There’s one question I’ve been asked more than any other in my adult life. On a recent visit to the emergency room, I heard it once again. My pain was so intense I could hardly tolerate the standard intake procedures: getting my blood pressure taken and explaining why I was there was beyond me. When I told the admitting nurse about my symptoms, she followed up with those overly familiar words.
“What’s your pain level on a scale of 1-10?”
I couldn’t do it. It might have been the feeling of scalding hot knives piercing my body that caused me to rebel against the nurse’s inquiry. Maybe it was the bored look in her eyes, which stayed fixed on the computer screen as she talked to me. Whatever it was, I wasn’t going to play the game, not this time.
“I’m in the ER,” I groaned.
That didn’t satisfy her. She repeated her question as if I didn’t understand the first time. I squirmed in my chair and told her it was off the charts, beyond a ten, and I wouldn’t be there otherwise.
I suppose I should be grateful she didn’t give me the smiley/frowny-face version of the pain scale; instead she murmured “10” and continued typing as if I wasn’t there.
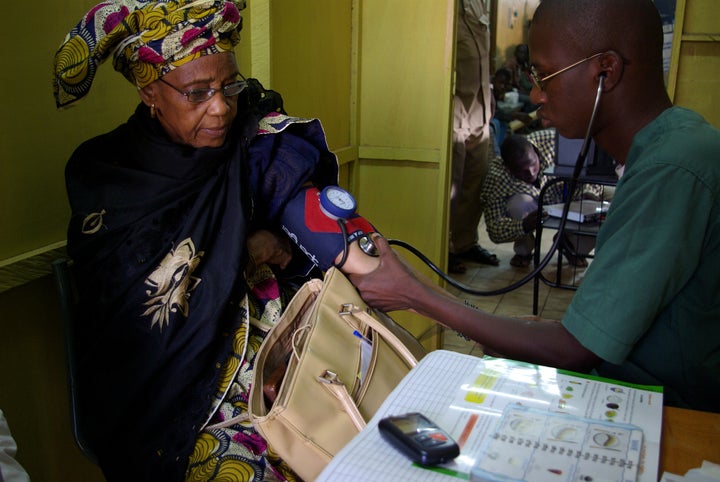
I am one of the 100 million americans who suffers from chronic pain. This number exceeds those affected by diabetes, heart disease and cancer combined, according to the American Academy of Pain Medicine. The more than 900,000 doctors in the United States and multitude of nurses need a better way of interacting with and caring for this astronomical amount of people.
Chronic pain presents a myriad of other problems as well. While knowledge has increased over the years, pain is still poorly understood, and most physicians aren’t trained in managing it clinically. Many doctors lack information about less common underlying causes and related conditions. This makes it difficult for patients to get an accurate diagnosis. Another concern is that the medical profession often fails to acknowledge the emotional aspects of pain, or even the effects pain has on daily living.
As if these barriers to patient care aren’t enough, society often disbelieves or blames people in in chronic pain. This stigmatization leads to further suffering from isolation and lack of appropriate care. Uninformed and biased response to use of opioids is one unfortunate example of this, as is the American Medical Association’s mind boggling determination that pain assessment is no longer a necessary part of patient-doctor dialogue.
One of the most significant problems is that the medical world has limited ability to measure how a person hurts. This means chronic pain sufferers aren’t getting the support or relief they need.
The standard measurement of pain consists of a description by the patient (typically brief) and the doctor’s interpretation, both of which are too vague. Unlike blood pressure or temperature, clinicians can’t objectively measure pain.
The 1-10 scale can offer information to a certain point, but its usefulness is severely limited. At times it’s even more stressful than helpful; it certainly was for me that recent night in the emergency room. I knew my answers gave no particulars about how I felt, and I had to rate my pain so many times I lost count. I was asked at intake, when I got into a room, the moment I swallowed medication, after they took images, and every time another nurse came by.
Aside from the minimal information my number provided, how much difference was a few minutes going to make? Typically, not enough to move up or down on the arbitrary scale. I suppose I could have rated the pain in more detail, like I was an olympic competitor, and given digits based on execution and difficulty. The nurse fails to properly insert the IV into my vein for the fourth time? A one point gain. Slightly less hurting in one of multiple painful areas? One-tenth of a point deduction.

As patients with pain, we are judges determining our own scores, but, it is our role as expert commentator that needs to be honored in the doctor-patient relationship. Medical professionals need a better way to understand the many levels of a person’s suffering, and the only way to do this is to gather information directly from patients. We need to be able to share our narrative with our doctors.
