Small Drop in Vaccination Could Triple Number of Measles Cases in United States
Despite the societal benefits of vaccines and the known consequences of not using them, it is astounding that delays in acceptance or the refusal of taking vaccines exists in various parts of the world. Vaccine hesitancy is a major public health concern that needs to be highlighted.
Given increasing parental decisions not to vaccinate their children, investigators from the U.S. wanted to understand what the effect of small reductions in vaccine coverage on measles cases were. Nathan Lo, from the Stanford University School of Medicine in California, estimated the disease burden and economic costs associated with declines in the measles-mumps-rubella (MMR) vaccination rate.
“Routine childhood vaccination is declining in some regions of the United States due to vaccine hesitancy, which risks the resurgence of many infectious diseases with public health and economic consequences,” the authors wrote in the journal JAMA Pediatrics.
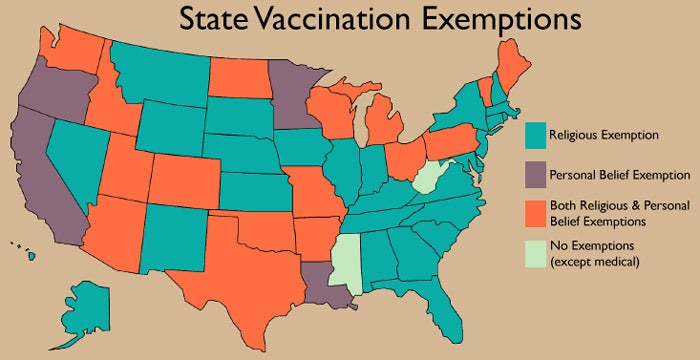
US State Vaccine Exempotions
The study set out to find the number of measles cases in U.S. children. From there, researchers used vaccine data from the Centers for Disease Control and Prevention to simulate county-wide MMR vaccine coverage for children ages 2 to 11. They then used a mathematical model to estimate the impact of decreasing vaccination rates, taking into consideration the infectiousness of the disease while simulating situations in which measles is introduced by a traveller into the U.S. They calculated the number of cases that would be expected if the MMR vaccination coverage was to decline. The researchers repeated this process thousands of times, changing the variables and scenarios each time for each state. The model was checked for its accuracy using data on measles cases from England and Wales.
At baseline, MMR vaccine coverage was at 93 percent, and the prevalence of non-medical exemptions was at 2 percent. This would yield 48 measles cases annually in this age group across the U.S. However, if vaccine coverage dropped by 5 percent, the estimated number of measles cases would increase to 150, a threefold increase. This could cost the public sector $2.1 million. That’s $20,000 per case of measles. Still, the researchers warned that results of the study may be underestimated! The study did not take into account other variables, such as cost of illness, parental time off work, hospitalization, or other societal factors.
Peter Hotez, Dean of the National School of Tropical Medicine at Baylor University in Texas, added: “I think our study is a wake-up call for what we can expect in the coming months and years as vaccine coverage rates continue to decline in the 18 states that now allow non-medical or philosophical belief exemptions.”
While childhood vaccination rates remain high in the U.S., there are areas where non-medical exemption policies are translating into decreased immunization coverage. Currently, 18 out of 50 states allow non-medical personal belief exemptions to childhood vaccinations. Moreover, all but two states offer non-medical exemptions on religious or philosophical grounds. Given the trends in declining vaccine coverage, researchers predict that preventing non-medical personal belief exemptions would bring the annual number of cases down to 38. This, they say, would be “an effective strategy to mitigate annual measles cases and costs.”
The study’s conclusion was supported by a recent study that examined the association between vaccine coverage and measles outbreaks in Denver, Colorado. This study found that making non-medical vaccine exemption requirements more stringent (therefore, reducing non-medical exemptions) would reduce measles cases and economic consequences.
Plummeting vaccination rates have prompted several countries around the world to adopt firm policies. In Australia, the “No Jab, No Pay” bill mandates that only parents of children (less than 20 years of age) who are fully immunized or are on a recognized catch-up schedule can receive the Child Care Benefit, the Child Care Rebate, and the Family Tax Benefit. “No Jab, No Pay” came after the 2012 whooping cough epidemic in Australia. That same year, measles, a disease mostly eliminated through vaccines, returned.
In Germany, kindergartens are obligated to inform authorities if parents fail to prove they have sought vaccination advice from a doctor. The measure is part of a government effort to improve vaccination rates.
In France, parents will be legally obligated to vaccinate their children starting in 2018. French Prime Minister Édouard Philippe said that it was “unacceptable that children are still dying of measles” in a country where some of the earliest vaccines were pioneered.
This move follows a similar initiative in Italy, where parents are required to show proof of vaccinations to gain admission into preschools. Parents, whose children are of mandatory school age, could face fines of up to 500 euros ($588) for noncompliance.
Measles is an extremely contagious and potentially fatal disease that can spread very easily, particularly to those who are not immune
Measles is an extremely contagious and potentially fatal disease that can spread very easily, particularly to those who are not immune. It can spread through direct contact, via a cough or sneeze, or by way of contact with shared objects and surfaces. In 2000, measles was declared eliminated in the U.S. but, in the past few years, outbreaks have started occurring annually. According to the U.S. Centers for Disease Control and Prevention (CDC), measles cases have ranged from a low of 55 (2012) to a high of 667 (2014). The CDC also noted that in the majority of these measles cases, people who had not been vaccinated were those who became infected.
Measles is highly contagious and 90 percent of people not immune will get infected by someone who has it in close proximity. Therefore, there is an ethical argument to be made that everyone who can get vaccinated should get vaccinated – not only to protect themselves but to protect those who can’t, through means of herd immunity.

The more people who are vaccinated, the fewer opportunities a disease has to spread.