This article is part of HuffPost’s Project Zero campaign, a yearlong series on neglected tropical diseases and efforts to fight them.
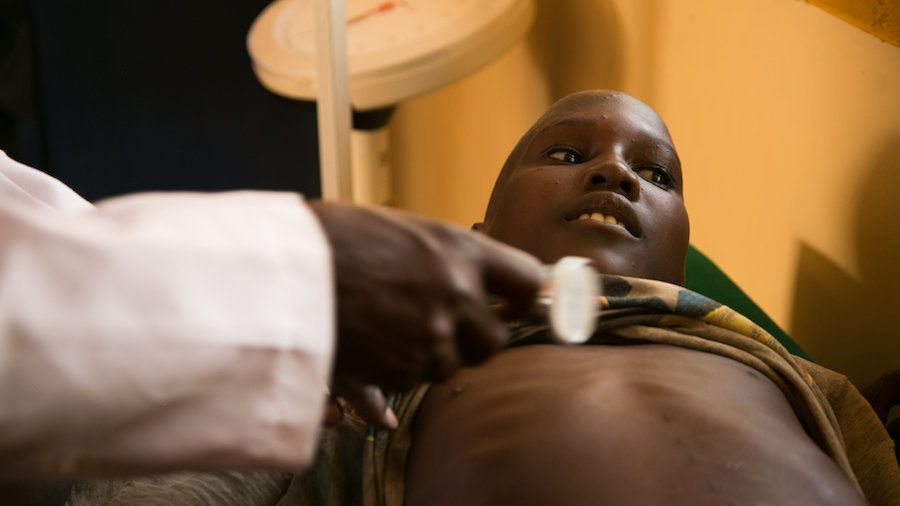
Kacheliba, KENYA ― Fifteen-year-old Pkorkor Lomerilima smiled tentatively before lifting his faded Marvel Heroes T-shirt to reveal over a dozen small scars across his slightly distended stomach.
“I was in a lot of pain when I had the treatment, and I was very scared,” he said, pointing out the scattered incisions, each about half an inch long.
When Pkorkor’s stomach began to swell and his body shivered with periodic fevers, his father took him straight to a traditional healer who promised to find a cure.

Living in Kenya’s rural Baringo region far from any clinic, Lomerilima Lokale was so hopeful the healer would make his teenage son better that he sold five goats and a camel to pay him ― a fortune for the pastoralist family.
During two expensive visits, the healer used razor blades to make multiple cuts across the younger Lomerilima’s belly, filling them with ground herbs that caused stinging.
But there was no improvement. “The money was gone,” said the boy’s father. “I didn’t know what to do.”
His son had fallen ill with the highly fatal disease visceral leishmaniasis, also known as kala azar. Transmitted by the bite of an infected sandfly and particularly common in South Asia and East Africa, this parasitic disease causes fever, enlargement of the spleen and liver, and substantial weight loss.
Getting proper medications for it can save lives, but that’s difficult in rural areas like the one where the Lomerilima family lives.
“It is almost 100 percent fatal if there is no treatment,” said Mark Riongoita, a clinical officer at the Kacheliba Hospital in West Pokot who specializes in kala azar.
“In this region, it affects the poorest and most remote. They are far away from communication and health workers so they don’t know what is wrong. Getting to the treatment facilities is a big challenge,” he added.
But unlike some sufferers in rural areas who go undiagnosed and die without treatment, Pkorkor was one of the lucky ones.
“I travelled more than 105 miles over seven hours from the hospital to Baringo,” said Isaac Nyeris, a community mobilizer who rides his motorbike into hard-to-reach areas, armed with kits he can use to test for kala azar. “When the boy tested positive, I called the hospital and they sent a vehicle.”
Visceral leishmaniasis is so common in Kenya’s Pokot and Baringo regions that locals have their own word for it. “Termes,” as the disease is known in Pokot’s local language, conjures images for English speakers of the pointy termite hills that dot the dusty landscape and are a preferred dwelling place of the sandflies that transmit the disease.

