
“Young Woman on her Death Bed,” unknown, Flemish,1621
I feel exhausted and gutted, like a doe that’s finally been caught after a long chase. I want to crawl between the sheets by nine o’clock. Words are lost before they get to my tongue—thanks to hormonal effects on the temporal-lobe declarative memory-system of my brain—and objects are not quite what they appear. I don’t mean that I’m hallucinating, but it’s as if my mind takes a picture and labels it wrongly, then feeds my mouth the incorrect title.
For example, during a drive with my family, what I think is a small chicken darts into the grasses on the side of the road. “Oh, look at that!” A tiny Araucana, I almost announce. When my husband asks what I’m pointing to, I stumble over the words, “It was just a cardinal.”
It’s summer, 2012, and I’ve had my period three times in eight weeks, for longer than five days each time. If this keeps up, my doctor warns, I will be admitted to hospital for I.V. iron and fluids. I’m taking an estrogen receptor balancer, which should help control the bleeding. My other options are a DNC followed by a uterine ablation, synthetic hormone tablets or, worse, more leuprorelin injections with intolerable side effects (past injections will eventually lead to hypothyroidism). An extremely low iron count is just one indicator of my condition, one facet of this game in which I’ve been an unwilling participant since childhood.
At age eight I was often mistaken for a boy. I had pixie-short hair, was stick-thin, and already over five feet tall. “You’d make a perfect flapper,” my great aunts enthused, hoping to cheer me when I neared teenagehood. But this was the early era of silicon implants and aerobics, and my figure was incompatible with society’s idea of normal: Christie Brinkley in Sports Illustrated, posted inside every boy’s locker door.
Just before my 15th birthday—some three years later than most of my peers—menstruation began with a startling adult fervor. Each month’s episode was heavy and painful, and I tottered my way to the school bus in a dizzy haze.
Instead of hair gel and toothpaste, my medicine cabinet housed half-empty bottles of pamabrom, mepyramine, ketoprophen, mefenamic acid—all prescribed for “period cramps,” but none reliable. The “growing pains” that set my legs on fire continued long after I finished growing, and my figure was nearly skeletal. I was often exhausted, run-down, infested with colds, a consumptive character from another era. My shy, mousy tendencies, wearing tweed skirts and reading A.E. Poe under a tree at recess, was greeted with scorn and bullying by my peers. For, suburban American teens are meant to attend of kissing parties and football games; they are most certainly not to be secretly living a life of daily nausea, pain, and blood-soaked sheets.
Various pediatricians approached me with a mix of skepticism and scorn, consistently announcing that all was “normal”: a term used to explain everything from the healthy to the outlandishly inexplicable. “You need to get her to eat more,” they would say to my parents, within my earshot. The thought was that I was anorexic from nerves, and that somehow this was the correct way to handle it.
My mother had raised me within a particular mindset of the 1960s-70s feminist era, where shame about the human body is not supposed to invade our modern consciousness. Yet this openness hadn’t shelved my personal humiliation, nor had it quashed my doctors’ penchant for blaming my symptoms on me. The social movement of feminism hadn’t taken care of the scrutiny under which all women still live: under glass, like specimens that need constant judging and tinkering.
One day in my senior year of high school, after vomiting from abdominal pain, I went to the nurse’s office. She reluctantly offered me the cot, then called my parents and sent me home. What I didn’t know was that she told my stepfather I was being sent home because I was pregnant and/or “promiscuous.” Besides himself, he asked me, “Are you promiscuous?” as if the word was an actual diagnosis. The scene might have been funny, considering I’d only ever had one boyfriend, except it felt more like something out of a 19th Century novel. This is what we still do, I thought even then. When we are met with the unknown, coupled with the female body, we cry loose morals and criminal insanity.
The incident was a mere shadow of what was to come. Because by the time I was in my mid-twenties, most people viewed me as the frail, “artsy,” over-sensitive, acerbically witty girl who was often ill and probably more than a little crazy.
After college I worked as a journalist, popping xanax to get through interviews, a practice that kept my accelerating anxiety attacks only slightly at bay. I took an hour preparing to leave the house (do I have my pen and notes, my compazine and fiorinal?). One day I heard my editor on the phone arranging for a subject to meet me. He said, “What does she look like? You can’t miss her: dark eyes, real thin. She has that heroin chic thing happening.”
My house became my sanctuary from the chaos that was Me In The World, and it felt terrifying to leave it. My bookshelves were crammed with Gothic novels, and I immersed myself in them: debauched women burying their stillborns under druidic henges; cursed castles where the undead lived amongst the barely-living. Biographies of accomplished women who were labeled unstable also became increasingly intriguing to me. Claudette Colbert, Vivian Eliot, Marilyn Monroe, and Mary Tudor had all battled severe menstrual symptoms, miscarriages, “false pregnancies,” unexplained tumors, and depression. All were severely ostracized by even their own families.
