
When Helen Chen was working toward a master’s degree in public health, she thought of cancer dismissively as an “old white man’s disease.” Shortly after receiving her degree in 2009, she was diagnosed with breast cancer at the age of 27.
This month, Chen celebrated what she calls her “cancer-versary,” marking a tumor removal in July 2010. She recalled that after her diagnosis, she learned that an aunt had had breast cancer too ― but chose not to discuss it with Chen or other relatives.
“It seemed like my family had this deep sense of shame,” Chen, who is Taiwanese-American, told HuffPost. “With Asian families, you just don’t put your shit out there. This is not stuff people want to hear about.”
Chen lives in California, where the breast cancer rate among Asian-American women has risen over the past 15 years, according to a new study by the Cancer Prevention Institute of California. Other U.S. racial groups have seen their rates level out or decrease.
The study was the first to analyze seven major Asian-American ethnic groups ― Chinese, Japanese, Korean, Filipino, Vietnamese, South Asians (Indians and Pakistanis) and other Southeast Asians (Cambodians, Laotians, Hmong and Thai) ― by age and stage of cancer. The data came from nearly 46,000 invasive breast cancer cases in California, which has the largest Asian population in the U.S.
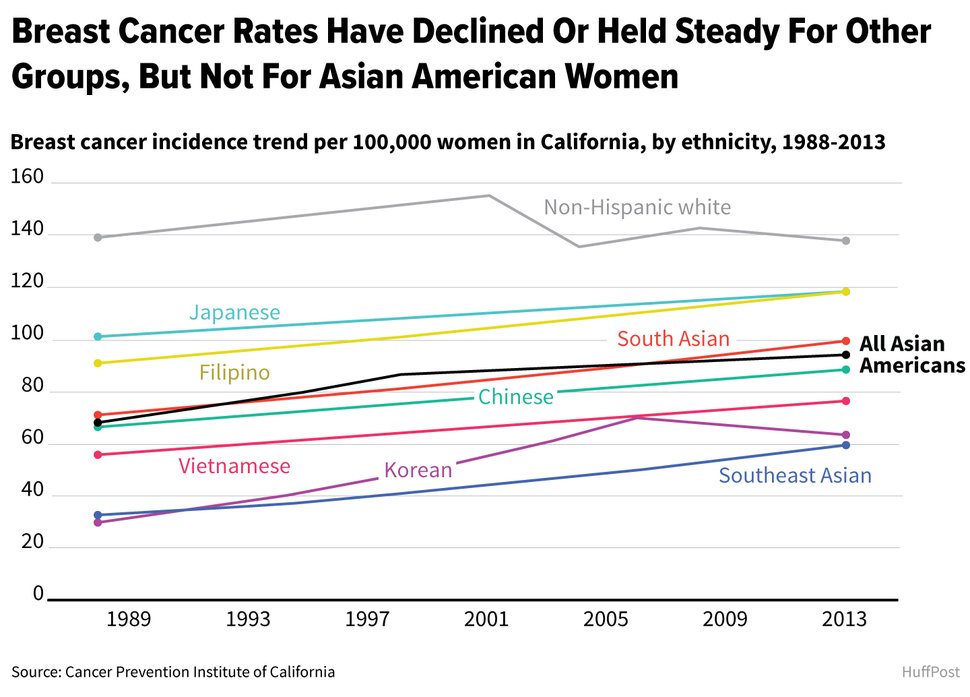
The chart below, which shows incidence of breast cancer per 100,000 women between 1988 and 2013, indicates that rates went up for all the Asian-American groups. The rate increase for Japanese women alone was not statistically significant.
Korean women had the greatest rate increase from 1988 to 2006, at 4.7 percent per year, after which they experienced a slight decline through 2013. Over the full period studied, the rate rose about 2.5 percent a year for Southeast Asians and 1.4 percent for South Asians.
The Reasons Why
Scarlett Lin Gomez, a research scientist at the Cancer Prevention Institute of California and the study’s lead author, said the reasons for the rate increases require further research. The stigmatization of women with breast cancer within Asian communities that Chen noted might play a role, Gomez said, because it keeps some women from learning about their genetic risk factors.
The rise in breast cancer may also be related to “Westernization,” said Gomez, who is Chinese-American.
She pointed out that the Asian-American populations with the largest increases are among those who have more recently immigrated to the U.S. in significant numbers. Chinese and Japanese women ― two groups that have lived in the U.S. longer ― saw lower or no increase.
Many of the established breast cancer risk factors “are related to what we think of as acculturation, Westernization,” Gomez said. There are “things that we might be more or less likely to do differently living in Asia versus living in the U.S.” She pointed to such risk factors as drinking more, eating a typical American diet, being obese, getting less exercise, having children later in life and having fewer children.
