
If a person cannot do the OK sign, this person may have a nerve injury (anterior interosseous nerve injury) or a rupture of the flexor pollicis longus tendon (the tendon that bends the thumb). Also, paralytic brachial neuritis may present with flexor pollicis longus and flexor digitorum profundus weakness and an EMG of the shoulder girdle may help distinguish this condition from anterior interosseous nerve syndrome. An inability to do the OK sign is known to result from a supracondylar humerus fracture in children.
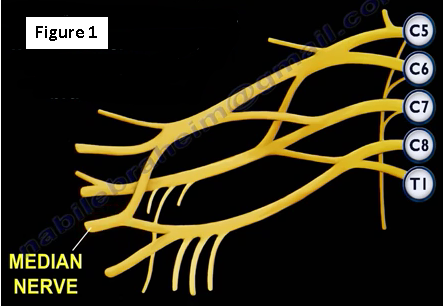
The anterior interosseous nerve arises from the median nerve about 4-6 cm distal to the elbow, which is about 1/3 of the way down the forearm (Figure 1). The anterior interosseous nerve exits from the anterolateral aspect of the median nerve and it runs between the radius and the ulna on the interosseous membrane between and below the muscles of the flexor digitorum profundus and the flexor pollicis longus.
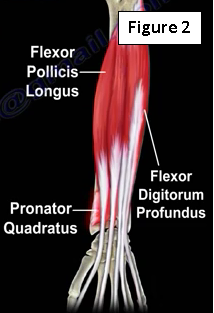
This anterior interosseous nerve innervates three muscles of the forearm; the flexor pollicis longus, flexor digitorum profundus (lateral half), and the pronator quadratus (Figure 2). The medial part of the FDP is supplies by the ulnar nerve (FDP has dual innervation) (Figure 3).
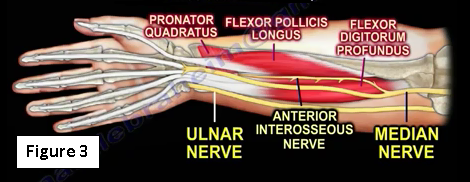
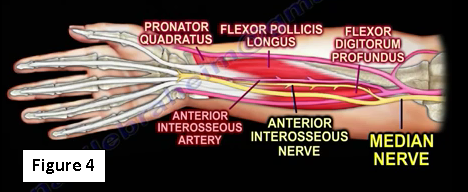
The anterior interosseous nerve passes dorsal to the pronator quadratus with the anterior interosseous artery and provides innervation to the volar wrist capsule. The terminal branch of the anterior interosseous nerve innervates the carpal joint capsule (Figure 4).
The integrity of the anterior interosseous nerve is tested by performing the O.K. or circle sign. The patient will be asked to make the O.K. sign by touching the tips of the index finger and thumb together. Integrity of the anterior interosseous nerve allows for flexion of the distal phalanx of the thumb and the index finger. When an anterior interosseous nerve injury is present, the patient will be unable to bring together the distal phalanx of the thumb and the index finger. The patient is unable to make the O.K. sign (Figure 5). Testing the integrity of the anterior interosseous nerve by touching together the middle finger and the distal phalanx of the thumb is not reliable.
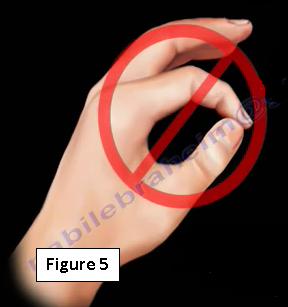
With injury to the nerve there will be a loss of motor function, however there will be no loss of sensory function. Unable to do the O.K. sign means that there is a loss of motor function. There will be aching in the anterior forearm (Figure 6).
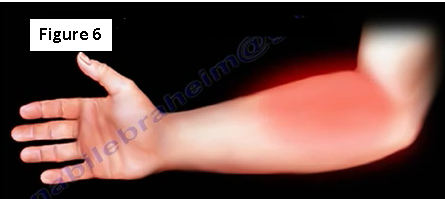
A patient with a complete anterior interosseous nerve injury or a high medial nerve injury is asked to make a fist. The first and second digits will have difficulty in flexing, while the other digits will flex. The third digit will be weak, while the fourth and fifth digits are normal (Figure 7). This position of the hand is similar to the position taken during a hand blessing.
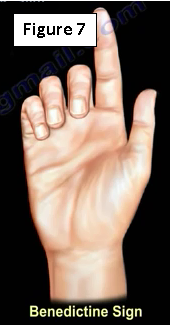
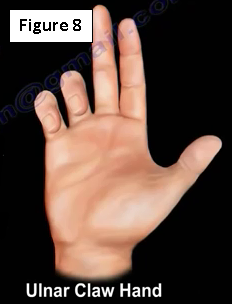
The Benedictine sign is different from an “ulnar claw hand.” (Figure 8) Ulnar claw hand refers to damage to the ulnar nerve and is seen when attempting to extend all the digits (leaving the 4th and 5th digits flexed).
Treatment
Treatment is initially conservative involving observation with EMG testing. If no improvement occurs in 4-6 months, an exploration and release may be needed.
Differential Diagnosis
The inability to do the O.K. sign may also result from a high median nerve injury. The presence of sensory symptoms will indicate a median nerve injury.
Froment’s Sign
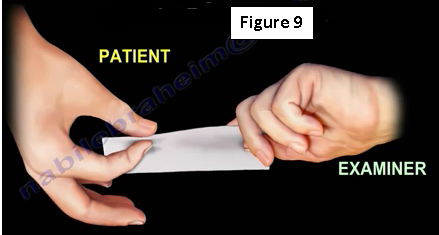
Froment’s test is performed to determine the presence of an ulnar nerve injury (Figure 9). When pinching a piece of paper between the thumb and the index finger, the thumb IP joint will flex if the adductor pollicis muscle is weak. With an ulnar nerve injury, the adductor pollicis muscle is weak and the patient cannot adduct the thumb. The flexor pollicis longus muscle substitutes for this movement by flexing the thumb. Bending of the thumb when pinching the piece of paper is a sign of an ulnar nerve injury.
Important Points
In patients with Martin-Gruber Connection, the median nerve, or anterior interosseous nerve to the ulnar nerve in the forearm may present with intrinsic muscle weakness. It may be differentiated also from Parsonage-Turner Syndrome (acute brachial plexus neuritis) and patient may have pain in the affected extremity. In anterior interosseous nerve entrapment, the median nerve conduction study result will be normal, however the needle EMG of the anterior interosseous innervated muscles will be abnormal.
For more information, follow the links below
For more information, visit my YouTube Channel:
