On Dec. 16, 2011, my 27th birthday, my husband and I excitedly went in for our big mid-pregnancy ultrasound, happily expecting to find out if the twins I was carrying were boys or girls.
We invited my parents, planning to go out for a celebratory birthday lunch afterward. Twin ultrasounds take a while, as I well knew at that point, but this one really began to drag on.
As I sat, belly covered in jelly on a table in that darkened ultrasound room, I heard the tech say, “I’m going to go get the doctor. I see some problems with Baby B’s head and spine.”
My jelly-covered belly began heaving with sobs that I tried to stifle as the maternal-fetal medicine expert arrived and attempted to get a better look at Baby B.
As she examined the baby’s “lemon-shaped” head and looked at her spine, she saw the unmistakable signs of myelomeningocele spina bifida, the most severe type of the neural tube defect.
That day, sitting on that table, I had no idea what myelomeningocele spina bifida meant for Baby B, the twin on top, whose head so frequently found itself resting on the outside of my ribs, stretching my skin so taut I could cup her skull in my hands.
I didn’t know if the doctor was telling us our baby would live or die. I didn’t know if she would walk or talk. I didn’t know if it would affect her twin sister, Baby A, the twin on the bottom, deep inside my pelvis, whose hiccups I often felt in my crotch.
I was led, still sobbing, into another room, the light blinding after the dark of the ultrasonography suite. Genetic counselors were brought in. My obstetrician came in to tell us she had looked at the scans with the maternal-fetal medicine expert, saw me sobbing and gave me a big hug. She explained the situation and promised to call me the next day, a Saturday, when we had had some time to process and might have more questions.
We went out for a very awkward birthday lunch. When we got home, I collapsed into bed, hugging my belly as I cried, and slipped away for a tear-stained nap.
The biggest thing I learned that day is that the ultrasound between 18 and 22 weeks of a pregnancy isn’t just the happy day when you get to find out if your baby is a boy or a girl. It’s also the point that can turn a very much wanted pregnancy into heartbreak. It’s the point where, peering at fuzzy images on a black-and-white screen, doctors can finally see the anatomical information that reveals something severely wrong with a baby. It’s the point where genetic counselors are brought in and “options” must be discussed.
Because of the worst birthday of my life, I take it a little bit personally when I see legislators and columnists like David Brooks talking about banning abortion access at the 20-week mark. For us ― and for many other sobbing women with jelly-covered bellies ― 20 weeks was the exact point at which options became painfully necessary.
In the end, our baby’s diagnosis was manageable, and we decided to continue the pregnancy. Her twin sister disqualified us from the amazing fetal surgeries now being performed to correct spina bifida defects in utero, and we had to wait 15 more weeks to see what those fuzzy sonograms really meant.
Our baby was born with a large portion of her spine exposed, her head enlarged by fluid trapped there as a result of her spinal cord being pulled down and blocking her cerebral spinal fluid from flowing in and out of her skull as freely as it should.
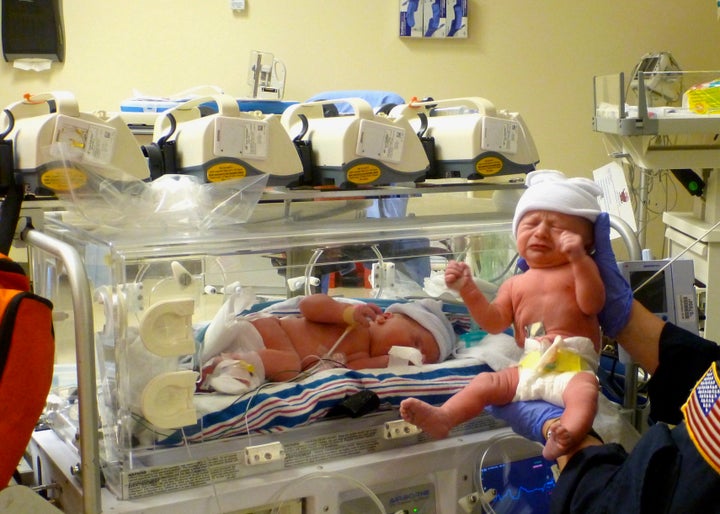
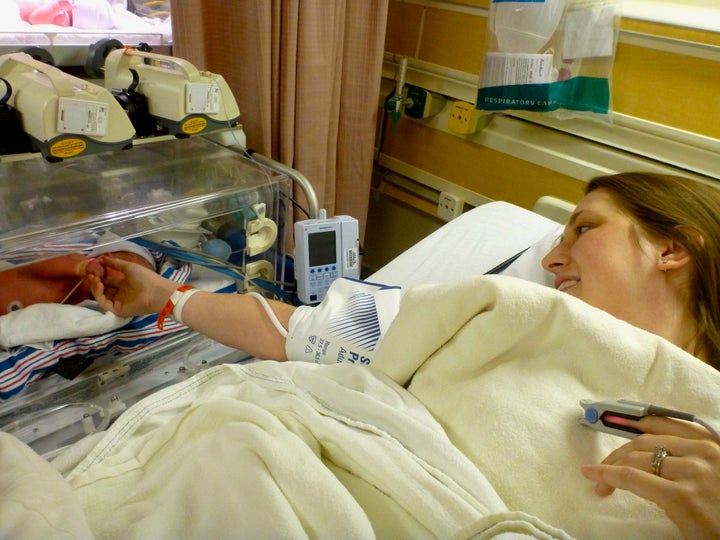
I did not get to hold her on the day she was born. She was placed into an incubator, and I held her hand and told her I loved her before she was whisked away by a transport team to a nearby children’s hospital where she would have her spinal defect surgically closed within 24 hours of her birth, just as we had begun planning for after that fateful diagnosis day.
I understand that abortion opponents like to use cases like mine to support their bans. After all, didn’t I decide to continue my pregnancy after the diagnosis?
I feel lucky that our diagnosis was manageable, that we had and continue to have access to great health insurance to get me and my daughter the health care we needed then and still need today. I feel lucky that my partner was able to take paid time off work for the two months after the birth that the babies and I needed care following a complicated delivery.
I know that any number of factors could have made our choice a much different one, and I will fight for everyone to have access to the care they need to make the right choice for them.
Twenty weeks should not mark the end of a pregnant person’s options. Abortion, fetal surgery, plans for care for special needs, further testing ― all can become necessary because of the things revealed on an 18- to 22-week ultrasound. I look back on my sobbing self that day and feel love and compassion for that new mom faced with heartbreaking news, already having to make tough choices for a baby who isn’t even born yet.
I also feel nothing but love and compassion for anyone else making the choice to terminate after 20 weeks, whether because of a lack of access to providers, lack of insurance coverage, lack of funds for care or travel, or any other reason. Every pregnant person deserves access to a full range of care, not a cruel ban arbitrarily imposed by legislators who will never know what it feels like to be sitting on that table.
