be re-thought, and we need to think about how to best support everyone in our community.”
Stewart said that people in all communities need access to a crisis line where an expert responds and connects them to the supports they need. “And that happens outside of a policing call,” she said.
If police do attend a mental health-related call, all five experts HuffPost spoke to agreed that officers must be paired with a mental-health worker to ensure the person in crisis is treated with dignity, understanding and compassion.
“We’ve had too many tragedies,” said Dr. David Gratzer, a psychiatrist at the Centre for Addiction and Mental Health in Toronto, Canada’s largest mental health hospital, which released a damning statement in June calling for mental-health workers to be first responders in crisis situations, rather than police.
“Our current approach is accidental because no one was doing it and the role of police grew, but just because we’ve been doing something for decades, it doesn’t mean it makes sense or that there couldn’t be a better approach that saves lives,” Gratzer said.

When the Saskatoon crisis team assisted Pringle around 2015, it was still a pilot project and responded to 875 calls — close to half of all reported mental health-related calls made to the Saskatoon police that year, according to a provincial press release touting its success, and police statistics provided to HuffPost.
The unit continues to operate, but Saskatoon police said they no longer specifically track how many calls it responds to and directed HuffPost to file a FOI request.
Earlier this month, Saskatoon police officers responded to a request for a non-emergency wellness check for an Indigenous man who reportedly used a garden hose to bathe in front of an apartment building, according to CBC News.
The officers were captured in a six-minute video posted to YouTube sitting on Evan Penner, punching and tasering him. At one point as many as eight officers were pinning him to the ground as he repeatedly said, “Help me, please.”
Penner is charged with multiple criminal offences, including assaulting a police officer and possession of a controlled substance.

The first officer at the scene has been put on leave pending a review of his use of force. He was not a member of the crisis team, but had taken a 34-hour mental health training course offered to its police recruits about substance use, mood, anxiety and psychotic disorders, Saskatoon police told HuffPost. The training is meant to equip them to respond to situations including overdoses, suicidal behaviour, panic attacks, acute stress reactions and psychotic episodes.
The problem with police mental health training is that it is inconsistent across services, and insufficient given the wide range of mental health and addiction challenges police officers will encounter, said Cohen.
And it is “typically predicated on rationality,” Cohen added. “If I tell you to put your hands up, that will work if you’re a rational-thinking person. But if you’re in the middle of a schizophrenic psychosis episode, none of that is working.” That’s when, in some cases, police reach for non-lethal weapons like tasers, or their gun, he said.
RCMP officers are required to complete one, three-hour online course in crisis intervention and de-escalation, which includes a module on some major mental health disorders, said RCMP spokesperson Cpl. Caroline Duval.
“Police officers are not medical professionals and cannot diagnose individuals,” Duval said. “However, it is important for the police to have an understanding of mental illnesses, including signs and symptoms of distress, in order to conduct effective risk assessments and de-escalate a mental health crisis, wherever it is tactically feasible.”
Other courses, like suicide prevention, are mandatory for some staff, and how to de-escalate situations is a focus of cadet and annual training.
The RCMP said that on average it responds to 2.8 million calls for service each year, including 149,000 related to mental health in 2019, and only 0.1 per cent result in use of force.
Research suggests that 30 per cent of people experiencing serious mental illness will first come into contact with police when attempting to get help. One study found that police are more likely to use force on a person they perceive has a mental health disorder, and they’re also more likely to believe that person is resisting arrest.
A CBC investigation found that 70 per cent of people fatally shot by police between 2000 and 2017 suffered from mental health and substance abuse problems.
In Kelowna, B.C., nursing student Mona Wang is suing the RCMP over what she said was an officer’s excessive force and alleged brutal conduct during a health check that left her with cuts, bruises and a swollen eye. Wang said she was semi-conscious when she was handcuffed and made to lie on her stomach as the officer held her head down with a booted foot, an incident that was captured on surveillance video.
Kelowna RCMP operate one crisis team from Tuesday to Friday. Wang’s boyfriend requested a wellness check on a Monday.
In response to the incident, Supt. Brad Haugli, head of the Southeast District, said at a press conference earlier this month that he wants to add more mental health teams in the region.

