As a teenager, I hated my skin. While I know now that my acne wasn’t actually that bad, I was convinced it was blotchy, red and terrible. In my early 20s, my skin was fine ― not glowy or perfectly smooth, but fine. Whenever that time of the month came around, I’d wake up to a few pimples here and there, particularly along my jawline and neck, but they usually went away within a week (if I could refrain from attempting to pop them).
Last year, when I turned 26, everything changed.
I decided to get an intrauterine device, aka an IUD (which, for the record, I really like now). Little did I know that while the small T-shaped device prevented me from getting pregnant, it would also wreak havoc on my skin.
It was January 2017. After not being on any sort of birth control for a few years, I got the hormone-based Mirena IUD. Aside from the extremely painful insertion process ― yes, it hurts A LOT ― I was happy with my decision.
A month later the breakouts started.
I began developing red, painful and downright angry cystic breakouts along my jawline and neck. After doing some research, I realized my experience wasn’t unique. I just wish I’d had some sort of warning of how bad it could get before I had a foreign object placed inside my uterus.
Although I’d experienced this type of acne in the past, especially around my period, there was something different this time. Before, I would get one, maybe two decent-sized pimples, but they’d typically disappear within a week or so. After the IUD, the breakouts just wouldn’t go away.
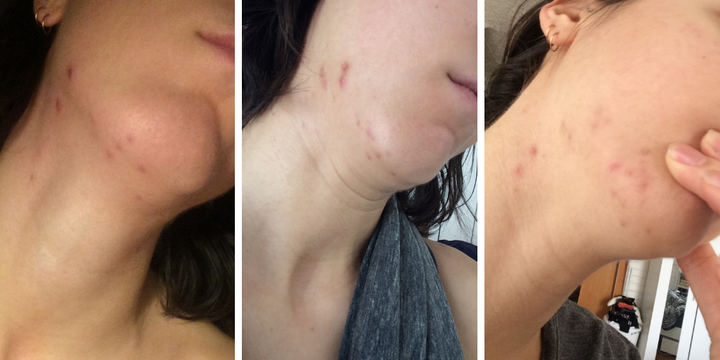
Around the same time as the acne appeared, I went in for a follow-up IUD appointment with my gynecologist. I noted that I seemed to be breaking out a little more, but admittedly downplayed my concern. Instead, I chalked it all up to the fact that my body was still getting used to the foreign object (and hormones) placed inside it and figured the breakouts would eventually clear up on their own. And it seemed like they were starting to ...
But in January 2018 ― almost exactly a year after I got my IUD ― I was greeted with another round of angry cystic pimples that just wouldn’t quit. It was basically the worst anniversary gift I could’ve received. (Thanks, IUD!) Initially, I thought my skin was just irritated because I was using a new detergent. I’d also gifted myself with a birthday facial and thought that might have played a role. It got so bad that my mom even asked me if I had chicken pox (despite the fact that I had chicken pox as a child).
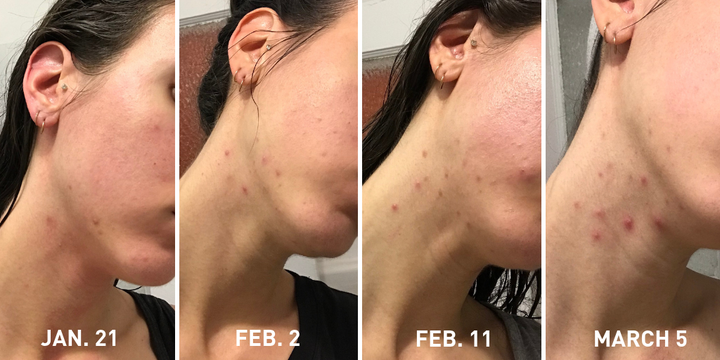
I tried everything to treat the breakouts on my own. First, I stopped using the fancy serums and oils I was testing for work ― as a beauty editor, I’m constantly trying new products without giving my skin much time to breathe ― and went back to basics. I attempted to spot treat with salicylic acid products, sulfur-based products or 100 percent tea tree oil, with no success. I tried cutting down on my sugar and dairy intake, but didn’t really notice any changes. When one pimple would get smaller, another one would pop up beside it, and then another one beside that one, and so on and so on.