But despite the disease’s prevalence, Kacheliba Hospital hosts one of the only wards specializing kala azar treatment in western Kenya, which according to Riongoita treats up to 20 afflicted people a month. Patients like Pkorkor stay in the basic ward for several weeks and endure intense daily injections of a combination of sodium stibogluconate and paromomycin. Most patients who receive treatment recover and are able to go home.
“Before, many people lost their lives,” said Nyeris, whose own uncle died of the disease. “But today it is rare to lose a patient to kala azar unless we don’t have blood in the hospital.”
While the drugs used to beat kala azar have improved ― in Kacheliba, the treatment time has gone down from 30 days to 17 after a move to combination therapy ― countries like Kenya still rely on a potentially unstable external supply.

Across the country, public health facilities aren’t easily available, and some of the drugs used for treatment aren’t registered in Kenya.
The Geneva-based nonprofit Drugs for Neglected Diseases Initiative (DNDi), which carried out the studies that successfully reduced the standard treatment time, is helping to provide medicine to the clinic, Riongoita said.
DNDi is now focused on developing an oral alternative for kala azar patients that can replace the painful injections used in the current treatment process.
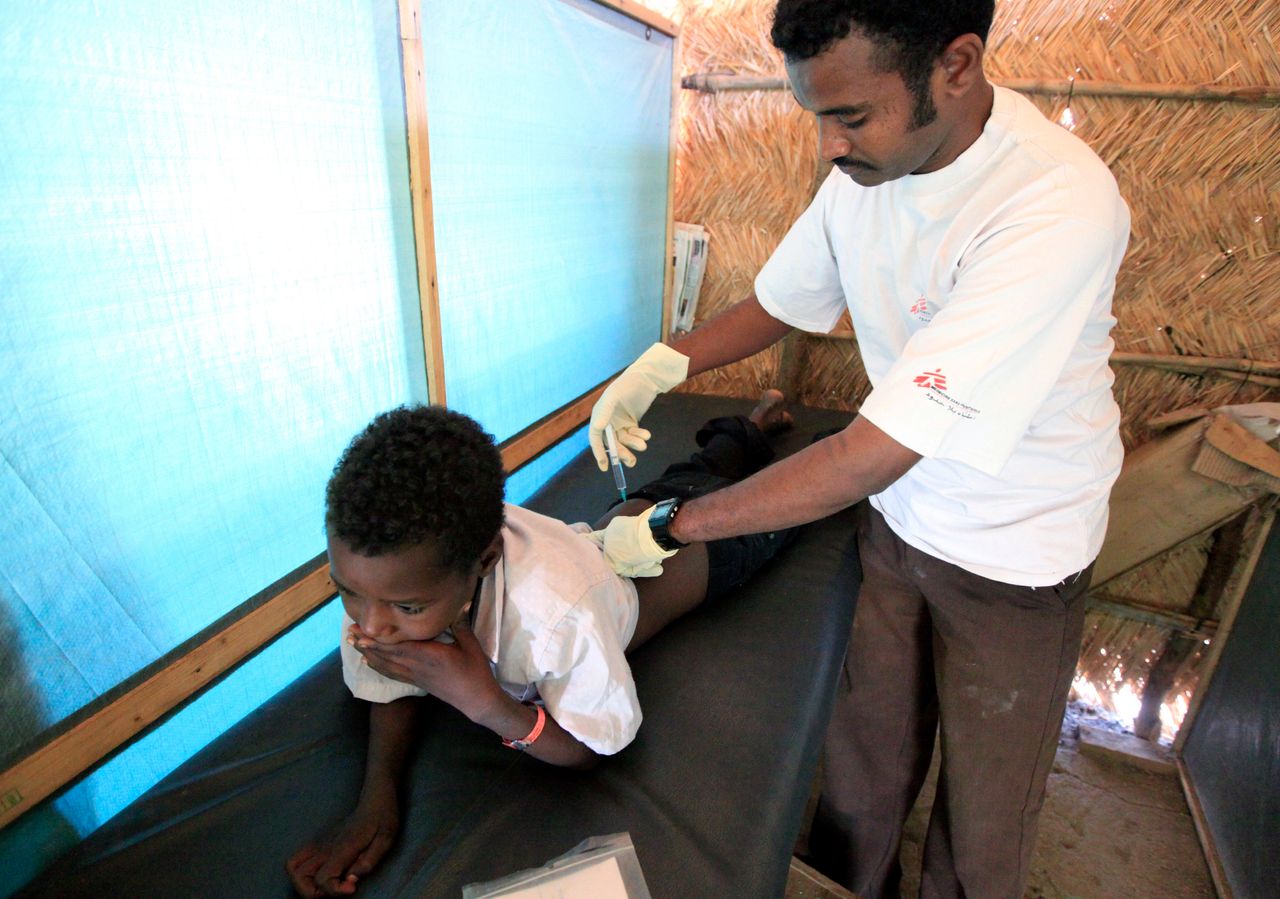
“What the patients need is an oral treatment ― so that you can say, ‘Go take this two times a day at home for two weeks and then come back’ ― that is the ultimate goal for us in DNDi,” said Dr. Monique Wasunna, the organization’s Africa director.
Leishmaniasis manifests in several syndromes ― Kenya is also suffering from an outbreak of the non-fatal cutaneous form in another part of the country. But throughout the country, outbreak locations share the same problems around remoteness and access to medical care, meaning that the true prevalence of the disease is hard to gauge.
It is estimated that ― globally ― there are up to 400,000 new cases each year, but that only 30 percent of cases are reported, according to the DNDi.
Nyeris and his bike do help bring accurate diagnoses to remote communities, but kala azar is often misidentified, and many, like Pkorkor and his father, still turn to traditional healers.
“Many people don’t understand the causes of this disease. They think it is malaria,” said Nyeris. “I use this motorbike to go into the interior to create awareness of the disease and tell people where they can get treated.”

