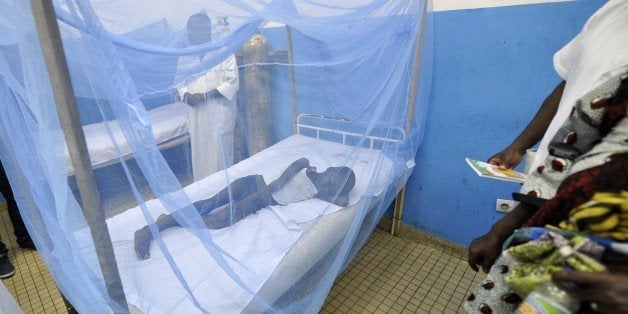
Like hundreds of other doctors from around the world, I started this year in Sierra Leone, where the national health system was near collapse amid the Ebola crisis.
My mission was unrelated to Ebola, whose rapid and lethal spread was igniting fears of a worldwide catastrophe. Instead, I was there to help shore up the country's efforts to fight malaria, which was flaring up around the capital city of Freetown.
The outbreak was centred in the same areas of Sierra Leone where Ebola was taking hold. Caused by parasites and transmitted through the bites of infected mosquitoes, malaria can kill. But, with the proper use of the right tools, it is preventable and curable.
I was 3 months into my job as Director of the World Health Organization's Global Malaria Programme in Geneva, where I was on new terrain. But my visit to Africa returned me to familiar ground. I had spent 30 years in such far-flung places as The Gambia, Tanzania and Mozambique. During that time, I had evaluated tools like anti-malarial medication and insecticide-treated bednets and learned how they could save lives.
As the threat of Ebola grew, Sierra Leone's Ministry of Health mobilized 10,000 volunteers to quell the malaria outbreak. In just a few days, working with WHO and its partners, they treated nearly 3 million people in and around Freetown -- more than 80 percent of the people in the targeted areas. Their primary weapon: a cheap and readily available combination of drugs that include artemisinin.
That work also helped in the fight against Ebola: By reducing the number of malaria cases, the campaign reduced the number of people with fever. That was important because anyone with fever required isolation to exclude the possibility that it was caused by Ebola.
Soon after, the malaria outbreak abated, and I returned to Geneva.
Last month, I flew to China. It was my first visit there, and I was impressed by the bullet trains, which race from Shanghai to Jiangsu Province at 300 kph. I was also impressed by the country's speedy advances against malaria, which have reduced its incidence from 27 million in the early 1970s to about 50 so far this year.
Instead of easing up, the Chinese authorities are focusing now on completing the job of eliminating the disease within their borders and preventing its reintroduction.
Such advances are not unique. This year is on track to mark the first in which the European Region tallies zero new cases of malaria. The former Soviet republics of Uzbekistan and Kyrgyzstan reported zero indigenous cases of malaria last year.
Some countries are making great strides against malaria, despite great obstacles. The Democratic Republic of the Congo is marked by civil unrest and a primitive communications network. Still, health workers last year deployed enough insecticide-treated bednets and medication to exert a profound impact. Though DRC still has a high rate of malaria, its 50-75 percent rate of decline is among the steepest in the world.
How can we apply the lessons we are learning in individual countries to a unified plan to end malaria? We cannot -- and should not. When it comes to malaria, one size does not fit all. What may work in Jiangsu Province may not work in Kyrgyzstan or Congo.
When fighting malaria, we first need to understand the context, the biology, the ecological factors, the health systems and the responses of the parasites in each region of each country. Then, we need to tailor our response to the locale.
Luckily, we have powerful tools at our disposal. In addition to bednets and medication, we use indoor residual spraying of insecticides to kill mosquitoes.
And we use locally available technologies, such as cell phones, to improve our reporting and determine where to focus our resources. Some of the interventions are even less complex -- we teach people to get rid of standing bodies of water, where larvae can grow.
But continued progress is threatened. Many parasites are becoming resistant to the medicines, and mosquitoes are becoming resistant to insecticides. We need new prevention and treatment tools, which must be delivered through a robust research and development effort.
This week, WHO is launching the World Malaria Report, an annual publication that tracks global progress in malaria control and elimination. Our report shows a 37 percent global decline in malaria incidence and a 60 percent decline in malaria death rates over the last 15 years.
Among children under 5 years of age, death rates have fallen by 65 percent. An estimated 6.2 million deaths have been averted since 2000.
Target 6C of the Millennium Development Goals -- which aimed to halt and reverse the global incidence of malaria between 2000 and 2015 -- has been achieved.
But there remains a massive, unfinished agenda. An estimated 438,000 people will die of malaria this year, versus about 13,000 who will die of Ebola. As health leaders -- including many of us here at WHO -- rightfully debate how to prepare for the next health crisis that may emerge, we should take pains to ensure that we continue to make progress against the diseases we already know much about.