March rolled around and the breakouts didn’t calm down. So, for mostly personal reasons, I pitched a story to HuffPost about how to treat hormonal acne. I did plenty of research, read about various treatments and spoke to dermatologists in hopes of clearing my skin again.
And what I found was spironolactone, a prescription medication typically used to treat high blood pressure and heart failure. In low dosages, “it can work like a charm for hormonal acne,” said Dr. Jennifer MacGregor of Union Square Laser Dermatology in New York, because of its anti-androgen properties.
Hormonal IUDs release hormones ― typically just progestin ― which can throw your body’s chemistry a little off balance, as noted by Bustle. If your levels of androgen hormones (the male sex hormones, like testosterone) increase, that can overstimulate your oil glands and lead to increased oil production, which can then lead to breakouts. Spironolactone blocks androgen hormone receptors so, according to HealthLine, it can help stabilize hormone levels.
After learning about spironolactone and reading other people’s positive experiences with it, I went to see Dr. Samer Jaber at Washington Square Dermatology in New York. Over the phone, he told me that he often sees patients dealing with cystic breakouts after an IUD insertion and that many of them aren’t actually aware of the acne-related side effects that may come with the device. (Interestingly, he noted, combined hormone birth control pills ― that is pills with both estrogen and progestin ― are a common treatment option for acne.)
After he examined my skin, Jaber presented me with a few options, including having the IUD removed (which I wasn’t quite ready to do) and trying spironolactone in conjunction with topical acne treatments. I opted for the latter and left his office with a prescription ― for both spironolactone and Aczone, a topical acne gel ― and a glimmer of hope.
Much to my delight, I started noticing a difference in my skin after a couple of months. The breakouts didn’t magically disappear, but they were getting smaller and weren’t as painful. As for side effects from the medication, mine were (thankfully) minor: I experienced some irregular spotting and found myself having to pee more frequently, but both effects went away after a few months.
Fast forward to now ― about seven months later ― and my breakouts are basically gone. I get some tiny pimples here and there, but nothing compared to the cystic acne at the start of this year. If I’m being totally honest, my skin has never looked better. I barely even wear any makeup anymore (save for some mascara and a hint of blush).
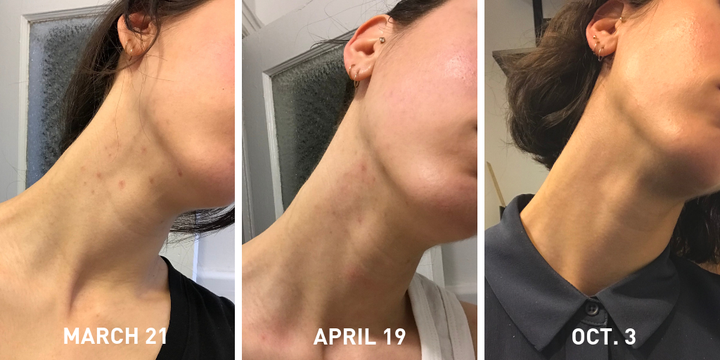
Jaber said that spironolactone is a good option not only for people like me ― someone who got acne after an IUD insertion ― but for women experiencing hormonal acne sans IUD. Even if someone’s testosterone levels are normal, their body can overreact to the hormone. “Spironolactone, by blocking testosterone receptors, can improve acne,” he said.
Most women with hormonal acne can get relief with spironolactone, Jaber said, especially when used in combination with topical treatments like retinoid cream or topical antibiotics. But he added that every patient is different.
MacGregor noted in an email that spironolactone “would not be a good choice for those with blocked pores (blackheads and whiteheads), T-zone acne, acne rosacea and other non-hormonal forms of acne.”
For those individuals, Jaber said, topical treatments ― whether it’s a retinoid cream or a combination of retinoid and anti-inflammatory ― might be sufficient.
Going on spironolactone has (so far) worked for me, and while I don’t necessarily want to take it for the rest of my life, I plan on sticking with it for a while.
But that’s me. And what worked for me and my skin won’t necessarily work for everyone. Plus, not everyone who gets a hormonal IUD will experience acne like I did. Some may see no changes in their skin at all. The best thing you can do before starting any new medication or treatment is talk to a doctor about your options.