I never thought I’d become a mother. The idea of handling someone else’s bodily fluids as, like, a day job, was abhorrent to me. And yet, at 29, I found myself walking across a graduation stage to shake George W. Bush’s hand after receiving my Ph.D. ― all while very, very, cumbersomely pregnant. In fact, security had to make an exception and allow me to have a bottle of water (not much was allowed in with a former president around, and all) because I ― or, well, my uterus, rather ― kept threatening to go into labor.
I often describe May and June of 2015 as the months I gave birth twice, first to a dissertation on the social impact of infectious disease and then six weeks later to my first daughter.
My two June 2015 births (especially the second one) left me with a surprising psychological artifact ― a very cheesy but very real feeling of connection with other mothers. Most women I ask about this feel similarly. You see another mom struggling to get a planking 2-year-old into a car seat, and you get it. You can almost feel the bottled frustration rising vicariously in your own pulse.
I spent the first few months after my daughter’s birth entranced by the way my role as a mother lent me an insight into other women’s experiences that crossed geographic and political boundaries. Are you in ISIS and a mom? Then I suddenly, out of the blue, understand a vital part of your existence and priorities. Do you drive a Volvo and carry Louis Vuitton while I struggle to pull together a decent ponytail with one hand while steering my grandma’s old minivan with the other on my way to teach my college classes? If you’re a mom, I can still relate to you in a multitude of ways that didn’t exist before June of 2015.
When I really get in my feels about it, the urge to wink and finger-shoot at every other mom I see is palpable ― and weird. This is how my first birth ― the dissertation ― relates to this feeling of connection.
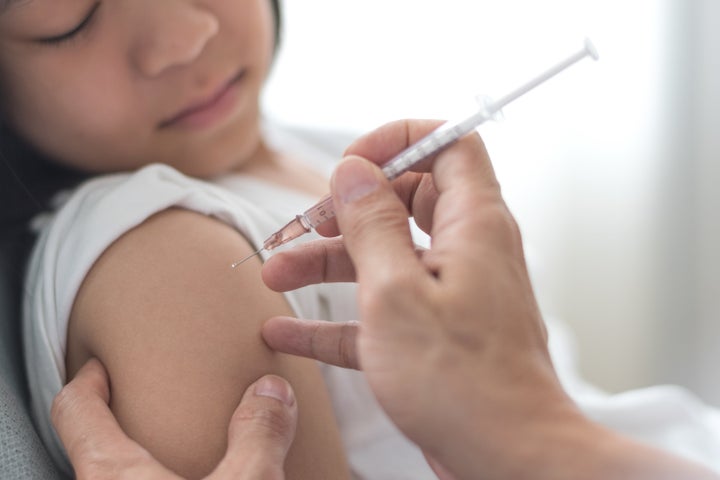
My graduate work, coming out this year as a book published by State University of New York Press, tracks the various ways that contagious disease shapes families and relationships. No book on contagious disease can be written without addressing vaccines, and so, I consider myself a vaccine researcher not because I’m at a lab bench each day making vaccines, but because I spent nearly a decade in school reading the tragic stories of loss that ultimately led people to make vaccines.
These stories are real for me, as real as they’d be if I witnessed any living person today hold their baby and watch it die. I have a phrase I use in vaccine arguments: “Until you’ve had to read as many accounts of women holding their babies while they died as I have had to do, you don’t get to say vaccines are the dangerous thing here.”
But I don’t want to alienate you. I say you, because I hope at least one vaccine-hesitant mother reads this and pauses a moment. Maybe I can change one mind, soften one heart bristled with maternal protectiveness. Because remember that thing? That cheesy universal connection to other moms? Yeah. It applies to me and you.
So I’m not going to come at you with witty phrases and condescension. As I teach my medical humanities students in a series of ethnographic labs ― change doesn’t happen there. Change happens when we can listen, pause and think.
Nevertheless, I do wish more people could encounter these century-old narratives of bereaved mothers. The Victorians were absolutely amazing empirical observers of disease. Their records show us not only maternal agony, but also just how fully infectious diseases had society over a figurative barrel, and ultimately, why people were driven to fully develop vaccination technology ― which came with its own risks even then (much greater risks, in fact, in the pre-antiseptic days, when any medical procedure could result in blood poisoning).
But the science doesn’t seem to be the linchpin that will change this debate. The science is convincing, and if that’s what we were really talking about, I think the discussion would be over by now.
The more I mull over the issue, the more I think vaccine resistance is really about the complex braid of privilege, trust and risk assessment. We are ironically privileged because of vaccines to live in a world where only specialized experts know vividly what these diseases do to bodies ― the bodies of people we love.
It bears noting that there is a contingency of vaccine-hesitant parents who are people of color and whose resistance is based not on privilege but instead on stark awareness of systemic racism and its long, long history in medical technologies, and to whom my argument does not apply. However, research also tells us that vaccine resistance is frequently situated in privileged, white families ― families who have time and leisure to panic about infinitesimally small risks that may exist in vaccines.
This data makes sense to me ― if you’re worried about where your baby’s next meal is coming from, you probably aren’t thinking about vaccine insert warnings. I should note here that autism is not one of these risks, for which we now have ample evidence that need not derail this essay.
