
This story was originally published by The UAB Mix.
Breakthrough research suggests a female sex hormone may be the key to saving lives on the battlefield, where between 2001 and 2011 more than 80 percent of potentially preventable U.S. war injury deaths resulted from blood loss.
The hormone shows the promise of prolonged survival despite massive loss of blood and could be carried in a small autoinjector for use.
In a landmark step – after 19 years of research by Irshad Chaudry, Ph.D. – UAB has received a $10 million U.S. Department of Defense contract funded by the Combat Casualty Care Research Program, U.S. Army Medical Research and Materiel Command, Fort Detrick, MD, to begin testing its potentially life-saving synthetic estrogen for safety in humans. The long path to this breakthrough for Chaudry, who is director of the Center for Surgical Research in the UAB School of Medicine, was prompted by a mistake; in 1997 he and postdoctoral fellow Rene Zellweger, M.D., received the wrong shipment of mice.
Chances like that are a beguiling part of science. Alexander Fleming discovered the penicillin mold through fluke contamination in a Petri dish. Charles Goodyear created vulcanized rubber after accidental stove contact. The hint leading to the first microwave oven began when radar researcher Percy Spencer reached in his pocket and found his chocolate bar had melted.
Chaudry and Zellweger’s spark of serendipity came during study of a serious complication seen in trauma-hemorrhaged patients – the bacterial blood infections that are called sepsis. These infections can strike days, weeks or months after severe trauma and blood loss, causing single or multiple organ failure, long hospital stays and death of patients. “The cost to society is substantial, and the onset of sepsis after trauma is a major, worldwide problem,” Chaudry said.
Chaudry and Zellweger were examining the mechanism by which sepsis produces multiple organ failure and death in a murine model. But when Zellweger received a group of female, not male, mice, he told Chaudry they were unsuitable because female hormone levels vary too much.
Chaudry told Zellweger to use the female mice, and the result was astonishing. All of the female mice resisted sepsis without any treatment.
“I was excited,” Chaudry said, “and he was puzzled.” So they repeated the work with another group of female mice, but this time the untreated septic mice all succumbed to the infection — a seeming paradox.

‘Wasting our time’
“See, we’re wasting our time,” said Zellweger. But the researchers solved the puzzle when they realized that the two groups may have been at different stages of their estrous cycles. By pure chance, the females of the first group had been at the proestrous phase, that moment when estrogen hormones levels are at their peak. In animal models, Chaudry and colleagues soon learned that a dose of the estrogen 17β-estradiol (E2) could protect males and females against septicemia, regardless of the female estrous phase. The estrogen affects the immune system and cardiovascular responses, which typically are profoundly depressed after trauma.
Chaudry and his colleagues next tested E2 for another trauma problem — blood loss. They found that after massive blood loss, and an additional prolonged hypotensive period, followed by intravenous fluid resuscitation, E2 significantly improved heart performance, heart output and liver function. E2 also attenuated an increase in interleukin-6, a pro-inflammatory cytokine.
About this time, in 2005, the U.S. Defense Advanced Research Projects Agency, DARPA, announced a vital goal: finding a way to stretch the time that a severely wounded soldier with blood loss could stay alive. This would give the warfighter a better chance of reaching a field hospital for definitive surgical and medical care.
The agency held a competition with a simple and unequivocal criterion – produce a treatment that enables survival at least three hours after significant, almost universally fatal blood loss. Any research programs that passed this first trial then would face a Phase II challenge of six-hour survival. Furthermore, the therapeutic material had to be deliverable in a small volume, for easy future inclusion in a battlefield pack.
Chaudry and his colleagues discovered that E2 could allow survival for three hours without any fluid resuscitation, and long-term survival if fluid resuscitation was provided after 3 hours. The prolonged period of low blood pressure after blood loss significantly affects mitochondrial function, endoplasmic reticulum stress markers and inflammatory cytokine production, but E2 was able to diminish those changes. Low blood pressure reduces the delivery of oxygen to tissues and to the mitochondria, which voraciously consume oxygen to produce energy in the form of ATP. Thus, oxygen deprivation is a burden for tissues and mitochondria under low blood flow conditions.
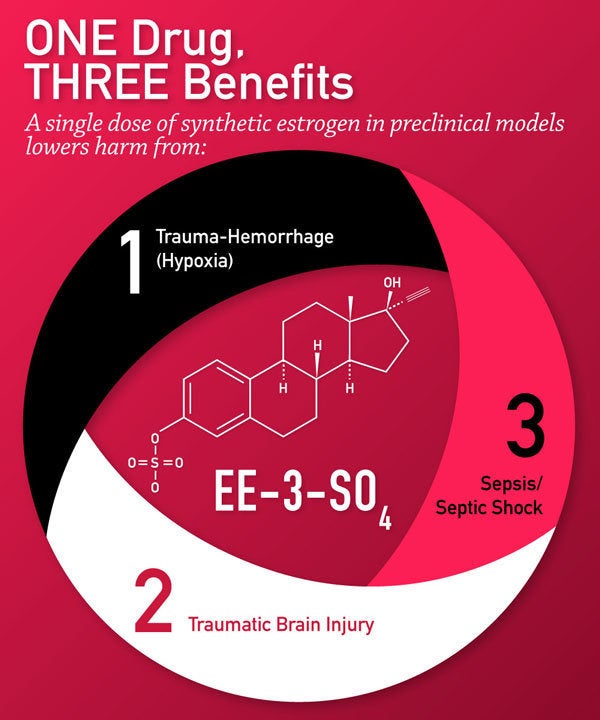
In the three-hour challenge, Chaudry and his colleagues used E2 that was microencapsulated within cyclodextrin to make it water soluble. For the six-hour challenge, with the help of DARPA, UAB had a synthetic estrogen variant called ethinyl estradiol-3-sulfate, or EE-3-SO synthetized by a pharmaceutical company. Six-hour survival rates of 50 and 80 percent were seen with EE-3-SO in porcine and murine models respectively, even in the absence of fluid resuscitation. These results from a multi-site study led by Chaudry, which were reported in 2014 and 2015, provided the needed proof of principle for initial clinical studies.
