According to the American Lung Association- about 5,000 to 10,000 babies born in the United States each year have BPD (bronchopulmonary dysplasia). BPD is also known as Chronic Lung Disease. More babies today have BPD than 30 years ago because more and more very premature babies are surviving.
Bronchopulmonary dysplasia (BPD) is a lung disease that is seen most often in babies who were born severely premature--more than 10 weeks before their due date.
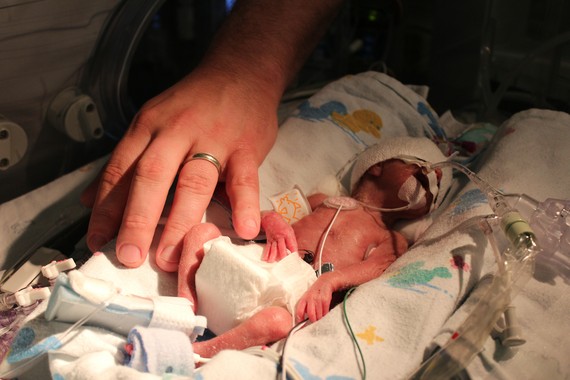
My daughter was born 17 weeks early and she suffers from BPD.
Joy was born a micro preemie (baby born before 26 weeks) at 23 weeks gestation in 2012. Her early birth was caused by my placenta percreta (a very dangerous form of placenta accreta). Babies with BPD have inflammation and scarring in the lungs and often develop asthma later in life.
According to Kidshealth.org, after coming through the more critical stages of BPD, some infants still have longer-term complications. They are often more at risk for respiratory infections, such as influenza (the flu), respiratory syncytial virus (RSV), and pneumonia. And when they get an infection, they tend to get sicker than most children do.
That's for sure!
Joy has had pneumonia numerous times since she was discharged from the NICU and most times required long hospital stays and time back on oxygen. One time was caused by the Human metapneumovirus (the cousin of RSV) and the other from the regular Rhinovirus or regular common cold. Most full term babies with healthy lungs would fight these off on their own. Not Joy.
What can we parents do about it? I'll get to that soon.
My daughter recently turned 3 years old and on most days you would never notice that she has very weak lungs, but it's very apparent when a respiratory virus invades them.
Joy spent 4 months (121 days to be exact!) in the NICU (neonatal intensive care unit). Like most micro preemies, the beginning of her life was very difficult due to the many medical interventions needed to keep her alive. It is a blessing that she is not able to remember the countless blood transfusions, intravenous lines, PIC lines, X-rays, intubations, extubations, heel sticks, and other daily stresses of her first few months on Earth.
My daughter graduated the NICU with little scars from her beginning battles against her war on prematurity, yet she is left with one constant battle to fight- the one against her lungs.
We are ready to fight and win!
So why do preemies get BPD?
Premature babies are born with underdeveloped lungs and cannot breathe on their own and need to be placed on ventilators that provide them with pressurized oxygen. The act of the machine forcing a baby's lungs open and shut can damage the infants' delicate airways and lead to respiratory distress syndrome (RDS). If symptoms of RDS continue for more than one month after birth, the condition is classified as bronchopulmonary dysplasia (BPD). Many infants will outgrow mild cases of BPD, though they may have some continuing symptoms. In rare cases, BPD can be fatal.
Medications are available to help premature babies survive their compromised lung conditions- with surfactant being arguably the most important. Here are the most common:
•Surfactant given at birth can help reduce death in preemies. Very premature babies do not produce enough surfactant to keep their air sacs open, which is what surfactant, will do, as well as reduce lung tears. Surfactant is delivered using an artificial airway or breathing tube that is inserted into the trachea either immediately at birth for extremely premature babies, or later once respiratory problems have revealed themselves.
•Bronchodilators (to help open the airways)
•Steroids (to help to reduce inflammation)
•Diuretics (to help reduce excess fluid in the lungs)
After discharge from the NICU, babies with chronic lung disease often go home with nebulizers and inhalers that cane be used multiple times a day to help reduce the chances of the baby developing pneumonia from a respiratory infection.
But what can us parents do to help our children strengthen their lung capacity as they grow- post NICU?