B.C. RCMP were unable to provide the number of mental health-related calls its crisis teams respond to. Of more than 150 detachments, 11 have access to such units, including several communities that share one car.
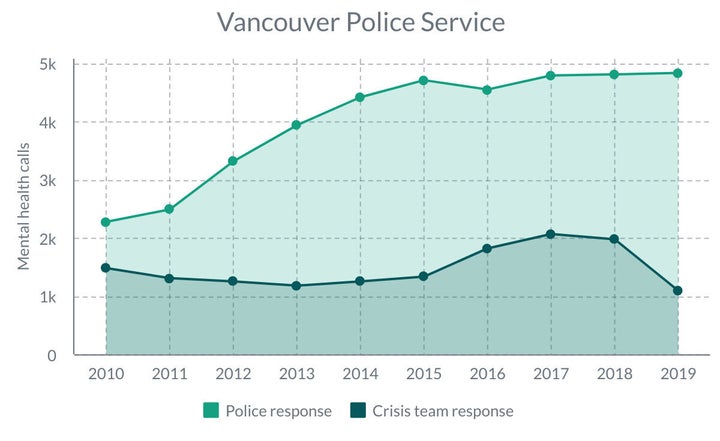
While Vancouver police received more than two times as many mental health-related calls in 2019 compared to 2010, its crisis team attended to half the number of calls as it did in previous years. The crisis team was limited to one car because the local health authority that provides the mental-health workers was “adjusting staffing,” said spokesperson Const. Tania Visintin.
Quebec’s provincial police serve more than 1,200 municipalities and have seen a steady increase in mental health-related calls, from 14,884 in 2014 to 20,115 in 2019. Yet, it does not have any crisis teams dedicated to assisting people with mental health difficulties.
Saskatchewan and Alberta each have more than 100 RCMP detachments, but only two and three crisis teams, respectively.
In Alberta that translates to crisis teams responding to less than one-eighth of all mental health-related calls from January to May of this year.
“As RCMP members, we do care about people and want to do a good job and help people,” Alberta RCMP spokesperson Cpl. Deanna Fontaine told HuffPost. “That’s why we have the [Police and Crisis Teams], to do better and learn from our mental health partners and provide a better service for those clients that are in crisis.
“I wish we could have them everywhere. Unfortunately we just don’t have the funds for that.”
Dalhousie University law Prof. Archie Kaiser called the Alberta RCMP’s stance a “truly startling admission because what it says is we know we aren’t serving the public adequately but we are determined that the public can bear that cost.
“We don’t say to victims of heart attacks, ‘I’m sorry, you have to have your heart attack within business hours and only in urban centres.’ That would be inconceivable. And yet, we are willing to tolerate service limitations for mental health-related needs.”
“We have to get away from the stigma of what mental illness was 20 years ago.”
- Sgt. Peter Wiesner, Hamilton Police Service
It is unclear how much it costs to fund a crisis team as the vast majority of services that HuffPost spoke to, including the RCMP, were unable to provide an estimate — deferring to other levels of government.
Hamilton police, in partnership with St. Joseph’s Healthcare, runs two types of crisis intervention teams, which cost $1.6 million — or less than 1 per cent of its $171 million budget for 2020.
The service has trained half of its 800 officers in crisis intervention. The in-person course is 40 hours long and includes hearing from people with lived experience.
“We have to get away from the stigma of what mental illness was 20 years ago,” said acting Sgt. Peter Wiesner, who leads the program.
“What we do is so groundbreaking that services from all over Canada look to us for guidance to create this program. We like to call it the gold standard.”

The city has two Crisis Outreach and Support Teams that each include a mental-health worker and a plain-clothed officer driving an unmarked car that responds to calls made to a 24-hour crisis line. They do follow-ups after emergencies to make sure the person has access to services.
Three Mobile Crisis Rapid Response Teams (MCRRT) respond to 911 calls, with the officer in uniform and in a police cruiser, accompanied by a mental-health worker, available 17 hours a day.
“We’re trying to avoid having a regular patrol unit attend persons in crisis unless, obviously, one of our three units are tied up,” Wiesner said.
Last year, MCRRT responded to 2,549 people in crisis, out of 6,059 mental health-related calls. The outreach team made 2,358 mobile visits. Hamilton police could not say definitively how many of these interactions result in officers using force except that it’s a rarity, according to Wiesner. New statistics will be released at a police service board meeting later this week.
Before MCRRT began in 2015, 75 per cent of all mental health-related calls resulted in the person in crisis being apprehended by police and brought to the hospital, Hamilton police said.
By 2019, that rate had dropped to 22 per cent because the mental-health worker can often connect a person to the resources they need without going to the emergency room, said Sarah Burtenshaw, one of the mental-health workers who has assisted police for almost 20 years.
Hamilton police launched their mental health crisis program in 1997, after two tragic events demonstrated gaps in mental-health care and spurred the city to take action, said Burtenshaw.
The first was the death of Mary Popovich, a mentally ill, homeless senior who died in 1992 with open sores covering her legs and experiencing the symptoms of pneumonia. And in 1995, two-year-old Zachary Antidormi was stabbed to death by a neighbour in an extreme state of mental illness. Police had been called to assist the woman many times but failed to help.
“Things change, and we have to respond accordingly,” said Burtenshaw. “That’s really how rapid response came into being, with people saying we need a mental-health worker right here right now. And that’s what we’re able to provide.”
If you or someone you know needs help in Canada, contact Crisis Services Canada at their website or by calling 1-833-456-4566. You can also find links and numbers to 24-hour suicide crisis lines in your province or territory here. This guide from the Centre for Addiction and Mental Health outlines how to talk about suicide with someone you’re worried about.