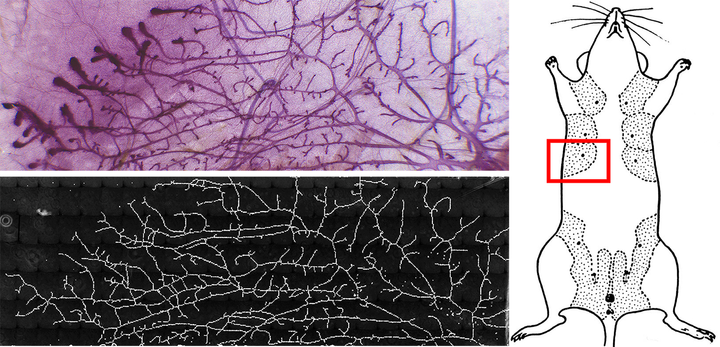
An illustration of one of the two types of biological structures -- a vascular network -- created using a new technique developed by a team at UCSF.
We need more organs. At any given moment, more than 123,000 Americans are waiting for an organ transplant. Each year, 6,500 of them die for want of a donor. Moreover, between 15 and 50 percent of patients lucky enough to receive a transplant from a donor -- depending on the organ -- suffer from acute organ rejection within five years.
For that reason, scientists across the country are racing to develop a way to grow organs in the lab. The dream is to eventually use a patient's own cells to construct new kidneys, livers, hearts and lungs that would be impervious to rejection by their immune systems -- in other words, a way to let patients be their own organ donors.
What makes this hard is that the techniques humans use for manufacturing most things don't work for organs. A car "has lots of pieces, and they fit together very nicely, and they're guided to the correct position by a human hand or a robot, and then welded together into this complex machine," said Dr. Zev Gartner, an associate professor of pharmaceutical chemistry at the University of California, San Francisco. "Tissues and organs, on the other hand, self-assemble in a process that's guided by rules that are quite distinct from the way that we as humans think about building stuff."
One key challenge is getting blood vessels to the right place. It's essential, because blood vessels deliver life-sustaining oxygen and nutrients to the cells, but the tiny vessels travel circuitous paths through organs -- surrounded at all times by other types of cells.
This week, researchers from Gartner's lab unveiled a technique that could help overcome this obstacle. The team developed a method for assembling living cells (from both mice and humans) into tiny "organoids" with a simplified version of the deeply complex structures of actual organs.
The technique, written up in Nature Methods, is essentially a form of 3D printing -- but it doesn't involve a 3D printer. Instead, it's not totally unlike glitter painting, where little kids draw a pattern in glue, pour a bunch of glitter over it, then shake away the excess to reveal a glittery shape. Except instead of glitter, the scientists used cells -- and instead of glue, they used DNA to make a kind of biological Velcro that affixed the cells in the right place.
This video, courtesy of The Gartner Lab and Nature Methods, demonstrates the principles of the technique. All those little circles are cells:
What makes this technique unusual, though, is that the scientists assigned differently coded strands of DNA to different types of cells. So they were able to specify the location of different types of cells precisely, much as the human body does naturally.
"The DNA has this remarkably ability to only stick to the complementary sequence, and when it finds that complementary sequence, it sticks very, very quickly and specifically," Gartner said. "So what we've done is turn this molecule, which is normally a genetic information carrier, into [...] a multi-flavor Velcro."
To return to the glitter painting analogy, it's as if you could assign different types of glue to different colors of glitter -- so that if you drew concentric arcs using glues for the seven major colors, poured multicolored glitter over it and shook off the extra, you would be left with a rainbow.
But the group was working in three dimensions, not two. They built up the organoids atop a piece of glass, layer by layer. Depending on the pattern they started with, that left them with either a cluster of several different types of cells around half the size of a human thumb or a complex branching structure of cells that resembled a vascular system.
Gartner's team built these structures using just three or four types of cells, but the technique could, in principle, accommodate any number of cell types.
In the short term, Gartner said, their goal is to use this method to study the development of tissues and the interactions between the cells that make up those tissues. But Gartner hopes to eventually refine the technique enough to use it to build working human organs. Such organs could be used first to test new experimental drugs; they would give researchers a better idea of some drugs' effects on our bodies than today's lab mice do. The hope is that eventually they can act as personalized transplant organs for people whose own organs are failing.
"That's a very long-term goal," Gartner said. "Being able to build an organ is the dream, but it's at least a decade away, if not multiple decades away."
