By Allison Bond
In January 2013, as the University of Chicago prepared to unveil its newest hospital building, one last task remained: swabbing the nooks and crannies of the building, from floor to furniture to water faucets.
The people doing the swabbing were researchers collecting samples of microorganisms—the bacteria, fungi, and viruses that are essentially everywhere, including within hospital walls. As part of an initiative called the Hospital Microbiome Project, these researchers returned to the hospital throughout the year to collect nearly 12,400 samples, with the goal of mapping out the mix of microbes that populate a health-care environment.
Just as the human gut has a microbiome, so too does a hospital, the team posited. They’re among a growing group of researchers who believe that understanding hospitals’ microscopic ecological community could be key to preventing people from getting sicker in hospitals when they should be recovering. Our gut microbiome has been linked to effects ranging from Parkinson’s disease to the body’s immune response; some scientists believe a hospital’s microbiome could play a role in health, too.
It’s no secret that health-care-related infections have major health and economic costs. Every year, an estimated 440,000 infections occur in U.S. hospitals, costing nearly $10 billion. And despite efforts at keeping the building and workers’ hands and tools clean, these illnesses persist. “There are many unexplained diseases that occur in hospitals—sepsis, infections—and although we can identify a bacterium most associated with those events, we still fail to understand the specifics of the transfer of organisms in the hospital,” says Jack Gilbert, a leader of the Hospital Microbiome Project and a microbial ecologist at Argonne National Laboratory.
To answer those questions, the team collected samples from two nursing stations and a few sites in 10 hospital rooms in the new hospital building. They swabbed these areas before the building began admitting patients, then throughout the first year after the rooms were occupied. The researchers sampled the microbes in the air of the hospital and on staff members’ bodies; they also collected environmental information such as humidity and the concentration of carbon dioxide to keep tabs on the number of human occupants during all hours of the day and night. As a separate component of the project, researchers measured similar variables in a single patient room in a U.S. Army hospital in Germany.
It wasn’t the first examination of the microorganisms living in buildings. In 1887, Thomas Carnelley investigated the airborne germs in schools, sewers, and homes in Dundee, Scotland. And recently, another team of researchers examined the microbes in a hospital’s neonatal intensive care unit. Still, the Chicago project is larger-scale, enabled in part by recent advancements in gene-sequencing technology that facilitate processing myriad samples. And the project is the first not only to identify which types of microorganisms—friendly or pathogenic—dwell in a hospital, but to gauge how location and environmental factors, such as humidity, ventilation, and human foot traffic, may shape these populations over time.
“If you can understand the patterns of microbial community composition and how these change over time, you can get a pretty good idea of how to prevent some of the transmission of pathogenic organisms,” said John Chase, who has researched the microbiome at Northern Arizona University and is not involved in the Hospital Microbiome Project.
For example, only a minority of the bacteria in any microbiome—whether in the gut or in a building—poses an infection risk; the rest are bystanders (sometimes called colonizers), or even beneficial. Yet many treatments patients undergo, such as chemotherapy or antibiotics, tweak that microbial mix, potentially turning the generally harmless bacteria or fungi into disease-causing agents.
“We traditionally think the only organisms in a hospital are those that cause disease, and that when we detect them that patients are at risk of an infection,” Gilbert says. “Yet there is a surprising paucity of data supporting that.”
Instead, the infections acquired in the hospital likely stem from more just the presence of “bad” bacteria, he says. After all, plenty of people who work in the medical field unknowingly carry potentially pathogenic bacteria in their digestive systems and on their skin. Yet unlike weakened or otherwise compromised patients, they don’t fall ill because they are protected from a full-blown infection by their immune system and the other microbes that live there.
The project’s results haven’t yet been published, but Brent Stephens, a Hospital Microbiome Collaborator, revealed that certain types of bacteria commonly found on human skin, such as some species of staphylococcus, streptococcus, andcorynebacterium, became much more abundant after the hospital opened. Meanwhile, Pseudomonas, which can cause bladder, wound, and lung infections, and which is less often a skin colonizer, became less plentiful. That indicates the hospital environment and the humans within it mingle in a way that fosters the exchange of bacteria.
This jibes with prior research, which has shown that humans deposit and acquire microbial mementos from buildings via the skin. “Surprisingly quickly, when you enter a room, you start picking up microbes, and the room picks up microbes from you,” says Daniel Freedberg, a gastroenterologist and assistant professor of medicine at Columbia University Medical Center in New York City.
Freedberg believes a map of a hospital’s microbiome—something that delineates the surfaces where certain bugs thrive—could provide valuable insights into the environmental conditions that allow microbes to flourish. He led a recent study that indicates the hospital environment could indeed play a role in infection transmission. The research linked inheriting a hospital bed from a patient who had received antibiotics to a higher risk of infectious, potentially deadly diarrhea caused by clostridium difficile, a bacterium whose spores thrive in human guts when normal bacteria have been decimated by antibiotics.
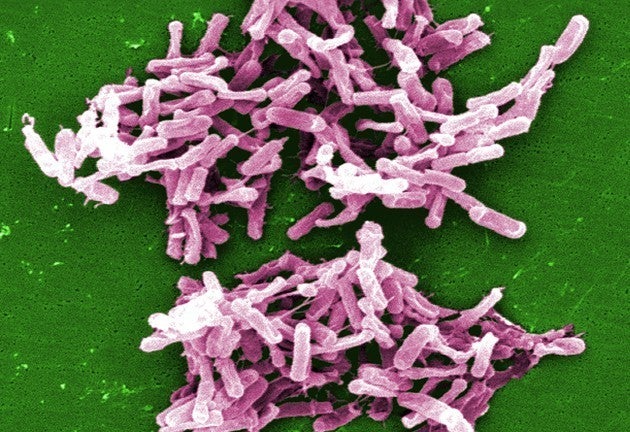
A cluster of clostridium difficile bacteria
The study didn’t identify the reason for the association between antibiotics and infection—but it points to the possibility that the medicines one patient received altered his or her gut microbiome, and that this modified mixture of bugs was then passed on to the next patient in the bed, predisposing this second patient to c. difficile. Alternatively, one patient could have directly passed the bacterium to the next by way of the mattress or bedrail. Although hospital staff cleaned the bed between patients, c. difficile spores are notoriously tough to kill. (Gilbert, for his part, is not convinced cleanliness alone will ever eliminate infections in hospitals.) Both explanations speak to the effects that altering the gut microbiome of one patient can have on another, and how the hospital may serve as a vector for disease.
“The ultimate goal is to be able to understand whether there are communities of microbes that can affect human health,” said Chase, “and what kinds of conditions go into creating those communities.”
This story originally appeared on TheAtlantic.com.
More from The Atlantic: The Life-Changing Magic of Mushrooms, The Different Stakes of Male and Female Birth Control