Biogen Inc.'s recent revelation of promising early data from an experimental Alzheimer's treatment is something of a breakthrough: it's the first time that we have seen positive human data about a new Alzheimer's drug that can both reduce the presence of amyloid plaques in the brain and improve cognitive function.
An estimated 5.3 million Americans are believed to be living with Alzheimer's and currently there are no FDA-approved drugs that slow or prevent the neurodegenerative disease.
In the past, despite early stage (phase 2) positive results, late-stage Alzheimer's research has repeatedly failed in expensive phase 3 tests, so when Biogen, a Cambridge, Massachusetts biotech company, announced some of the most promising Alzheimer's phase 1b results it grabbed our attention.
We routinely hear hype about potential new drugs for Alzheimer's disease. What's often missing from the reporting is the fact that these drugs are typically only at the "preclinical" stage of research. This means that a new drug is being studied in test tubes or animal models for its effect on simulations of Alzheimer's disease.
Drugs at this stage might offer great promise for patients with Alzheimer's, but they're a long way from testing in humans and any chance of FDA-approval. Biogen's results suggest that attacking amyloid may be a therapeutic strategy that could be available for patients living with Alzheimer's disease in the next few years.
The drug, called aducanumab, is a monoclonal antibody vaccine -- a large biological agent that needs to be administered intravenously, probably every month. Most FDA-approved drugs are small molecules, which can be ingested in pill form. The Biogen compound is similar to the molecules the immune system normally produces in response to infections or to clear debris from areas of injured tissue. These antibodies are very specific to their beta-amyloid target, which are involved in genetic, familial forms of Alzheimer's, and may also be involved in the senile, old-age forms of Alzheimer's.
The results that Biogen unveiled in Nice, France were the culmination of several years of costly and time-intensive preclinical and clinical research. The monoclonal antibody Biogen presented binds together amyloid plaques and crosses the blood-brain barrier.
These results are especially meaningful because the study was conducted in human populations, part of a phase 1b clinical trial. The primary purpose of the study was safety, but the company also included biomarkers of the disease and cognitive function as secondary outcomes.
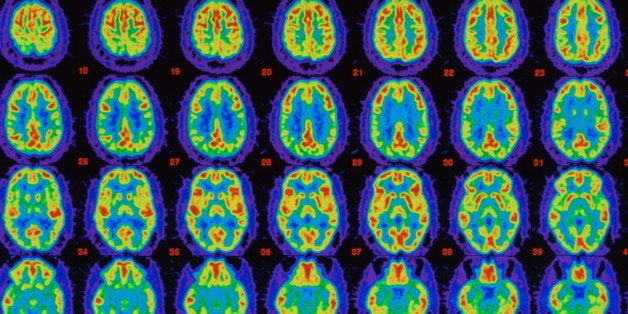
These biomarkers included Amyvid, the beta-amyloid PET brain imaging test that the Alzheimer's Drug Discovery Foundation helped to develop. The brain scan technology was used to enroll patients in the study and to ensure that they had a verifiable Alzheimer's diagnosis.
The results showed, probably for the first time in a well-designed clinical trial for Alzheimer's disease, a believable, dose-related stabilization or slowing of cognitive and functional decline. They also demonstrated the first-ever dose-related reduction in brain amyloid, suggesting that the drug was hitting its target in the brain.
The fact that the results were dose related adds credibility to the evidence that the positive clinical trial results were due to the drug rather than chance. Researchers also saw improvement on other biomarkers of Alzheimer's disease.
These are very hopeful results, but they are not without caveats. This was an early stage, phase 1b study with a relatively small number of patients. In total, only 166 patients enrolled in the study, broken into four groups of about 40 each: three groups taking different doses of aducanumab and one group taking a placebo.
For a safety study that enables a drug to move further in clinical testing, this relatively small number of patients is reasonable. But for a study designed to prove efficacy, it is too small to draw truly reliable conclusions and creates the possibility that the results happened by chance. Studies that prove efficacy in later stages of clinical research often enroll 3000 or more patients.
There were also many people who dropped out of the study because of serious side effects, especially patients in the highest dose group--the same group that had the highest efficacy rates. These dropouts confound the statistical analysis of the trial and create concerns about safety.
But none of this takes away from the fact that the results of this Alzheimer's clinical trial are the most hopeful I have ever seen.
Biogen is taking a big risk -- one that should be applauded -- by aiming to go directly from this phase 1b trial to a phase 3 trial enrolling a few thousand patients. Usually, research progresses through phase 2 trials -- which study a drug in an affected population of several hundred patients -- and then to phase 3 trials to demonstrate efficacy. Generally, the FDA requires two phase 3 trials to provide a regulatory approval. Given the scale of the Alzheimer's epidemic (and the absence of any FDA-approved disease-modifying treatments), it is possible that the FDA might grant some form of special approval if Biogen sees very positive results in its forthcoming phase 3 trial.
Science is always incremental, building on what has been done before. This clinical trial learned from previous trials by studying patients with earlier stage mild Alzheimer's disease at which time treatment might be more effective. It also exclusively enrolled patients with a positive amyloid brain PET scan to be certain they had the biological markers of Alzheimer's, rather than exhibiting only clinical indications of the disease. (Previous studies were confounded by the presence of up 30 percent of patients who turned out not to have the disease on subsequent amyloid brain scanning.)
If the phase 3 test is also positive, a pathway for the development of other new drugs for Alzheimer's based on this model will also have been established. That alone is a very important outcome for Alzheimer's drug discovery research.
