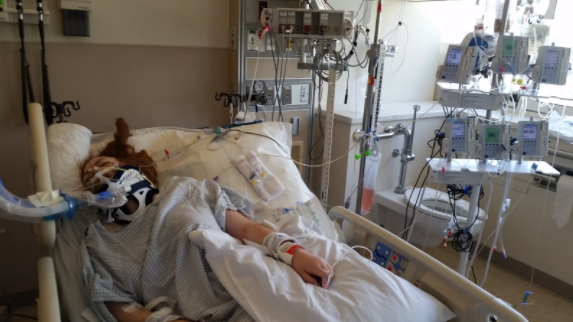
In 2015, I fell 20 to 25 feet out of a tree.
All of my medical records list different heights since no one knew the precise distance — that detail feels important to me. The person I had been climbing with said we were near the top of a redwood on the University of California, Santa Cruz’s campus when I turned to her and said, “I have to get down. Now.” Then, without waiting for a response, I scrambled downward until I was out of sight. A moment later, she heard two smacks followed by a thud.
Before I fell out of the redwood, I was drinking alcohol every day. In fact, I had been drinking pretty consistently since the age of 14. To say I simply had a “drinking problem” would be a gross understatement.
Often, I’d get C’s (or lower) in classes at UC Santa Cruz simply because I’d forget to turn in an assignment or get hammered and decide not to write an essay. One teacher’s assistant, after grading a paper I had managed to get in on time, handed it back to me, marked with an A, and gave me a line similar to the one Dr. Octavius gave Peter Parker in “Spider-Man 2”: “You’re brilliant when you turn things in. Imagine if you were more diligent.”
In my head, I translated this to: “Imagine if you weren’t depressed, ... if you weren’t a drunk, ... if you were just a better person.”
Instead of being a better person, I’d get drunk and climb trees. Usually, I avoided redwoods when I was three sheets to the wind, but I had a tolerance — a couple of beers wouldn’t stop me from climbing. The friend I was with on that fateful day said I had only had two beers. I can’t confirm or deny this because I have no memory of my fall or the entire day that preceded it.
“My family wasn’t given a specific prognosis because chances were that I wouldn’t wake up.”
For 10 days following my fall, I was in a coma, my vitals monitored at every moment at Santa Clara Valley Medical Center in San Jose, California. My family wasn’t given a specific prognosis because chances were that I wouldn’t wake up.
Comas aren’t what Hollywood would have you think they’re like. The media glosses over two main things when it comes to comas: the (un)consciousness of a coma — you’re dead to the world — and the immediacy of your uselessness upon waking. Every inactive day causes your muscles to atrophy. Your vocal cords may be paralyzed because of intubation (one of mine was), and you can’t swallow without aspirating (accidentally letting food or liquid enter your lungs, risking pneumonia).
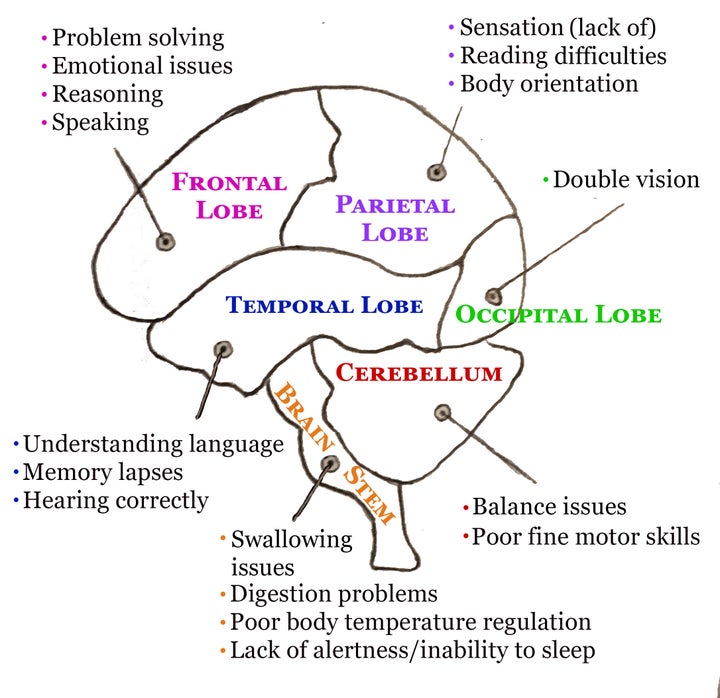
On top of these standard coma difficulties, I had a severe traumatic brain injury that affected nearly every aspect of my body. For example, I must’ve landed on my backside because the heft of the damage was located in the occipital lobe — that’s the lobe at the back of your head that controls vision. Because of this, I had diplopia (double vision), which required eye muscle surgery to be corrected (but that surgery wouldn’t happen for another nine months).