While, the medication has some toxicity in certain cases, especially when mistakes are made around the dose, fear surrounding stories of others dying in the hospital also keeps potential patients away.
“People in the village say that if you go to the hospital and have injections, then you will die, so they prefer to go to traditional healers,” said Riongoita, the clinical officer. “They don’t get well [with the healers] but during the delay in coming to the hospital they have already developed complications.”
Lotoyok Shang’ale, an assistant chief living near Kacheliba, has become an advocate for clinical treatment in his community, encouraging members with symptoms of kala azar to go straight to hospital.
Shang’ale survived the disease himself and was successfully treated at Kacheliba Hospital, but only after enduring an excruciating traditional treatment in his home.
“They brought a woman who was said to be an expert in kala azar ― she told me that she would burn her medicine on top of my stomach and I would be healed,” Shang’ale recalled.
“After 30 minutes, the powder she put there was burning like fire. I told her it was too hot and she told me to hold on, but I could not. I ran away and jumped into the river to cool myself.”
“The traditional medicine is too painful… It leaves you even more sick,” he added. “We have told many people that treatment is available and that they should go to the hospital.”
Pkoror, still walking gingerly despite the many injections, began the long journey home by mounting the back of the bike that had helped bring him to the hospital.
While sufferers who reach the hospital generally leave cured, it’s an unpleasant experience and if a breadwinner either falls ill or has to accompany a child, already poor families are usually hit hard financially.
So it’s no surprise that, perched between Nyeris and his father, Pkorkor smiled as the bike meandered out of the hospital’s sandy yard toward Kacheliba’s main bus stop.
“I haven’t been able to play for a long time because of the illness and then the pain of the injections,” he said. “I’m looking forward to getting home and running around with my friends again.”

DNDi is a recipient of grants from the Bill & Melinda Gates Foundation, which also funds HuffPost’s Project Zero series. All content in this series is editorially independent, with no influence or input from the foundation.
If you’d like to contribute a post to the series, send an email to ProjectZero@huffingtonpost.com. And follow the conversation on social media by using the hashtag #ProjectZero.

