
Senators John McCain and the late Ted Kennedy
News of Senator John McCain’s glioblastoma diagnosis threw me back to intern year of residency training – a moment I remember vividly. In June 2008, I learned that “a senator was admitted for brain cancer treatment.” The hospital was Duke Medical Center. The senator was Ted Kennedy. The next day, I read, “The Senator is battling bravely. His family is at his bedside.” ‘Battle’ metaphors can be a troubling double-edged sword because I know how powerfully language can impact patients and their loved ones – particularly those with devastating diagnoses.
Having lived in Boston for several years before medical school, life was essentially all things Kennedy, all the time. In spite past controversies, I knew Kennedy had devoted his life to public service, and that he was truly beloved by the people of Massachusetts and beyond. But what I remember most are photographs with his son, Patrick; stories about his famous brothers; and the closeness of this larger-than-life family. All the more reason why this diagnosis must have been crushing.

Left: The late Senator Kennedy with son, Patrick. Right: Brothers at the White House, 1963. Attorney General Robert F Kennedy, Senator Ted Kennedy and President John F Kennedy. �
Over the course of my intense residency training, I learned about several “deadly diagnoses”: diseases you never want to get. Pancreatic cancer, biliary cancer (a.k.a. cholangiocarcinoma), idiopathic pulmonary fibrosis (IPF), amyotrophic lateral sclerosis (ALS). And glioblastoma multiforme (GBM or glio). Highly aggressive tumors, glios are typically resistant to conventional treatment, i.e. surgical resection, radiation and chemotherapy. As a result, prognosis remains dismal: according to the National Cancer Institute, 60% of individuals diagnosed with GBM are likely to die from the disease. Most die within 15 months, and prognosis worsens with age.
When I heard that Senator McCain was diagnosed with the same malignant tumor that killed his fellow senator and friend, my heart sunk. The “Maverick” can “battle” anything, people said. Impressive resume thus far: prisoner of war, malignant melanoma, and countless contentious arguments on Capitol Hill. Yet in spite a C.V. of toughness, my medical training has taught me a harsh lesson: as doctors, we should display optimism but never provide false hope. Warrior language, unfortunately, can contribute to the latter.

A young John McCain, Lieutenant Commander, in the U.S. Navy.
I believe that phrases such as “he’s a fighter” or “she’ll battle this disease” should be used with caution. Ted Kennedy and Beau Biden – as well the nearly 10,000 Americans who died from GBM in 2015 – succumbed to this relentless disease. Did these individuals not fight hard enough? Or were they simply up against a deadly behemoth of a disease? Yes, sometimes David wins, but not when Goliath is armed with insurmountable superpowers. Symptoms from glioblastomas are daunting enough – vomiting, headache, seizures. But treatment side effects can be downright unbearable: pain, weakness, oral ulcers, hair loss, nausea. Just as bad, I feel, is the emotional toll on family members who are by the bedside, in rehab, providing support, administering medications, while answering myriad phone calls from concerned friends.
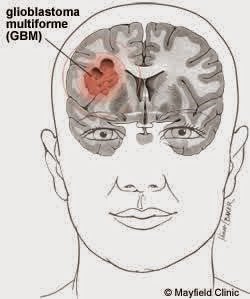
Glioblastoma, a rare but aggressive cancer, represents 15% of all brain tumors.
As a doctor, I’m always mindful that during the patient’s illness, the family is suffering, too. I remember walking into the waiting room outside the Duke Intensive Care Unit, preparing to deliver unpleasant news to a family whose grandfather was critically ill. His elderly wife faced the ceiling, repeatedly whispering “Please, God, help him.” His banker son was nervously pacing the hall, awaiting any news. And his college-sophomore granddaughter sat silently on a chair, nervously wringing her hands. The agony of granddad’s illness was painfully evident. I knew my words needed to be carefully chosen, dosed with comfort, compassion and realism.
I’m not completely against ‘warrior’ metaphor. Many of my patients “battle” lupus and liver failure, and they feel empowered by this analogy. It depends on the patient, their support system and the disease. But I do believe in managing expectations. Military symbolism – when up against deadly diseases – can create the perfect breeding ground for profound disappointment and even depression. As health professionals, we should remain hopeful. But we must also be honest with the details of the disease, including prognosis.
I’m certain that Senator McCain’s team at the Mayo Clinic have provided up-to-date information while setting expectations. I might start a conversation this way: “While glioblastoma is difficult to treat, new therapies may prolong lifespan including brain tumor vaccines and electric field oscillation.” Followed by honest reality: “In spite these therapies, prognosis remains poor. But we will do everything we can to treat the cancer, while also respecting your family’s wishes.” Let’s try our best to be authentic, hopeful and use supportive language that honors the patient and their family.
