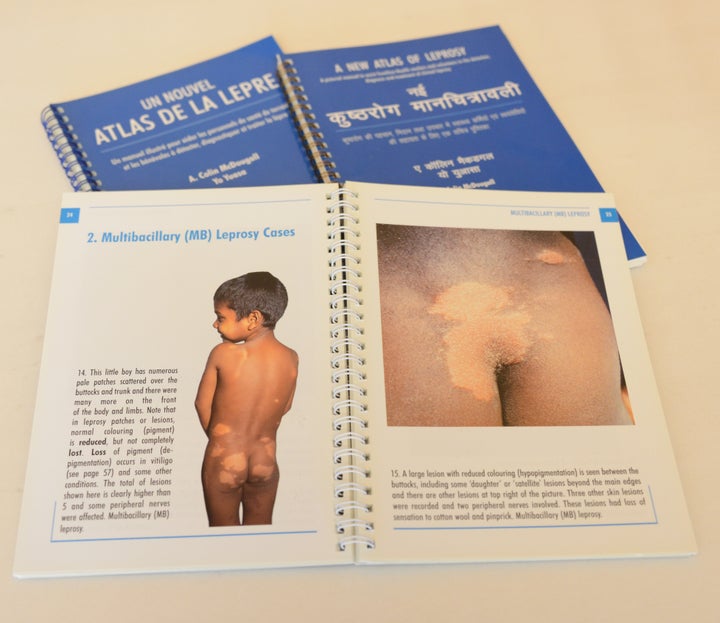
Incurable, a curse, unclean, hereditary, highly infectious, deadly, limited to undeveloped areas or tropical regions, an ancient or medieval affliction that no longer exists—all these are descriptions of leprosy that I still come across today, yet all of them are wrong.
Medically speaking, leprosy is a chronic, progressive bacterial infection caused by the bacillus Mycobacterium leprae. M. leprae is a microorganism belonging to the same genus as Mycobacterium tuberculosis, the pathogen that causes TB, and was discovered by Gerhard Henrik Armauer Hansen, a Norwegian doctor, in 1873. Hansen’s disease, as leprosy is also known, gets its name from Dr. Hansen.
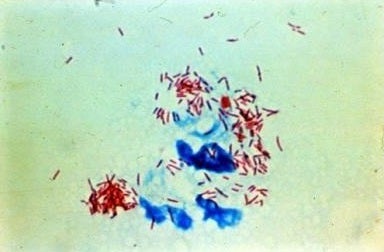
INFECTIOUS DISEASE SURVEILLANCE CENTER (IDSC), JAPAN Mycobacterium Leprae
The disease is of extremely low infectivity, with over 95% of people immune to it. Even if exposed to the bacteria, it is rare for someone to develop leprosy. It has a long incubation period; it takes an average of three years, in some cases 20 to 30 years, for the disease to manifest itself.
One of the early signs of leprosy are patches on the skin that have no feeling. If treated at this stage, leprosy is not disabling. Left untreated, however, the disease continues to damage nerves and destroys the body’s ability to feel pain, resulting in injury and festering wounds that cause secondary infections. This in turn can lead to the deformities characteristically associated with leprosy and result in permanent disability, including blindness.
For a long time, leprosy was treated with chaulmoogra oil. The oil is made from the seeds of the fruit of the chaulmoogra tree and was widely used in Southeast Asia and India as a folk remedy. Toward the end of the 19th century, it was taken up by Western medicine and its use spread in the 20th century as an injectable drug. Its therapeutic benefits were questionable, however, and in most cases there was no discernible improvement in the patient, except sometimes on a temporary basis.
In 1941, the drug Promin was used to treat leprosy patients at Carville Leprosarium in Louisiana with successful results, and leprosy became a curable disease. Yet Promin was toxic; it had to be injected and had a number of side effects. Subsequently, it was replaced by diamino-diphenyl sulfone, or Dapsone, which could be administered orally. This became the treatment of choice until the emergence of Dapsone-resistant M. leprae threatened leprosy control. As a result, multidrug therapy (MDT), which was first introduced in the early 1980s, is now the standard treatment for leprosy today.
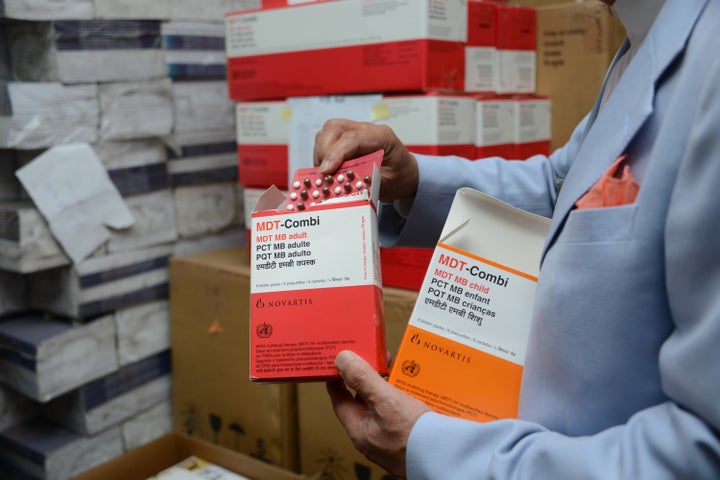
MDT is provided in blister packs, each containing four weeks of treatment for adults and children.
There are still some aspects of leprosy and its causative organism that are not yet understood. Today it is grouped among Neglected Tropical Diseases, yet in the past patients were found in colder climes such as Norway, Russia and Canada. Moreover, symptoms varied from place to place. In particular, the mechanism of transmission has yet to be precisely determined. It is not possible to cultivate M. leprae in vitro and this, combined with its weak infectivity, has made it difficult to test the route of infection. Eventually, however, science will find the answers to these and other outstanding questions about leprosy. An effective prophylactic agent may also be developed. But however far we advance scientifically and medically, that alone won’t be enough to resolve another issue—discrimination.
This article is part HuffPost’s Project Zero campaign, a yearlong series on neglected tropical diseases and efforts to eliminate them. This series is supported, in part, by funding from the Bill & Melinda Gates Foundation. All content is editorially independent, with no influence or input from the foundation. If you’d like to contribute a post to the series, send an email to ProjectZero@huffingtonpost.com. And follow the conversation on social media by using the hashtag #ProjectZero.
