In their famous August 2016 article in JAMA Pediatrics, “Unintended Consequences of Current Breastfeeding Initiatives,” Dr. Joel Bass and colleagues cite data from the Massachusetts Department of Public Health showing a disturbing proportion of Sudden Unexplained Infant Deaths (SUID) in the first 5 days of life among newborns, which they link to hospital-based breastfeeding initiatives in that state. This forms the primary justification for their argument that the government agencies should withdraw support for breastfeeding interventions comprising the Baby-Friendly Hospital Initiative (BFHI). Their paper has been cited 10 times and viewed 4,825 times as of November 23, 2017, and has been remarkably influential. The authors are particularly concerned about the possibility of death during skin-to-skin contact with a mother, a rare phenomenon known as Sudden Unexpected Perinatal Collapse (SUPC).
However, upon obtaining the actual Massachusetts infant mortality dataset from 2004-2013 used by Bass and colleagues, I found that the authors knowingly drew a false conclusion from the data, and that furthermore, a close examination of the data does not fit the timeline of implementation of breastfeeding interventions in the state of Massachusetts.
In their paper, authors pulled Massachusetts’s diagnostic codes for SUID among newborns. They concluded, “While SIDS in the first month of life is generally considered an uncommon event, in Massachusetts (2004-2013), 14% of the cases of SIDS occurred in the first 28 days of life. Of note, 8 (22.2%) of the cases of SIDS among newborns and 20 (35.1%) of the newborn sudden unexplained infant deaths occurred in the first 5 days of life . . .”
An official from the state Vital Records Department was able to send me the same dataset that was sent to Dr. Bass, which is unpublished but available to the public upon request. It is reproduced here in its original form, with the addition of totals.
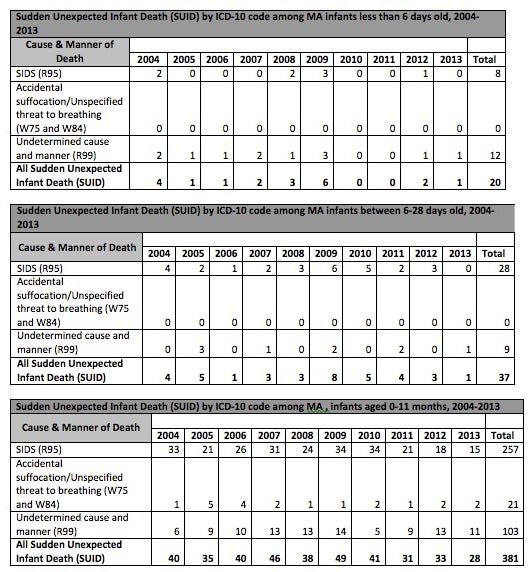
Dataset from Massachusetts Department of Public Health sent to Dr. Bartick 11/22/17
A couple of things stand out.
First, this data does not indicate whether these deaths occurred in the hospital. The state official indicated that this information is confidential and is therefore not available to Dr. Bass or to me. The authors are assuming that these deaths are related to hospital-based breastfeeding interventions, when we have no evidence from this data set whether these deaths even occurred in the hospital or not, whether they occurred while an infant was skin-to-skin, or bed sharing with a breastfeeding mother, and if so, what other risk factors were present, such as smoking, or impairment of the parent by alcohol or drugs.
Second, the largest numbers of deaths occurred were 2004 and 2009. In 2004, there was only 1 Baby-Friendly Hospital in Massachusetts, comprising 3.5% of all births and 4 or fewer facilities out of 49 on the BFHI pathway, according to data compiled by the Massachusetts Breastfeeding Coalition.
In November of 2008, I founded the Massachusetts Baby-Friendly Collaborative starting with the 4 facilities that were on the Baby-Friendly pathway at that time. I am thus intimately familiar with the progress of hospitals’ implementation of breastfeeding interventions across the state. In the spring of 2009, the first Massachusetts Mother-Baby Summit was held, the first statewide initiative to promote the BFHI. Massachusetts did not get its second Baby-Friendly facility until 2009, raising the percentage of births in Baby-Friendly facilities to 3.7%. Following 2009, there were only 3 deaths total, in 2012 and 2013. In January 2013, the Baby-Friendly Collaborative launched a new phase reaching out to all hospitals in the state and most joined. In 2012, Massachusetts had 4 Baby-Friendly facilities (5.7% of all births) and in 2013, it had 6 Baby-Friendly facilities (7.3% of all births).
All of these deaths pre-dated 2016 guidelines released by the American Academy of Pediatrics on establishing safe skin-to-skin contact in the hospital in order to prevent SUPC, which, though rare, has been associated with some practices of holding infants skin-to-skin that have since been found to be unsafe but can be prevented with certain positioning and monitoring practices. These guidelines acknowledge the importance of skin-to-skin contact for the health of the mother and the infant as well as for the establishment of breastfeeding. Ironically, these guidelines were published the day after the JAMA Pediatrics article.
While it is conceivable that some individual deaths in Massachusetts could have been from SUPC, the state data certainly do not demonstrate this. Although these 20 deaths represent 35% of all SUID deaths in the first 28 days of life, they still represent only 5% of all SUID deaths.
Thus, the crux of this 2016 article in JAMA Pediatrics is a false assumption that infant deaths in the first five days of life are due to breastfeeding interventions. They used this data to argue against “accelerated implementation of the Baby-Friendly Hospital Initiative” in the US, and instead suggested government agencies should shift their support toward “monitoring breastfeeding initiation rates coupled with evidence of lactation support both during and after the hospital stay. More attention should also be placed on ensuring compliance with established safe sleep programs, emphasizing the need to integrate safe sleep practices with breastfeeding.” Sadly, given the attention their article has gotten, that their argument has gained considerable traction.
But their argument is based on a faulty interpretation of the infant mortality data. Data on the circumstances of these infant deaths is unknown to the authors, and Dr. Bass and colleagues knowingly drew a false conclusion even though Bass was told that the state was not allowed to release the location of the deaths and whether they even occurred in the hospital setting.
Furthermore, the timeline of introduction breastfeeding interventions from Massachusetts does not support a population-wide correlation between implementation of breastfeeding interventions and increase in overall death rates. Regardless, steps have since been taken to minimize such risks of SUPC from skin-to-skin contact. Finally the risks of not breastfeeding are numerous to both mother and child. The risk of SUPC is very small, and hopefully will become even smaller, but is by no means proven by Bass and colleagues, and the much greater risks of not breastfeeding, including SIDS (Sudden Infant Death Syndrome) later in infancy, must be taken into consideration when advocating any one public health intervention, such as withdrawal of the Baby-Friendly Hospital Initiative. These risks were not considered in the JAMA Pediatrics article. Focus should be on the AAP guidelines to implementing safe skin-to-skin contact to prevent SUPC, not on eliminating breastfeeding interventions with proven efficacy such as skin-to-skin contact and the Baby-Friendly Hospital Initiative.