I have been researching this for over two years and have compiled a list of some great exercises and games for babies and toddlers that we have used and continue to use this summer. My list comes from meetings with neonatologists, pediatricians, pulmonologists, fitness teachers and parents of older preemies.
I want to mention that I am just a science teacher and mommy of 4 (my youngest being a micro preemie) and I have no medical training. Please use my list to have discussions with your doctors before trying anything that may be too much for your child to handle.
Here are 11 fun activities to try that may help your child build up their lung strength:
1. Pushing Out- This exercise was popularized by doctors Paul and Patricia Bragg, authors of Super-Power Breathing. Have your child assume an upright posture, preferably standing on flat ground. Keeping both knees loose, have them bend over from the waist, simultaneously pushing out all air from your lungs. Then they should slowly return to a vertical position, inhaling at an equal rate. Next have them fill their lungs to the greatest degree comfortably possible and hold this breath for a count of 20 seconds (or less if 20 sec is too long). While counting, have them extend both arms fully overhead then relax, lower their arms and exhale slowly. Complete this cycle four times.
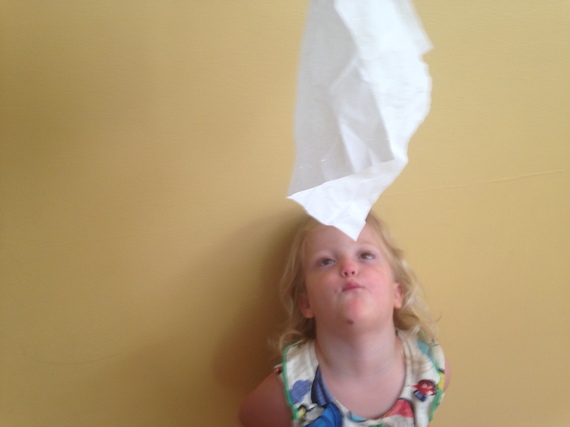
2. Flying Tissue- Another fun exercise is to tape a long, light slip of paper (or a tissue) to the tip of your child's nose and have them try to keep it in the air by blowing it as long as possible.
3. Take it to the water- Mommy/Daddy and Me swimming classes are great for this! But if those are not available, you can do some similar exercises on your own. While being submerged in water up to your shoulders, blood shifts into the chest cavity and you will have to take shorter, quicker breaths when exercising. Research shows that your air capacity will be cut by up to 75% during this time, and your body will try to compensate for that. Experts say that if you exercise in the water regularly, your respiratory system will become more efficient, increasing your lung capacity. Why not try this with your babies if they are healthy enough to do it?
4. Dance Party- It can be surprising how much lung capacity you can develop doing short bursts of cardiac exercise. Throw on some music and dance for 5 minutes.
Take a break in between to relax and drink some water then do it again! My kids love this!
5. Ride a Bike- Once your baby is able to ride a bike with training wheels- go cycling. And while you're at it, through in some elevated climbs. Going up hills means your body needs to pump more blood to your legs and your lungs supply the oxygen to the blood.
6. Play a wind instrument- Encouraging your child to play a wind instrument is a great way to give their lungs a regular workout. It will teach them to control their breathing and expand their lung capacity to utilize all the alveoli. And it can be something they do for the rest of their life.
7. Sing a Song- Singing really works the diaphragm, and can aid in continuous breathing exercises.
8. Blow up Balloons- While this may not be safe for younger children due to the choking hazard, it can be supervised and the balloons can be hit or kicked around for fun once they are filled with air. This activity can help strengthen the lungs.
9. Blow Bubbles- This can be enjoyable for everyone. Siblings can run and try to pop the bubbles floating through the air. What a fun way to help your baby exert their lungs.
10. Move a Feather- Place a feather on a table and encourage your child to blow it across to the other end of the table. You can even draw a "finish line" on the table so the win can be celebrated.

11. Laugh- Tickle, tell jokes, make silly faces and have as much fun as you can with your child. Not only will these moments make lifetime memories for your family, but the laughing will help increase everyone's lung capacity.
I am happy to report that Joy, after 3 years of twice a day steroid treatments (through the nebulizer at first and then the inhaler), has been taken off all steroids! It has been three weeks since her last treatment and she is breathing like a pro!
What other methods have you used to help improve your child's lung capacity? I would love to hear them!