It was at this point that I began to wonder if my life-long fascination with a 19th Century ideal of beauty, and women who were labeled societal outcasts, held clues that might solve my own illness.
By age 31, eating was a torture ending in something akin to stomach flu. My Regency-style wedding dress had to be made for me, because, though I was 5’8” tall, my torso was as narrow as an 11 year old girl’s. Naturopaths and acupuncturists threw their hands up at me. I spent most days bleeding profusely, and vomiting from vicodin. Though I tried, I could not get pregnant.
There was a cyst on my left ovary, then it was gone, then it mysteriously returned. My condition had grown to such an extent that both Western and Eastern doctors finally agreed it could be an actual condition.

The author with her husband, two days prior to her first surgery, in December, 2000.
Chlorosis, Hysteria, Moral Insanity, Female Morbidity: the Victorians had as many inaccurate names for it as they could invent, and committed countless women afflicted with these so-called conditions to asylums. The seven modern-day doctors I saw in two years had their own diagnoses: Chrome’s disease, colitis, panic disorder, common migraine syndrome, nervous exhaustion, dysmenorrhea, Irritable Bowel Syndrome, duodenal ulcer, follicular cyst proclivity, and general infertility.
In a magical moment of consensus, an OBGYN and a fertility specialist both ordered a laparoscopic procedure. The exploratory excursion, they said, might involve the removal of the cyst and a few microscopic clogs in my fallopian tubes. Instead, the brief procedure turned into a three-hour surgery. I was told later that a team of medical students stood bug-eyed in the theatre. The students couldn’t believe their luck. The two surgeons couldn’t believe what they saw.
Endometrial implantations had to be cauterized and cut from my exterior uterine walls, fallopian tubes, ovaries, bladder, stomach, small and large intestines, and kidneys, taking healthy tissue from each of those organs with it. Most of my left ovary was removed along with the orange-sized cyst that rendered it useless; and endometrial cells that could not be removed had to be left to fate. When I awoke, the primary surgeon leaned over, her face aghast and accusatory, and said, “You have Stage IV Endometriosis. You must have had it for years. You probably won’t have children, now.”
This is a moment that—even coming out of the haze of anesthesia—I will always remember. Not because of the unfortunate news, but because once again, even after this surgeon had seen with her own eyes what had caused years of suffering, there was a declaration of negativity that pointed at me. On my follow-up visit, the same doctor told me she didn’t want me to try and conceive right away. “Being pregnant comes with major body changes and weight gain, and for someone like you, I’d be worried about how your body image would affect you,” she said. When asked to clarify she mentioned my “anorexia.” I said, “You mean the anorexia that was caused by all those lesions you just cut out of my body?”
Endometriosis is a condition wherein cells like those in the uterus lining are found elsewhere in the body. These cells are still affected by hormone changes and may cause hormonal imbalances. They grow, then break down and bleed.
Unlike during a menstrual course, the cells have no way of leaving the body, and so remain, multiply, and form adhesions. Endometrial tissue can be found almost anywhere in the human body (in rare cases, in the brain and lungs), and can form large, blood-filled cysts. According to the World Endometriosis Research Foundation, there are an estimated 170 million sufferers wide. Women negotiate this prickly and humiliating landscape of ill health with little more than a nod from anyone, and with varying symptoms. The disease constitutes a pre-existing condition, and continued affordable healthcare can mean the difference between life and not-much-of-one.
Over the last decade, there is better research and more communication within the medical community. There is the Internet. Oxford University and M.I.T. have notably launched schools of research devoted almost entirely to endometriosis, which both institutions currently classify as an auto-immune disease. I have found doctors who are willing to take on the arduous task of managing my disease, though I have also, even recently, had to change physicians—because, even when faced with my history, these practitioners have missed recurrences, or were stumped as to what to do with new symptoms.
In part, this happens because endometriosis is one of the most mysterious medical conditions, manifesting in symptoms that are severe, to mild, to unnoticeable. Frankly, the problem is that most physicians are educated about and trained for the disease in the same way they would have been had they attended medical school in 1970.
A woman with moderate-to-severe symptoms suffers an average of eight years before being properly diagnosed. The disease itself can manifest at a girl’s first menstruation cycle, or—more puzzlingly—before it. Women with endometriosis suffer a 40% greater loss of work productivity than those without endometriosis, due to pain. Some with the disease have no pain at all, but find they cannot conceive when they try to have children. Women with endometriosis who do conceive have a higher rate of miscarriage and ectopic pregnancies.
While I’ve had three miscarriages and twice had my tubes cleared to conceive, I am also, without in-vitro fertilization, the biological mother of two—that in itself a joy as well as a curiosity. It was thought until recently that endometriosis went into remission after pregnancy (it does not). Former theories also said menopause or hysterectomy was a cure. But endometriosis has no cure.