Out of 10 initial Surviving Blood Loss programs funded by DARPA, UAB was the only one that met the challenge of six-hour survival after 60 percent blood loss in the absence of fluid resuscitation.
Mechanistic studies
DARPA’s six-hour aim was solely survival, but Chaudry has continued mechanistic studies of how EE-3-SO produces beneficial effects. The estrogen appears to interact with the different types of estrogen receptors in all types of tissues in both men and women. Using selective estrogen-receptor antagonists or agonists for the different types of estrogen receptors, Chaudry’s research team continues to look at which type of receptor is important for EE-3-SOaction in different tissues.
Besides improved heart function, EE-3-SO appears to dilate blood vessels and speed the movement of fluid from the tissue compartment into the blood compartment (the interstitial fluid of the tissue compartment has about twice the volume compared to the average volume of blood in adult humans). Lowering this resistance to improve blood flow to vital organs hails back to the great challenge to trauma recovery seen by the noted English trauma researcher Harry Berrington “Berry” Stoner, M.D. He wrote that the body’s blood system is like a swamp after trauma, and anything that turns the swamp into a running brook is the answer for treating shock.
Human trials
DARPA was key to finding a company to manufacture pharmaceutical grade EE-3-SO under U.S. Food and Drug Administration Good Manufacturing Practice. Also, in preparation for an investigational new drug application to the FDA, some of the pre-clinical animal experiments have had to be done in institutions under FDA Good Laboratory Practice.
UAB has applied for patent protection for EE-3-SO. Beyond its battlefield potential, one important application could be domestic trauma patients, given that earlier E2 results that have shown reduced mortality and septicemia. Also, EE-3- SO may have a third beneficial effect – treatment after traumatic brain injury. In experiments, the estrogen is able to reduce cerebral edema, increase brain blood flow, increase cognitive function and memory, and lessen brain cell death. Thus, EE-3-SO may prove to be a triple boon for trauma victims.
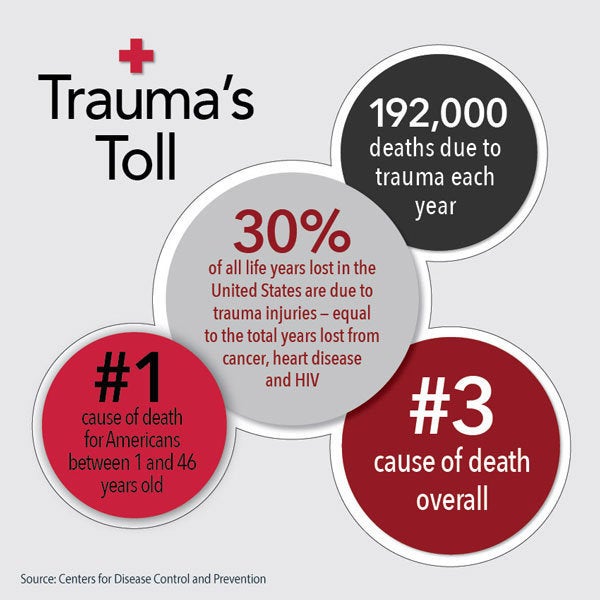
Trauma is the leading cause of U.S. deaths for people under 47 years of age, according to the federal Centers for Disease Control and Prevention. Because trauma hits all ages of people, it represents 30 percent of all U.S. life-years-lost each year, a far larger loss than cancer, 16 percent of all lost life-years, or heart disease, 12 percent.
“If we can prevent sepsis and multiple organ failure after trauma,” Chaudry said, “insurance companies will gladly reimburse drug costs because there will be great cost benefits and the quality of life will be better.”
"If these study findings translate to the battlefield,” Chaudry wrote in his recent paper last June, “additional time will be available for transport of the wounded to safer locations where standard resuscitation measures can be accomplished."
Likewise, the so-called “golden-hour” after injury for needed fluid resuscitation may be prolonged to six hours if a small volume of E2 is administered shortly after injury in patients at the scene of an accident in rural areas where transportation to a Level 1 trauma center takes more than an hour.
Chaudry’s 19-year study of the effect of estrogen began at the Shock and Trauma laboratories, Michigan State University, and at the Center for Surgical Research at Brown University School of Medicine. Chaudry moved to UAB in 2000. He has had many collaborators since his initial 1997 paper with Zellweger and other colleagues in the journal Critical Care Medicine.
UAB’s B.L. Harbert Institute of Innovation and Entrepreneurship is managing two pending U.S. patent applications of EE-3-SO4, with Irshad H. Chaudry, William J. Hubbard and Zheng F. Ba listed as the inventors.
The recent Chaudry papers on six-hour survival, published in the Journal of Trauma and Acute Care Surgery and Journal of Surgical Research, include co-authors from UAB, the Keith Pharmacology Research Group, Andover, Massachusetts; Fast-Track Drugs and Biologics, North Potomac, Maryland; Texas A&M Institute for Preclinical Studies, Texas A&M University; and NDA Partners, Falls Church, Virginia.