For instance, “soy intake during earlier stages in life might be protective against cancer,” Gomez said. And soy products are much more widely eaten in Asia than the U.S.
The American Cancer Society states that the main risk factors for breast cancer ― gender, age and genetics ― are out of patients’ control, but there are lifestyle choices that may increase your chance of developing breast cancer.
‘We Just Don’t Examine Ourselves’
When Betty de Guzman learned at age 62 that she had stage 3 breast cancer, she asked her sister what that meant. Her sister had had a double mastectomy years ago but the two had never talked about it. Her sister had simply given her a book about cancer. After de Guzman’s own diagnosis in 2001, she made a point to re-read the book.
De Guzman discovered she had breast cancer shortly after immigrating to the U.S. from the Philippines. She told HuffPost there simply wasn’t much awareness among Filipinos or Filipino-Americans about the disease.
“We just don’t examine ourselves, you know?” said de Guzman, who had 14 lymph nodes removed in August 2001.

De Guzman observed that the silence among Filipinos may be based in part on a belief that patients might be “deserving” of their fate.
“Many Filipinos believe in superstition,” she said. “They are afraid to come out about it because it would seem they had done something to deserve it. They want to hide it. They’re ashamed of it.”
Asian-American immigrants from some areas may also lack the knowledge about available treatment options and medical advances, Gomez said.
“Access is a big part of this ― not knowing what kind of access is available,” Gomez said. “More education and more awareness needs to be made around that.”
She would also like to see more discussion within families. “I would like to see it not become a stigmatized topic,” she said. “It’s OK to talk about. And there’s an importance of family history.”
Certain misunderstandings about breast cancer are still too common within the Asian-American community, Gomez said, including that the diagnosis is a “death sentence” and that if a person is asymptomatic, there’s no need to see a doctor.
“With regard to barriers to screening, some people think, ‘If I don’t feel anything, why do I need to see a doctor?’” she said. “The issue is obviously by the time you feel something, the tumor may be more advanced.”
‘A Patient Can Fall Through The Cracks’
At the same time, Asian-American women are less likely to receive followup treatment after an abnormal mammogram, according to a new study from research scientist Kim Hanh Nguyen and Dr. Leah Karliner of the University of California, San Francisco.
They evaluated data for more than 50,000 women in the San Francisco area between 2000 and 2010, publishing their results in Cancer, a peer-reviewed journal of the American Cancer Society.
“We are surprised at the extent of the delay,” Nguyen said, given the importance of receiving timely care.
The researchers found that only 57 percent of Asian women were receiving followup tests at 30 days, compared to 77 percent of white women. Asian women were also less likely to have followed up after one year. The study did not evaluate black and Latino women.
Their data also varied widely across Asian ethnicities, Nguyen said. Pacific Islander and Filipino women, for example, were 20 to 60 percent more likely than white women to receive a late-stage cancer diagnosis, whereas Chinese and Japanese women were 30 to 40 percent less likely to receive such a diagnosis.
The causes, Nguyen suggested, range from basic barriers to medical care ― including language, lack of transportation and lower insurance rates ― and cultural issues such as not wanting to trouble friends or family members.
“Patients may have their own personal feelings of not wanting to burden the family ― maybe after 30 years of not being able to speak the language and get their own services,” she said.
The larger health care system is partly to blame, too. Nguyen pointed to the fact that providers don’t easily talk to one another or share medical records.
“In a fragmented and uncoordinated system, a patient can fall through the cracks,” she said. “That could really affect how her cancer journey turns out.”
Attacking From All Sides
The next research step, Gomez urged, should be studying the nuances across patients’ cultures. She said it’s critical to study different Asian groups with regard to when they immigrated to the U.S. and compare them to women still living in Asia.
Among health care providers, Nguyen said there’s a need for more staffers who possess not only diverse language skills but also awareness about cultural backgrounds and who have been trained in outreach. Clinics that serve sizable Asian populations should ensure they have robust monitoring and tracking processes, she said.
On the advocacy level, Chen is speaking up personally and professionally. “My voice is underrepresented and missing, but I take part whenever I can now.”
She called for Asians to participate in clinical trials for breast cancer research. She’s also working to make sure younger women are informed about the risks of breast cancer. She coordinates outreach across the Bay Area as an educator and a facilitator.
But advocacy begins at home, she said.
“My cousin got diagnosed with stage 3 [breast cancer], and she’s a physician,” Chen said. “It was the awareness of my experience though that made her go to the doctor.”
Learn more about breast cancer screening here.