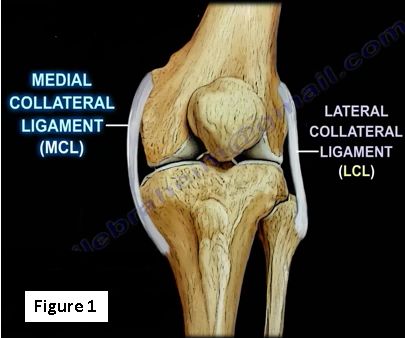
The medial collateral ligament is one of four major ligaments of the knee (MCL, LCL, PCL and ACL) (Figure 1)
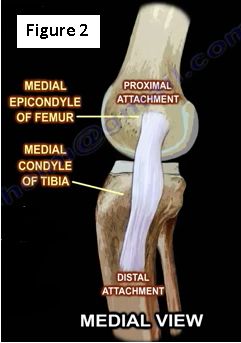
The medial collateral ligament extends from the medial epicondyle of the femur to below the medial condyle of the tibia. The MCL is a static stabilizer composed of superficial (primary) and deep (secondary) portions that are restraints to valgus stress. The proximal attachment is the posterior aspect of the medial femoral condyle and the distal attachment is the metaphyseal region of the tibia, about 5 cm distal to the joint, lying beneath the pes anserinus (Figure 2).
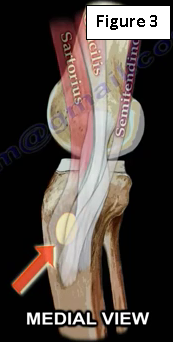
The deep MCL is the secondary restraints to valgus stress. It inserts directly into the edge of the tibial plateau and meniscus. It may be separated from the superficial layer by a bursa. The joined tendons of the sartorius, gracilis, and semitendinosus muscles cross on top of the lower part of the MCL. The pes anserine bursa is located anterior to the insertion of the medial collateral ligament into the tibia (Figure 3).
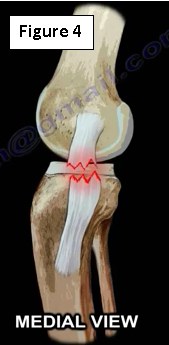
The MCL’s primary function is to be a restraint to valgus stress. The MCL is the most commonly injured ligament of the knee (Figure 4).
The typical mechanism of injury of the MCL is due to a valgus and external rotation force. A direct blow to the knee usually causes a complete rupture of the MCL. The rupture may occur proximally or distally. Tears of the proximal MCL have a greater healing rate. Tears of the distal MCL may not heal well (similar to a Stener Lesion of the thumb) (Figure 5).

Associated Conditions
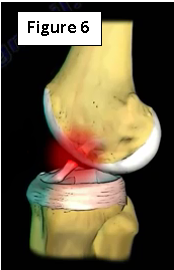
Injuries to the ACL comprise up to 95% of associated injuries (Figure 6). A rupture of the ACL causes anterolateral rotatory instability. The majority of MCL injuries that are associated with ACL injuries are Grade III complete ruptures, which demonstrate no end point with valgus stress at 30° and 0° of knee flexion on examination.
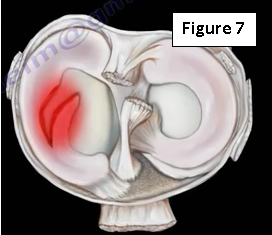
Up to 5% of isolated MCL injures are associated with meniscal tears (Figure 7). It is not a common injury.
Classification of MCL Sprains
MCL sprains can be classified into three different grades. A Grade I is a sprain, stretch injury. A Grade III is described as a partial tear of the MCL. A Grade II is described as a complete tear of the ligament. There is no end point with valgus stress at 30° of knee flexion.
Presentation
There will commonly be a “pop” sensation. The patient will have pain and tenderness usually superior to the joint line. During the physical examination there will be tenderness along the medial aspect of the knee. There will also be ecchymosis and knee effusion.
Testing for MCL Injury
A positive valgus stress test at 30° of knee flexion indicates an injury to the superficial MCL. An opening around 1 cm indicates a Grade III complete tear of the MCL. A positive valgus stress test at 0° of knee extension indicates a posteriormedial capsule or cruciate ligament injury in additional to MCL injury (means a combined injury). The physician must always evaluated for other injuries (ACL, PCL, or medial meniscal tear).
Imaging
Pellegrini-Steida Syndrome
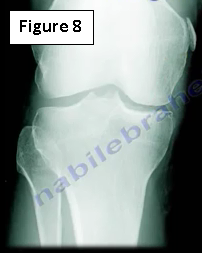
Radiographs are usually normal however they may show calcification at the medial femoral site (Pellegrini-Stieda Syndrome) (Figure 8). There will be calcification due to chronic MCL deficiency at the medial femoral insertion site.
Pediatric patients with a knee injury and suspected Salter fracture should get stress view x-rays to rule out a growth plate injury. Growth plates are weaker than ligaments (may use MRI instead of stress views).
An MRI is the study of choice as it identifies the location and extent of the MCL injury.
Treatment
Treatment should include NSAIDs, rest and therapy. A minor sprain of the MCL will require therapy with return to play in about one week. The patient may use a brace if the injury is Grade II, and they will return to play in about 2-4 weeks. With a Grade III injury, the patient can return to play in about 6-8 weeks.
Surgery is utilized in Grade III injuries with multiple ligament injuries, especially with a distal avulsion fracture. If there is chronic instability with opening in full extension, a reconstruction will be done. An additional arthroscopy may be needed to rule out any associated injuries.
In a combined MCL and ACL injury, surgery for the ACL is usually delayed until the MCL heals (up to 8 weeks). The patient will use an ACL brace.
Complications include stiffness and loss of motion. Laxity is also associated with distal MCL injuries.
Functional bracing may reduce an MCL injury in football players, particularly interior linemen.
For more information visit my YouTube Channel
