By Ms. Jo-Anna Baxter and Dr. Raluca Barac, Centre for Global Child Health, The Hospital for Sick Children (SickKids)
This week is World Breastfeeding Awareness Week - a time to draw attention to one of the most effective, yet arguably under-utilized, interventions to ensure newborns and children everywhere survive and thrive. Although it is widely accepted globally that there are many health benefits tied to breastfeeding for mothers, newborns and infants, only about a third of children are exclusively breastfed to the recommended age of six months.[1]
- Breast milk, in sufficient quantity and quality, provides essential nutrients and antibodies, preventing common infections and reducing the risk of mortality from infectious diseases.[2]
- Breastfed children score three to five points higher on IQ tests,[3] and appear to have improved intelligence test performance 30 years later--making a difference in education attainment and income in adulthood.[4]
- Breastfeeding has the potential to be life-saving particularly in low- and middle-income countries where there is limited access to sanitary resources and appropriate weaning foods.
- For mothers, breastfeeding reduces the risk of breast[5] and ovarian cancer,[6] and results in temporary postnatal infertility, helping to space out births.
- Breastfeeding is a very low cost intervention, given that it is naturally produced.
While the rate of Exclusive Breastfeeding (EBF) has improved in some countries, only 39 per cent of children less than six-months of age are exclusively breastfed in the developing world.[7] This low coverage implies that social and environmental factors may be influencing breastfeeding rates. Factors associated with the use of EBF are multiple, variable, and dependent on the families and communities.
To learn more about the factors that influence EBF, our team at the Centre for Global Child Health at The Hospital for Sick Children (SickKids) paired up with two international NGOs: CARE Canada and Save the Children, who were implementing multiple activities to promote EBF in Ethiopia and Mali as part of the Muskoka Initiative Consortium funded by Department of Foreign Affairs, Trade and Development Canada to improve maternal, newborn and child health.
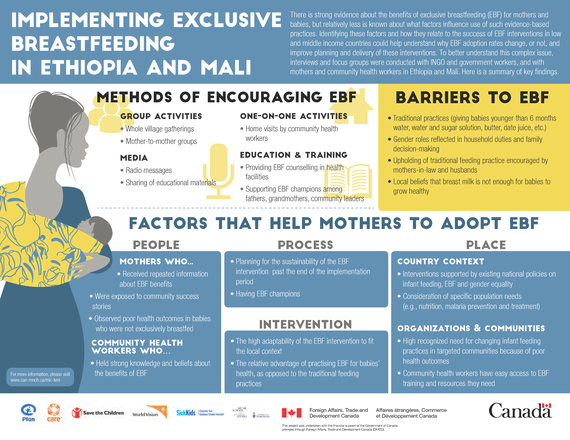
Activities included sharing educational materials, conducting counselling by community health workers during home visits and community sessions, radio messaging, and mother-to-mother groups. In both countries, EBF rates increased after approximately two years of implementing these activities. Here is a summary of the study key findings:
Identifying which factors accompany the successful implementation of EBF activities can help us in increasing the number of mothers who exclusively breastfeed their children--an important intervention with the potential to save lives.
To learn more, visit sickkids.ca/globalchildhealth.
REFERENCES
About the Authors
Jo-Anna Baxter is a Data Analyst at the SickKids Centre for Global Child Health. Since completing her MSc in Nutritional Sciences at the University of Toronto, Jo-Anna has worked on several research projects related to maternal and child health at SickKids. Jo-Anna is passionate about improving maternal and child nutrition through the implementation and effective scale up of evidence-based nutrition interventions.
Dr. Raluca Barac is a Research Associate at the SickKids Centre for Global Child Health. She received her MA and PhD in Developmental Psychology from York University, Toronto. Raluca is working in the area of implementation science, studying how evidence-based interventions are being disseminated in different sectors such as education, mental health and global health, and the factors associated with implementation success.
Follow the SickKids Centre for Global Child Health on Twitter @SickKidsGlobal.