Even though pain is subjective, there’s a well-regarded method which can help. In 1971 Dr. Ronald Melzack and his colleagues at McGill University developed an assessment tool called the McGill Pain Questionnaire (MPQ). A review of the MPQ resulted in the development of a short-form version, the SF-MPQ-2 (revised in 2009), which addresses both neuropathic and non-neuropathic pain. This is the first tool of its kind to measure pain on a multi-dimensional level. Although far too few doctors implement it in their practice, it’s one of the most reliable pain assessment resources available, and is used by clinical researchers around the world.
The pain questionnaire offers descriptors to measure three dimensions of a person’s pain experience: affective (emotional impact of pain such as fear, anxiety or depression), sensory (location, intensity, temperature, pressure, pattern), and evaluative (intensity of the overall experience, actions that increase or decrease pain). Patients choose from well-researched descriptors (such as throbbing, stabbing, sharp, searing, numb, dull, cold, torturing) to explain the effect of pain in each of these three areas.
You can imagine how useful this could be when used over time to determine how we respond to treatments, and to see patterns of progression or remission.
Another helpful tool is the McGill Pain Index (MPI), a scientific pain scale born from the McGill questionnaire. A diagram rates the level of pain for various conditions on a scale from one to fifty; zero indicates an absence of pain, while higher numbers show increased suffering.
As an example, when you look at the index you see that a fracture rates as a 17. Complex Regional Pain Syndrome (CRPS), one of the most painful conditions that exists, has a score of 46. That means it’s more painful than those with lower numbers including unprepared childbirth, non-terminal cancer and amputation. As somebody who personally lives with this harrowing medical issue, the chart emphasizes why CRPS is nicknamed the “suicide disease.”
So, considering the value and potentially powerful impact of these assessment tools, who can they help?
Medical and mental health professionals.
The questionnaire can help doctors discriminate between varying medical conditions, make diagnoses, and more effectively treat patients. The pain index can help psychotherapists conceptualize the physical impact of a particular problem that’s unfamiliar to them. Like any other approach, this can only be effective when there is a trusting and mutually respectful relationship between patient and caring professional.
Family, friends, care-givers
Many people with chronic pain feel they lack adequate support. Although loved ones shouldn’t need a diagram to help them with empathy, a look at the pain index could expand their hearts (and minds). It might inspire compassionate souls to extend the simple kindness of reaching out on occasion. See Christine Miserandino’s wonderful and clearly explained Spoon Theory to help those in your life understand your day to day reality.

Women
With respect to men who also suffer from pain, it’s no secret that women in particular tend to get misdiagnosed or dismissed in the medical world. The overwhelming bias results in women getting less access to medications and insufficient (or an absence of) treatment. Among these and other injustices, the impact of insufficient care can lead to anything from reduced physical functioning to life-threatening circumstances. For Grace is a fantastic organization that supports women in pain.
People with chronic pain
We can suggest that our doctors use the questionnaire and index to understand more about the source of pain, as well as it’s quality or intensity. Pain may persist despite multiple levels of treatment and self-care. Sadly, sometimes patients blame themselves, or feel frustrated about the various levels of impact pain has on their lives. The scientific picture comparing conditions can offer much needed perspective.
Patients with rare diseases or poorly understood medical conditions—and those providing treatment
CRPS, as mentioned above, is one example of a rare disease. Most of us who have the condition suffer alone for a long time prior to receiving any help. We see about six doctors before we even get an accurate diagnosis. This is a devastating truth considering early intervention is key to increasing the likelihood of successful treatment. Link here for information on other conditions.
Although the complexities of pain need more attention, the questionnaire and resulting pain index’s long-standing, reliable outcomes can help to demystify a person’s agony. Patient-centered assessment tools, which move beyond the simplicity of a number, have potential to positively impact the medical community and society as a whole.
The value for people suffering from pain? Beyond measure.
Elisa Friedlander is a licensed psychotherapist. Currently unable to practice due to an excruciatingly painful neurological disorder, complex regional pain syndrome (CRPS), she is active in disability and pain communities. Much like her tendency to belt out 70’s music in the bathtub (the sappier the better), she often writes while submerged in water. Now that she extends some of her writing to the public, what happens in her tub no longer stays in her tub. Elisa has been published in a local mental health publication, a national medical newsletter distributed by www.rsds.org, and contributes to The Mighty. Convinced that pain and humor must play nicely together, Elisa can be heard laughing with her wife moments after yelping out in pain during intermittent visits to the emergency room. Elisa loves living in the San Francisco Bay Area with her wife and best friend (one in the same) and their irresistible rescue dog, Zakai. A baby elephant would complete the picture. More of her story and other writing can be seen on her blog at https://www.ElisaFriedlander.com
If you or someone you know needs help, call 1-800-273-8255 for the National Suicide Prevention Lifeline. Outside of the U.S., please visit the International Association for Suicide Prevention for a database of resources.