Because my injury was closed-head (my skull wasn’t penetrated), my brain bounced around inside of my skull, ricocheting against the hard surfaces and sending reverberations to many different regions. This is referred to as a diffuse axonal injury.
For me, my deficits revealed what other parts of my brain received damage. My balance problems (ataxia), lack of fine motor skills and poor grip strength indicated my cerebellum had been hurt. At first, my body also had issues regulating its temperature, signaling some damage to the brain stem. My fits of laughter and inability to remember anything longer than a few moments meant frontal lobe damage.
A medical social worker, at this point, staged an intervention about my drinking. She asked my mom to show me a picture of me in my coma, hooked up to machines. When I saw the photo and started laughing, the social worker told my mom, “This is just her injury.” She turned to me and said, “You almost died, and your drinking contributed to it — don’t you care?” When I didn’t stop laughing, my mom told the therapist, “She’s always been like this.”
It’s hard for professionals to determine which parts of you are pathological and which parts are damage sometimes. It’s also hard for family members not to be dismissive when they’re upset with you.
On top of that, I had to relearn everything. My speech therapist taught me how to swallow and gave me memory techniques to improve my recollection of details. My occupational therapist showed me how to navigate a kitchen, accompanied me into the shower to explain how to safely bathe myself in a precarious environment (aka the shower) and went over strategies to remember if I had completed a task or not. (“Have I shampooed? How many times? Did I put conditioner in my hair?” “How long have I been stirring these eggs?”) My physical therapist helped me work on my core strength for balance and worked with me on how to swing my arms correctly so I looked like a human being instead of a robot.
But relearning was difficult when my short-term memory was as impaired as it was. It didn’t end up coming back at all until a couple of weeks after I woke up from my coma. Apparently, I had already been doing speech, occupational and physical therapy for a while before I had any memories of doing any sort of therapy. It would take a few more days for me to remember the names of all of my therapists or to navigate the Brain and Spinal Cord Injury Unit (in my wheelchair).
“My occupational therapist showed me how to navigate a kitchen, accompanied me into the shower to explain how to safely bathe myself in a precarious environment (aka the shower) and went over strategies to remember if I had completed a task or not. (“Have I shampooed? How many times? Did I put conditioner in my hair?” “How long have I been stirring these eggs?”)”
I also contracted Clostridium difficile (commonly referred to as C. diff) toward the end of my stay. It’s very contagious and common in hospital settings, and patients often take a rigorous course of antibiotics to treat it. The antibiotics kill the good gut bacteria that fends off the bacterium that causes C. diff. Considering the number of antibiotics I was prescribed while I had a bolt inserted in my head to relieve pressure caused by fluids in my brain, it was only a matter of time before I contracted C. diff. Although I was treated, and the C. diff eradicated, my gut health plunged, and my digestion tanked. I lost more weight in addition to the weight I had lost during my coma.
During this entire time, I was benignly resigned and vaguely amused. My doctors recorded my blasé comments (“Oh, I get to cook eggs? I like eggs.”), but my nearly illegible handwriting from that time tells a slightly different story. On a piece of notebook paper dated Sept. 5, 2015, I wrote, “I don’t know how I feel about the future. What is life if you can’t remember it?”
After a month and a half, I was released from Santa Clara Valley Medical Center under orders to use an arm crutch for all ambulation (walking). But my rehabilitation was far from over. Once I returned to my parents’ home in San Diego, I would attend a brain injury day-treatment program five days a week from 8 a.m. until 3:30 p.m. This program took up where the other left off: I continued to practice writing by hand and doing eye exercises, build core muscles and correct my abnormal gait and complete logic puzzles and plan my life to improve the executive function, courtesy of the frontal lobe.
After two and a half months, I was only required to attend three days a week. I could walk without a crutch or a gait belt (which I wore so therapists could grab it if I started to fall). After four months, I was discharged and finished the last units for my bachelor’s degree at UC San Diego while I awaited my eye muscle surgery (this meant I had to close one eye to read anything, both in and out of class).

During the summer of 2016, a year out from my accident, I was told this was the most I would recover. The tacit addition was that it was all downhill from there. According to the Centers for Disease Control and Prevention, 52% of people who suffer a severe traumatic brain injury will further decline or die within five years of their injuries. Medical professionals were pleased I was doing well — I started working as a production assistant at an academic publisher, commuted independently on the train and was applying to grad school to get better health insurance — but everyone waited for a decline.
The real problem through all of this was that I looked fine. You can’t tell a person has a brain injury just by looking at them, and you certainly can’t discern the difficulty with which they’re holding themselves together in front of you. Even my own mother, who had been there throughout my coma, thought it was a good idea to take me out on a boat to go whale watching a few weeks after I was released from Santa Clara Valley Medical Center.
Nearly five years out from my fall, problems persist. Although I am lucky to function at such a high level considering the severity of my injury, I am permanently disabled but don’t look it. My body doesn’t listen to my brain very well, and my cognition falls short when it comes to mental math and my working memory (whiteboards line my room with scrawled reminders and notices held by magnets).
My long-term memory is intact: I remember my childhood and my family, but it’s the processing speed that causes issues. Sometimes it takes me a moment to recognize a place or a person or to place a person in their context. Sometimes I lose my words, can’t recover them (aphasia) and simply have to find a workaround or give up.
“People ask for my seat on the subway, and I feel too tired and embarrassed to say I need it — to explain my damage — so I cling to a pole and arrive at my destination shaking from the exertion.”
Some days are worse than others. Sometimes I have phantom pains in my extremities, and I still can’t write by hand for prolonged periods, i.e., more than a few sentences. Often, people are annoyed when I ask them to write something for me or if I can’t take the stairs. I’ve had baristas roll their eyes at me when I request a lid because I can’t carry a cup of liquid without sloshing it (“They’re on the condiment bar,” the baristas insist). People ask for my seat on the subway, and I feel too tired and embarrassed to say I need it ― to explain my damage ― so I cling to a pole and arrive at my destination shaking from the exertion.
I’m still an alcoholic. I’ll always be an alcoholic, but my coma served as a detox period. My disability prevented me from going to bars or obtaining alcohol in the beginning, enabling me to put the “white knuckle” approach to use. Of course, since then, I have relapsed, but I get cut off after a drink because my ataxia gives me a permanent wobble. Luckily, explaining I have brain damage just invites raised eyebrows and no beer. I know if I start drinking again, it’ll kill me. Instead of imbibing, I go to therapy and write stories — more productive pursuits.

And in the big scheme of things, my current deficits are just quibbles: My depression is medicated, and I’m sober. I teach at a college that respects my viewpoint and limitations — my students understand and are patient, as is the majority of my colleagues. I’m happier now than I ever was before falling out of the tree.
I’m not sentimental — I don’t think everything happens for a “higher reason.” But I do believe in physics — in gravity — and I do understand the weight of my actions. I’m sorry for the grief my accident caused, but I’m not sorry it happened.
Brooke Knisley is an instructor in Emerson College’s Writing Studies Program. Her work has appeared in The Independent, Playboy, Entropy magazine, McSweeney’s, DAME Magazine, VICE Health, The Boston Globe Magazine and others. She is working on a memoir about trauma and its damage.
Do you have a compelling personal story you’d like to see published on HuffPost? Find out what we’re looking for here and send us a pitch!
Need help with substance use disorder or mental health issues? In the U.S., call 800-662-HELP (4357) for the SAMHSA National Helpline.
