
People who suffer from migraines may want to check if they’re getting enough of certain vitamins and nutrients.
While it isn’t yet clear if supplementation might help prevent migraines, new research presented at the Annual Scientific Meeting of the American Headache Society in San Diego revealed that a significant portion of kids, teens and young adults who suffer from migraines are mildly deficient in vitamin D, riboflavin and coenzyme Q10.
"We think that there is a likelihood that patients with migraines are more likely to be deficient in these vitamins than the general population," lead study author Dr. Suzanne Hagler, a headache medicine fellow in the neurology division at the Cincinnati Children’s Hospital Medical Center, told The Huffington Post.
If future studies find that these deficiencies do indeed play a role in migraines, Hagler said that a healthy diet that samples from diverse food groups, as well as vitamin and nutrient supplements, could be key in helping to prevent or treat migraines, perhaps alongside standard migraine medicines.
The findings have not yet been published in a peer-reviewed journal, and should be considered preliminary. Hagler plans to submit the report for consideration this summer.
In her research, she examined baseline blood samples from a database of 7,420 patients at the hospital’s headache center and analyzed them for levels of vitamin D, riboflavin, coenzyme Q10 and folate -- all nutrients or vitamins that have been linked to migraine risk in past research. While folate results weren't suggestive, about 51 percent of patients were just at or below average levels of coenzyme Q10, 16 percent had less than average levels of riboflavin, and 31 percent had less than average levels of vitamin D.
Female patients were more likely to have deficiencies in coenzyme Q10, which is found in meat, fish, nuts and some fruits and vegetables. Male patients were more likely to have deficiencies in vitamin D, a vitamin the body makes when exposed to the sun. Those with chronic migraines were more likely to be deficient in both coenzyme Q10 and riboflavin, which is part of the vitamin B group, compared to those who suffered episodic migraines.
But because many of the patients were ultimately treated with both vitamin supplements and preventive migraine medications, Hagler couldn’t tell whether their migraine improvements were due to the vitamin supplements or the migraine medications.
Past research on migraines and their relationship to nutrient and vitamin deficiencies is mixed. A 2012 review of existing studies suggested that treating migraines with preventive doses of riboflavin and coenzyme Q10 has a positive effect, and in 2015, a randomized, double-blind and controlled clinical trial suggested the same for vitamin D supplementation. But other research, like a 2014 review of past vitamin D studies, suggests there is no reliable scientific support for the link between the vitamins and migraine prevention.
However, Hagler pointed out that many of these studies are often conducted among small populations, and researchers don't find out if the participants are deficient in certain vitamins or nutrients before beginning supplementation.
"The question is, would they have gotten more positive results had they treated patients who were actually deficient in those vitamins, or does not it really matter?" she asked.
Dr. Wade Cooper, director of the Headache and Neuropathic Pain Clinic at the University of Michigan, was not involved in Hagler's research but attended her presentation. He was impressed that such a large portion of the participants in the study had vitamin or nutrient deficiencies, but said it wasn't surprising; Cooper already uses vitamin and nutrient supplements to help treat patients for migraine, and Hagler's findings confirmed his clinic's decision to continue doing so.
Cooper says that these vitamin deficiencies could hint at the root causes for participants' migraines: "The finding of several vitamin deficiencies in patients with migraine suggests an underlying gut absorption issue, most likely related to inflammation."
Hagler also said that the possible link between vitamin deficiencies and migraines, especially when it comes to coenzyme Q10 and riboflavin, could mean that migraines are the result of abnormally functioning mitochondria, an organelle that creates energy for cells. Coenzyme Q10 and riboflavin are both extremely important in mitochondrial function, she explained.
The best way to sort out all these questions would be to conduct a large, randomized and controlled trial among migraine sufferers to see if specific vitamin supplementations can prevent or reduce migraines, Hagler concluded. Her center has no plans to conduct such a study right now, but she notes that unlike new pharmaceutical drugs in trials, vitamin supplements are already available over the counter and are very safe to take.
What researchers do know is that there are many reasons people experience migraines. Some of them are hormonal, like the menstrual migraines some women experience right before or at the beginning of their periods. A drop in estrogen increases the risk in migraine in women, and strategies to prevent this include using preventive medication, taking birth control pills that let a woman skip her period entirely, or using hormonal supplements that make up for the estrogen drop.
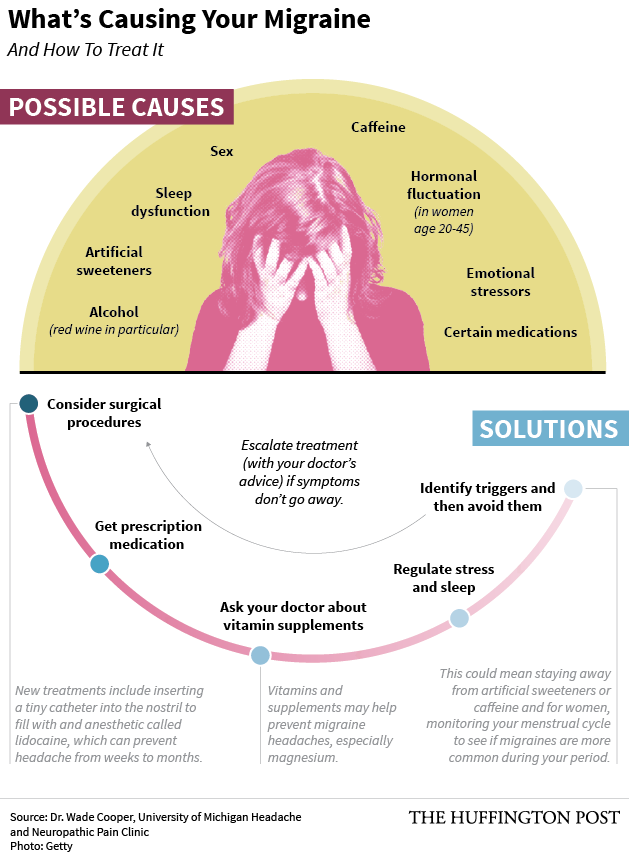
Other migraines can be triggered by food and drink like alcohol, artificial sweeteners and caffeine. Sleep dysfunction, emotional stress and muscle aches can also contribute to migraine risk. Experts say the most fundamental changes you can make to your lifestyle include regulating stress and sleep, as well as learning to recognize your migraine triggers and avoiding them. If lifestyle changes aren’t enough, a headache doctor can help guide you toward vitamin supplements, prescription medications and perhaps even surgical procedures to help stop migraines.
