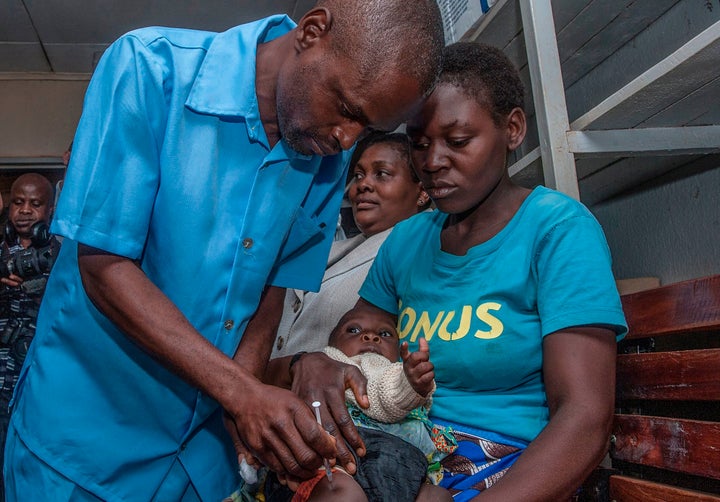
The government of Malawi has begun administering the world’s first approved malaria vaccine to young children as part of a sweeping pilot program that could save tens of thousands of lives per year across some of Africa’s poorest regions, advocates say.
The World Health Organization announced the project Tuesday, saying children in Malawi, Kenya and Ghana would soon receive injections of the vaccine, known as RTS,S. The vaccine is the only one currently on the market, although inoculation only protects about a third of people from the mosquito-born disease. But RTS,S also shows significant overall reductions in severity for those who get the injection and end up contracting malaria anyways.
“We have seen tremendous gains from bed nets and other measures to control malaria in the last 15 years, but progress has stalled and even reversed in some areas,” Tedros Adhanom, the director-general of WHO, said in a statement.“We need new solutions to get the malaria response back on track, and this vaccine gives us a promising tool to get there. The malaria vaccine has the potential to save tens of thousands of children’s lives.”
WHO estimates at least 360,000 children a year will receive the vaccination throughout the three countries. GlaxoSmithKline, the pharmaceutical company that developed the vaccine, said it would donate up to 10 million doses as part of the pilot project. It took the company more than 30 years to create RTS,S, according to The Associated Press. The vaccine was first approved in 2015.
There are more than 200 million malaria cases around the world every year, and the disease kills around 435,000 people annually, according to WHO. STAT News notes that people can be infected multiple times throughout their lives and some children who are infected by mosquitos can develop fatal cases of severe malaria.
The pilot program will continue for four years to determine how viable the vaccine is and if it does, in fact, protect children at rates seen in clinical trials. RTS,S has to be administered in four separate doses to see the reduction figures touted in trials, which some critics say could be hard to implement in the real world.
“Nobody is suggesting that this is a magic bullet,” David Schellenberg, a scientist who works with WHO’s Global Malaria Programme, told the BBC. “It may not sound like much but we’re talking about 40% reduction in severe malaria, which unfortunately still has high mortality even when you have good access to good treatment.”
The AP notes that many common vaccines, including those for polio and measles, are typically more than 90% effective.
“We know the power of vaccines to prevent killer diseases and reach children, including those who may not have immediate access to the doctors, nurses and health facilities they need to save them when severe illness comes,” Matshidiso Moeti, WHO’s regional director for Africa, said in a statement. “This is a day to celebrate as we begin to learn more about what this tool can do to change the trajectory of malaria through childhood vaccination.”
