
Influenza is a nasty virus, as anyone who has been infected can attest. For most Canadians, the affliction only lasts for a few weeks before life returns to normal. But each year, thousands suffer more dire consequences and require hospitalization. Even with the best treatment options available, hundreds of these individuals still succumb to the illness.
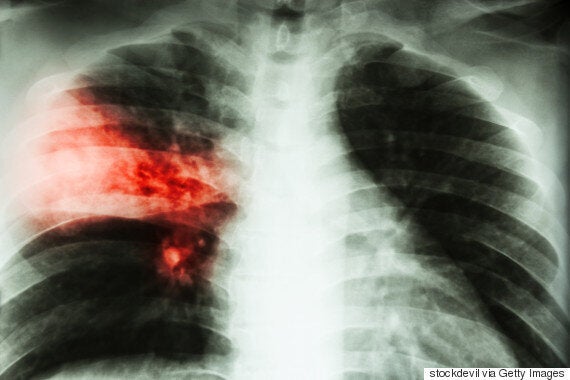
This rather depressing picture is worsened when one looks inside the lungs during infection. While the virus is actively infecting and killing cells, two branches of the immune system are hard at work to ward off the invasion. One arm, known as cellular immunity, conducts a coordinated attack. It hones in on the virus and ensures the situation is handled. The other, inflammation, is far less discerning. Its job is to wipe the slate clean regardless of what may be taken out in the process.
If it is not controlled, it can put anyone's life at risk.
Normally, there is a balance between these two regiments of the immune force. However, in individuals with weaker immune systems -- such as the elderly and the very young, as well as those with pre-existing conditions such as diabetes, cancer, morbid obesity and respiratory ailments -- inflammation can take over. This could end in what is known as a cytokine storm. As the name implies, the phenomenon ravages our inside environment. If it is not controlled, it can put anyone's life at risk.
For years, researchers tried to discover ways to reduce the toll of inflammation on the body. Initially, the concept of boosting cellular immunity to level out the playing field was considered an option. But as the mechanism behind the cytokine storm became known, the idea fell out of favour. Inflammation was not being controlled by these immune cells. Instead, it was being called for by the very cells under attack.
With this information in hand, the only answer appeared to be calming inflammation. This could be accomplished through the use of anti-inflammatory drugs, but they were not altogether trustworthy. In 2011, the concept of introducing drugs into the lungs was shown to be somewhat effective in mice. Yet this too was considered less than optimal. In order to truly balance the immune response, a drug needed to prevent infected cells from sending out the signal asking for inflammation and eventually, that cytokine storm.
For an international team of researchers, this need began a journey to find candidates capable of systemically reducing inflammation. Last week, they reported on one such molecule. It's known only as FP7, but based on its ability to help reduce the effects of inflammation -- at least in mice -- it may have a very bright future and eventually, a fancier name.
The team focused on one of the proteins known to be involved in inflammation called Toll-Like Receptor 4, or simply, TLR4. It's found on many different types of cells and acts as an early warning signal for the body. Once this molecule senses trouble, it will call for an inflammatory backup. Normally, the response is balanced, but in the case of viruses like flu, the signal may lead to a massive response and eventual storm.
In the studies, mice were infected with lethal doses of flu virus. Then, some were injected with FP7 in the hopes of reducing the toll of inflammation. These mice ended up living while those given the control in the form of saline, died. From a purely life versus death perspective, FP7 seemed to be perfect.
But the team wanted to know more about why FP7 worked so well. They did this by looking at the lungs of the mice. The lungs of control mice were a mess. Inflammation had ravaged the tissue and left the animals with very little chance to survive. On the other hand, the lungs of the mice who had received the drug appeared to be relatively normal. While there were some signs of infection, the effects were minimal.
This distinct difference in the tissue led the researchers to examine whether FP7 had led to a more balanced immune response instead of boosted inflammation. As expected, all the signs of a cytokine storm were gone in the mice given the drug. It had ensured inflammation was balanced and did not run amok in the lungs or elsewhere in the body.
The results of this study suggest FP7 indeed may be a good candidate for influenza treatment down the road. With further testing in animals and eventually clinical trials in humans, we may be able to help those most vulnerable to unnecessary and dangerous outbursts of inflammation.
We should focus on reducing inflammation.
The results also reveal the importance of immune balance during an infection. Unlike what we may hear in the public, there is no good way to boost our immunity; it even may end up being troublesome. Instead, we should focus on reducing inflammation. If you are infected, anti-inflammatory medications will probably be of service.
Natural options do exist. One is Vitamin D, known for immune balancing properties. Then there are those omega-3 fatty acids, which can help keep the immune system on track against viruses like influenza.
Of course, if you want to stick with remedies from the past, you could go for a long-standing flu soother that we now know doubles as an immune balancer. It's none other than good old-fashioned homemade chicken soup.
Follow HuffPost Canada Blogs on Facebook
Also on HuffPost: