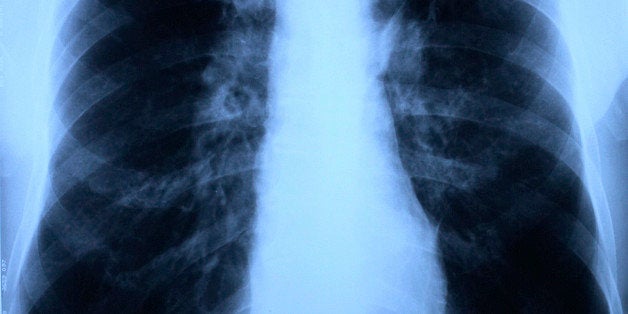
"Fight Tuberculosis with Modern Weapons," proclaimed a 1935 public health awareness campaign against what was one of the leading causes of death in the U.S. Those weapons: chest X-rays and lung surgery.
Fast forward to the 1960s. Effective treatment with antibiotics had transformed TB, a scourge as old as humanity, into the historical curiosity it is today for most Americans. Yet TB hasn't gone away.
Every year, thousands of Americans undergo months-long, costly, and often toxic TB treatment. Those treatments -- powerful antibiotics -- are still our primary weapons against the disease. It's a line of defense that may not hold, as the emergence of increasingly drug-resistant TB strains threaten to turn difficult treatments into obsolete ones.
Until we have better ways of detecting and treating TB, thousands of Americans and millions of people worldwide will continue to suffer from an illness that should have been consigned to history long ago.
To be clear, our nation's TB control efforts have achieved remarkable success. The most recent data from the Centers for Disease Control and Prevention reveal the lowest number of TB cases since reporting began in the 1950s -- about 9,600 in 2013.
Drug-Resistant TB
The ultimate goal of U.S. TB programs is to eliminate the disease in this country, just as we once did with malaria, polio, and smallpox. That will require bold efforts to address drug resistance, both here and abroad. Globally, of the nearly nine million TB cases that occur every year, one in 25 is multidrug-resistant (MDR). This means people with MDR TB cannot be treated with the two best TB drugs, and potentially others as well. While only about 1 percent of U.S. cases are MDR, keeping it that way is a constant challenge.
Because TB treatment is long and difficult, it can be hard for patients to complete -- which can result in drug resistance. A typical case takes six to nine months to treat. That's up to 270 days of antibiotics, blood tests, X-rays, and doctor's appointments to make sure people take every one of their pills.
In the U.S., treatment is usually successful despite these challenges. But in many countries where TB is far more prevalent, many people receive incomplete or substandard treatment, leading to resistance. Resistant strains of the disease can then be transmitted directly to others, putting everyone at risk.
Having MDR TB makes the experience dramatically worse. People with drug-resistant disease must endure two years or more of grueling treatment, often with drugs that must be injected and have substantial toxic effects. Major side effects include hearing or vision loss, liver or kidney damage, depression or psychosis. Patients often are forced to place their lives on hold. In a recent CDC study, nearly three-quarters of U.S. patients treated for drug-resistant TB were hospitalized, more than one-third faced home isolation (most for months), and more than one in four stopped working. Nearly one in ten died.
Treating drug-resistant TB is also very expensive. The same CDC study found that MDR TB treatment cost $134,000 per case on average, rising to $430,000 for the most extensively resistant cases. That's compared to $17,000 for drug-susceptible TB. If productivity losses experienced by patients are included, treatment costs can rise as high as $554,000.
How To Beat TB
These human and financial costs are unacceptable. To get serious about ending the threat of TB in the U.S. and reducing its human cost worldwide, we need action on three main fronts:
First, U.S. health care providers and local health departments need to work together to make sure that every single case of TB is diagnosed and effectively treated. Testing for drug resistance should happen right after a case is diagnosed, and providers should consult with a TB expert as needed - especially in the case of drug resistance -- to ensure an effective treatment regimen is prescribed. In addition, patients should receive "directly observed therapy," in which a health care worker is present every time they take their medicine.
Second, global TB control efforts need to be strengthened so that more people receive effective, timely treatment and avoid developing drug resistance. We at CDC are lending our support to these efforts. As just one example, we're working with the U.S. Agency for International Development in several countries to improve MDR TB diagnosis and management.
Finally, we need 21st-century TB tools to fight TB. After decades of neglect, we're finally seeing progress on this front. The first in a new class of drugs to treat MDR TB was approved by the Food and Drug Administration in 2012 (representing the first new class of TB drugs in over 40 years), and additional research on faster TB tests, more effective drug regimens, and potential vaccines is under way. But given the scale of the problem, more attention, more creative ideas, and more resources are needed.
Humanity has lived with, and died from, tuberculosis since recorded history began. The last century brought the hope of ending that tragedy, but success has remained elusive. It's time to make it a reality.