I’ve developed a kind of internal radar, an Endometrial Sixth Sense: zeroing in on the friend who gets her period for more than a week, or the cousin who’s been put on anti-seizure medication for migraines, or my own daughter’s frequent leg pains. A friend calls me “Dr. Google.” Like so many like me, I rely on information from medical websites, published research papers, and Internet chat groups. With a fluctuating list of symptoms, diverse theories of origin, and antiquated training of medical professionals, those of us who live through this feel like characters in a House episode that never ends.
In 2008, shortly after I’d had my daughter, 30 non-endometrial, rupturing cysts caused an E.R. resident to schedule an appendectomy (thankfully, after reading my chart more carefully, a senior doctor burst into my room to cancel the procedure and order a sonogram instead). In 2010, a cyst lodged itself in the lining of my uterus while, at the same time, a fibroid started to grow outside the lining of my uterus, neither of which were said to be the cause of severe bleeding and a suddenly low thyroid count. Almost 30 years into my symptoms, I still suffered migraines, acne and skin discolorations, and panic attacks that took hold of me for no discernable reason, often in the middle of a sound night’s sleep. Sometimes, I had searing, ulcer-like pain in my abdomen, as if I’d swallowed glass.
When I asked one of my doctors whether it was reasonable to assume endometriosis was contributing to these myriad anomalies, she was silent. I was treading on the thin ice that divides what can be seen and what has to be guessed at, a territory I’m certain physicians categorically dislike.
“That, and you have a hypochondriac code on your medical charts,” a friend who’s in medical billing tells me. I think she’s kidding until she explains the code comes across her desk every day, notably with people who see many different doctors over a period of years for “mysterious” symptoms. She has checked my own chart from our local hospital (it has the code).
By 2012, it’s clear that all I have to look forward to is a tapering off in the growth of new cells, and an increased risk of reproductive cancers. Three bad pap tests, a year of missed periods, bladder pain, and a sudden weight gain of 15 pounds in my abdomen in one month (“You’re just getting older,” says my GYN), and I am once again in full battle mode: I demand a full hysterectomy, with everything that is taken out biopsied. This is easier said than done, as my current doctor prefers I go back on hormone supplements and “wait it out.”
The shock is that even a female GYN, with other patients who have endometriosis, will hold off on what is—truly, really—the only option for endometriosis, which is excision surgery. My heart in my throat—a sliver of my inner thoughts wondering if maybe I’m wrong and she’s right—I decide to switch doctors, again (doctor-hopping, it’s a code!). The new surgeon admits me three days later for the surgery I’d been begging for the better part of five years.
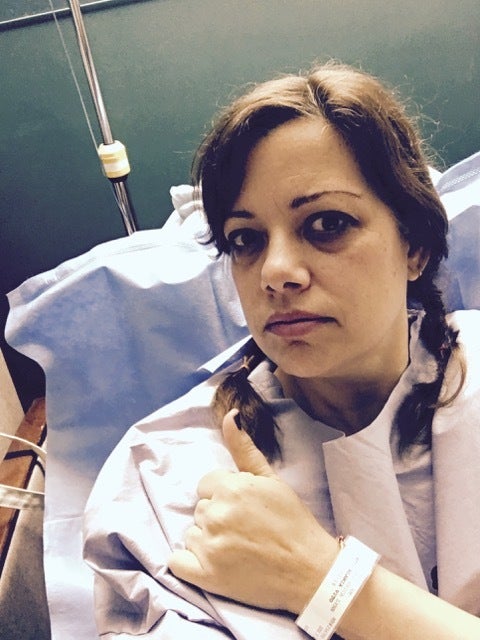
The author awaiting third and final surgery, February, 2016
It is the 18th of February of 2016, my sister’s birthday. She is five years and one day older than I, and yet she has been diagnosed with endometriosis for the first time in her life after an endometrial cyst caused severe anemia and a weeks-long flu she had around Christmas she couldn’t kick. On her birthday, I am filling out pre-op paperwork. The next day, my own birthday, I’m having blood drawn, my hospital bracelet fitted. On 21st February, I awake in the operating theatre and my surgeon, knowing how long I have waited to be told I’m not crazy, announces, “Congratulations! We found five fibroids—one about the size of a grapefruit—some other cysts, adhesions, and live endometrial cells blocking your tubes.” When I cheer a drowsy, druggy sort of cheer, the operating team laughs.
Except, I really am elated. It has been a too-long road and that road—while not over until a cure for my disease is found—has just narrowed significantly. It is no longer a wide mountainous thing with hairpin turns, but a little gravel path like in a Victorian garden, one I can manage for a long while.
The novelist Hilary Mantel, my friend who has battled this disease, has written, “It’s very difficult for me not to regard my body as my enemy. But it’s the only body I’ve got.” I think about that a lot. And I tell myself that I am not the demoralized, consumptive little girl with the sallow face and skeletal figure anymore. I tell myself: you are the gutsy female apothecary who insists on not riding side-saddle, trotting on to meet the next symptom head-on down that little garden path.

The author on Mother’s Day of this year, with her children.
