Since January 2015, my tiny private allergy practice in Manhattan has prescribed over 2,200 Epinephrine auto-injectors or refills, many yielding sales for the EpiPen brand. While politicians, the FDA, drug reps, the media, and other talking heads deliberate Mylan's monopoly and ability to price gouge, allergists are having hard conversations with those who rely on the drug to save them from a potentially inescapable life-threatening scenario.
Epinephrine injections are used to treat anaphylaxis, which occurs when your immune system overreacts to an allergen. Anaphylaxis can occur with small and even trace exposure to common triggers such as foods, insect stings, medications, latex, or even exercise. Anaphylactic reactions are a medical emergency. They can occur quickly and can be fatal. Anaphylactic reactions merit immediate treatment.
The threat of anaphylaxis is a particularly scary reality for the 15 million Americans who suffer from food allergies or 24 million Americans with asthma. When considering anaphylaxis, this is a better safe than sorry predicament.
Any person with a history of an anaphylactic reaction, or any person who has learned from a doctor that they are at an increased risk of an anaphylactic reaction, should carry an epinephrine auto-injector device. Epinephrine injections are the first line treatment for an anaphylactic reaction. It is possible that a single epinephrine injection can reverse an anaphylactic reaction entirely. However, in some anaphylactic reactions, patients will need a second dose of epinephrine. This is one reason epinephrine auto-injectors are sold in packs of two.
Regardless, any patient experiencing anaphylaxis or having administered an epinephrine injection should call 911 and seek immediate medical treatment in an emergency medical facility.
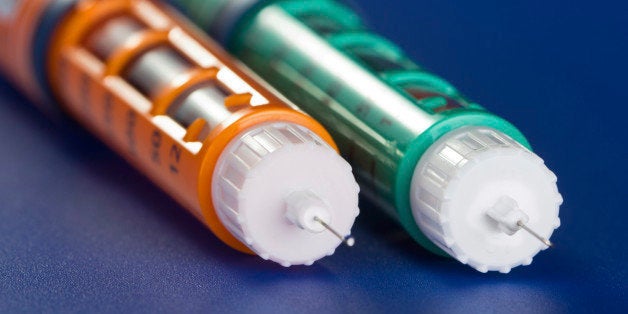
Epinephrine auto-injectors like the EpiPen, Adrenaclick, the recently discontinued Auvi Q, or any generic spin off make the administration of epinephrine much more practical. An alternative would be using a syringe and serum, which is what some EMTs have fallen back on. However, this is certainly more difficult and may not be feasible, especially since an injection is needed at a moment's notice and it is often a bystander who administers the injection to an anaphylaxis victim.
EpiPen has become the industry standard and in most cases the only option, and a price surge for this product certainly warrants this current uproar. It is particularly concerning because these devices are going to become cost prohibitive for many, and those who could potentially need them will opt to or be forced to go without, and thus be risking their lives. Like insurance, it is something you need to carry but hope you never use.
Epinephrine auto-injectors generally have about a one-year shelf life, at which point the epinephrine may become too weak to be effective. Its potency literally diminishes by the day, and thus individuals should check the expiration date and re-up as needed.
Additionally, it is advisable to have multiple epinephrine auto-injectors at your disposal, especially for children. They should carry one in their backpack (once mature enough to understand their health situation), their school nurse should have one and be aware of their condition (some schools have one anyway, after passage of the School Access to Emergency Epinephrine Act in 2013), divorced parents need one at each house, or at Nana's, etc.
Point is, by inflating the cost, there are going to be situations where an epinephrine auto-injector will not be available when someone really needs it, and someone could die from a preventable death. As an allergist, this is a conversation I must have with patients on a daily basis: "I'm sorry, I know it costs a lot, and I hope you never use it, but you need to buy one -- actually more than one -- and you need to spend this money every year." And while normally I am the one giving the shots, in recent times I am the one who ends up getting shot, as the messenger.