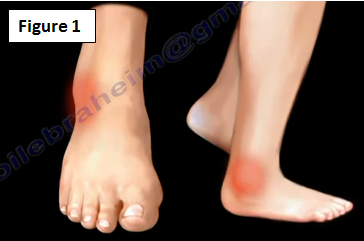
The patient will come to the doctor with a complaint of the ankle frequently "giving way" and the feeling of the ankle being unstable with pain (Figure 1).
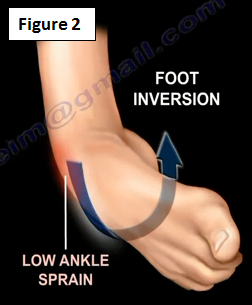
This condition can be caused by lateral collateral ligament injury of the ankle; however, it may be caused by multiple other factors. Ankle sprain is a common injury that occurs with sports activities and the lateral ligaments are the most commonly injured ligaments in the ankle (Figure 2).
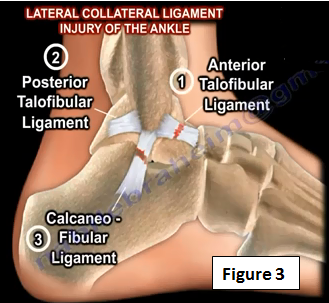
There are three ligaments on the ankle joint on the lateral side (Figure 3). The anterior talofibular ligament is the weakest of the three ligaments. The integrity of the anterior talofibular ligament is tested by performing the anterior drawer test. The posterior talofibular ligament is the strongest of the three ligaments. Injury to the calcaneofibular ligament usually occurs after injury to the anterior talofibular ligament. The integrity of the calcaneofibular ligament is tested by performing the talar tilt test.
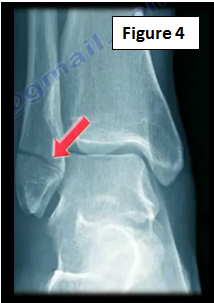
If the patient cannot bear weight after what is a suspected ankle sprain, then the physician will need to get an x-ray to check if the patient has a fracture (Figure 4).
Acute ankle sprains are usually treated by immobilization, ice, physical therapy and rarely surgery. Sometimes these ligaments do not heal and become incompetent. Incompetence of these ligaments may create chronic lateral ankle stability.
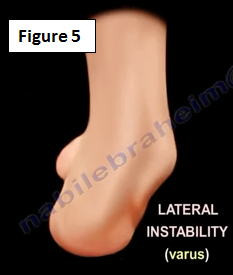
The physician may want to examine the hindfoot for varus malalignment (Figure 5). Occult varus may lead to treatment failure. The physician should check for peroneal muscles and tendon weakness, which is a frequent cause of lateral ankle instability. If the physician finds that there is hindfoot varus, they may need to do the Coleman block test to differentiate between fixed and flexible hindfoot varus. The treatment will be different.
Treatment
The majority of ankle sprains will heal with time and are treated with rest, and physical therapy including peroneal muscle strengthening with proprioception and range of motion of the ankle. In some cases, the patient may not get better and may have mechanical instability or functional instability. The patient may not improve with conservative treatment and may require surgery.
What type of surgery may be necessary?
An anatomic repair (Brostrom procedure) is the direct repair of the attenuated ligament. An anatomic repair (modified Brostrom procedure) is the direct ligament repair with augmentation using the inferior extensor retinaculum. A graft can be used if the Brostrom technique fails.
For chronic lateral ankle instability, we also need to look for other conditions such as peroneal tendon pathology, fractures, joint lesions, or arthritis. There are a lot of differential diagnoses for this area that can create ankle instability! These are some of the other causes that can create the same symptoms of pain and instability of the lateral ankle.
When the pain is located posterior to the fibula, you can blame this on peroneal tendon pathology.
Peroneal Tenosynovitis
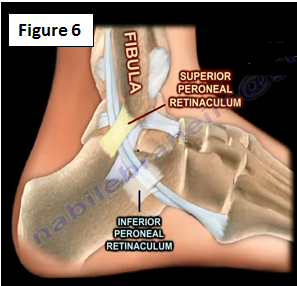
The peroneal tendons are subjected to excessive repetitive forces causing pain, swelling and instability of the lateral ankle. This is treated by an injection or possible surgery (synovectomy). The superior peroneal retinaculum is usually holding the two peroneal tendons behind the fibula. The inferior peroneal retinaculum is not as important as the superior peroneal retinaculum (Figure 6).
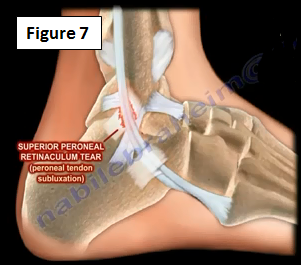
Superior Peroneal Retinaculum Tear may lead to subluxation of the peroneal tendons (Figure 7). Physical therapy or reconstruction of the superior peroneal retinaculum can be performed. Peroneal tendon subluxation occurs with dorsiflexion and inversion; however, it is tested with dorsiflexion and eversion against resistance.