It is only in a culture that rarely witnesses tetanus, polio or the measles that the infinitesimal risks held in the vaccine itself could seem to outweigh those of the diseases they were created to fight. It’s easy not to fear tetanus when you’ve never seen anyone die of it, and so the “toxins” you worry might be in vaccines become more important.
My research into our social past of reacting to diseases has shown me that the Western world is a risk-averse society. Advancements in technology and medicine have led us to the astoundingly privileged belief that risk should not exist in our sphere ― that if we can identify risk, we can extinguish it entirely and that we are entitled to live a risk-free life.
Statisticians and fantasy-free common sense would tell us this is impossible, of course, but it is nevertheless one of the fundamental structuring elements of life in the U.S. today. Risk labels appear on everything from medicine to ironing boards. Screenings for cancer and pre-cancer (will pre-pre-cancer exist eventually?) expand continually, even as hypertension has become a disease in its own right, rather than a noteworthy risk factor for later heart disease.
The past 30 years has seen an unprecedented shift away from a model of medical authority where doctors are respected as sole players when it comes to knowledge of the body. This shift in medical authority has left us with a society that feels privileged enough to completely avoid risk, but doesn’t know where to turn or whom to trust to help them avoid it.
No one would argue ― least of all me ― that it’s anything but wonderful that patients now have more access to information and a voice in their own health care. This comes with a fallout, however; doctors’ input is more often than not these days a second opinion, following personal (and likely imperfect) research relying on anecdotes through one’s social network and online data that is often less than helpful thanks to liability concerns.
We can’t trust, but we want solutions; we feel privileged to health and wealth, but we mistrust the avenues through which this has traditionally come to us; we want a life without risk, and our privilege has taught us that we are owed this, but reality doesn’t accommodate such fantasies. And so, our protective maternal instinct clings with fury to what seems to us the least risky path ― said path already informed by whom we have deemed trustworthy for information about this risk.
What seems to be getting lost in our cultural memory is that there are huge risks to not vaccinating ― risks that ripple outward from the unvaccinated individual to the local and global community. Immunity to disease is pretty useless if only a few people have it, and the most vulnerable of our society ― the very young, the very old and the very ill ― rely on broad disease patterns for protection. So, any sense that not vaccinating protects one child from potential harm ignores the great risk this stance poses to others.
We have lost interest in, and really any connection to, the idea of a greater good for the global community outside our own walls. Many cultures can’t understand the white, Western idea that we should care only for our own children ― a great proportion of the world views children as a community interest: the future of us all. This goes hand in hand with a sense that we should all protect all children. This, I would suggest, is a view of risk that has checked its privilege.
If we start from a perspective that there is more to mama-bear-protect (and believe me, I know the deep, deep, I-would-die-for-this-child feeling) than only our own children ― if we could think a little bit more broadly about the mother next to us, who also chokes down the I-would-die-for-this-child feeling every morning before sending her child off to school, gritting her teeth and pushing through her deep-down awareness that she can’t ever protect him fully ... then, we might have a start.
If we could begin to check our privilege and see our fellow parents as what they are ― equally as desperate with longing to protect their babies as we are ― if we could embrace that feeling with empathy, we would by definition want to protect their babies as much as our own.
Doing that, of course, means letting go of the belief that we are entitled to control all outcomes, and our belief that we are somehow owed a life without risk. It means looking broadly to what’s best for the planet, for all the families and mothers and fathers and babies that inhabit it. It means trust. Trust that we may not know what’s best, but someone else, for the moment, might; trust that the great beauty of the world is that we have different moments of “knowing best,” which allows for collaboration and community-building. If we can empathize fully with the universality of that gripping parental love, we can begin to trust even more.
If we could get to that place, we could, I think, learn to trust that a little risk may protect a greater good because we could trust, in spite of any personal doubts we might have, that the mothers and fathers around us also care about our interests and protecting them. Life is risk. To live means to be at risk of dying, and since we will all die, we can only choose how we will live ― in collaborative community, or in fear and isolation.
So let’s change this conversation. Forget the arguments over numbers. Forget the mom-shaming that surrounds all parenting debates. Start by checking your privilege. Then move on to caring about widespread risks to children, not just your own.
Finally, trust. Trust people to strive for the common good alongside you and to develop concern for all children along with you. Trust that we have centuries of stories about how horrible these diseases are, even if you haven’t seen it with your own eyes. And trust that treatments like vaccines developed out of a genuine desire to further this collective good, even before profits were involved. Trust the urgency of these historical narratives, urgency from mothers long dead, but whose experiences were very real and often very tragic; these are the experiences that resulted in vaccine technology and gave us the privilege of living in a world with drastically lower infant mortality rates.
And trust that moms like me get it. We get that you love your baby. We are connected in that fearful and desperate love. If we can keep sight of that connection, we can learn to trust one another and accept solutions that may have small risks, yes, but serve a bigger purpose.
Do you have a compelling personal story you’d like to see published on HuffPost? Find out what we’re looking for here and send us a pitch!