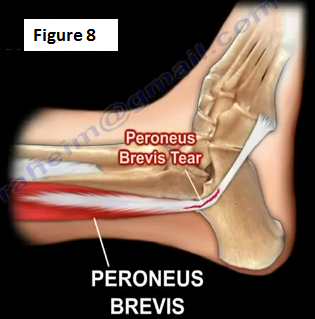
Peroneus Longus or Peroneus Brevis Tendon Rupture or Tear may occur at the peroneal tubercle with the Os Peroneum migrating proximally. Tears of the peroneus brevis may occur with peroneal tendon subluxation (Figure 8). In these cases, a repair or tendodesis of the torn tendon will be done.
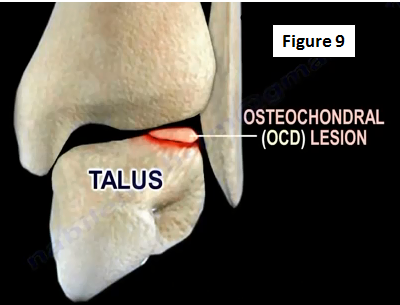
Lesions Inside the Joint are called osteochondral (OCD) lesions (Figure 9). There are two types of OCD lesions: posteromedial and anterolateral. Conservative treatment for OCD lesions includes NSAIDs and physical therapy. An ankle arthroscopy is the surgical treatment option. If the OCD ligament is less than 1 cm, then the surgeon will do an excision, curettage or drilling of the lesion.
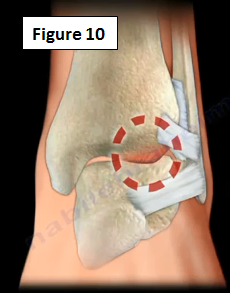
Anterolateral Impingement is the painful limitation of full range of ankle motion due to osseous (bony) or soft tissue pathology (Figure 10). Soft tissue thickening is commonly seen in athletes with prior trauma that extends into the ankle joint. The treatment includes physical therapy, injections and arthroscopic debridement of the impingement.
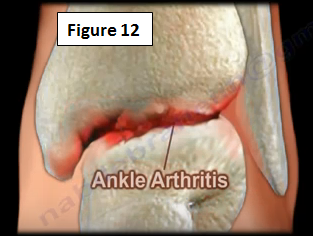
Arthritis of the Ankle Joint usually results from prior injury or inflammation to the ankle joint (Figure 12). It can be diagnosed by an exam or by an x-ray. The physician will begin with the conservative treatment of a brace and injections. If the conservative treatment fails, an arthrodesis or total ankle surgery will be needed.
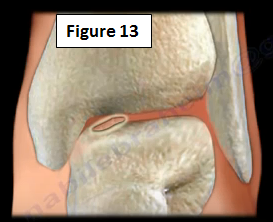
Loose Bodies within the Ankle Joint will need to be removed from the ankle when present (Figure 13).
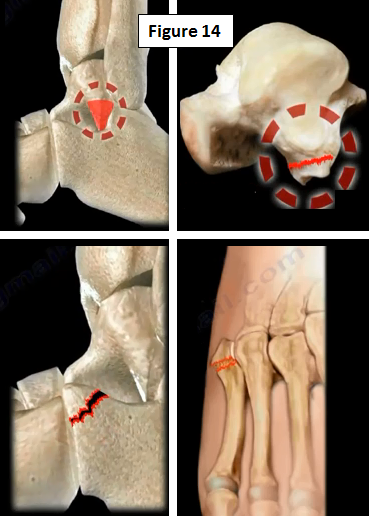
There may be some fractures that cause instability of the ankle including a lateral process fracture of the talus, anterior process fracture of the calcaneus, Jones fracture or Pesudo-Jones fracture (Figure 14). The treatment is specific for the type of fracture.
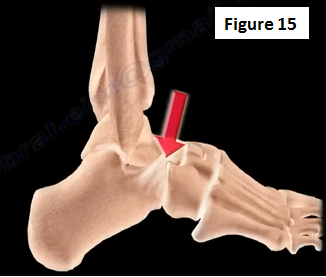
Tarsal Coalition needs to be diagnosed and treated accordingly. Tarsal coalition may cause frequent ankle instability (Figure 15).
For more information on ankle injuries, follow the links below:
https://www.youtube.com/watch?v=6aF-PIYDxF0
https://www.youtube.com/watch?v=dI4ntssi4bs
https://www.youtube.com/watch?v=c7QewW3Up50
https://www.youtube.com/watch?v=CSxHbPc7TMY
https://www.youtube.com/watch?v=yURalgCDQW8
https://www.youtube.com/watch?v=ejI91h-kjJI
https://www.youtube.com/watch?v=xIplNs4754Q
https://www.youtube.com/watch?v=sKIyBsiI1Z4
https://www.youtube.com/watch?v=ugf58OIPhUY
https://www.youtube.com/watch?v=yWQkp9cT7Rs
For more information, visit my YouTube Channel:
https://www.youtube.com/user/nabilebraheim