A new report analyzing the drugs involved in fatal overdoses once again emphasized fentanyl’s role in the United States’ opioid crisis and highlighted a point frequently made by public health experts: Most people who fatally overdose have more than one drug in their system.
In 2016, about 70 percent of fatal overdoses involving fentanyl or heroin involved another drug as well, and roughly 74 percent of fatal overdoses involving cocaine also involved one or more other drugs.
“We’ve had a tendency to think of these drugs in isolation. It’s not really what’s happening,” said Dr. Holly Hedegaard, lead author of the report and injury epidemiologist at the National Center for Health Statistics.
More than 72,000 Americans died of drug overdoses in 2017, according to the U.S. Centers for Disease Control and Prevention.
Most reports on drug overdose deaths only determine what class of drugs were involved. The new report, published Wednesday by the National Center for Health Statistics, analyzed the text of death certificates and compared it with National Vital Statistics System data, drilling down to determine the specific drug ― not just the class of drugs ― involved in overdose deaths from 2011 to 2016.
What researchers found mirrored news reports in recent years. Oxycodone, which was the most common drug cited in fatal overdoses in 2011, was eclipsed by heroin from 2012 to 2015, and then fentanyl in 2016. On average, the U.S. death rate involving fentanyl increased about 113 percent per year from 2013 to 2016.
In most of these cases, the researchers found that more than one drug was used, and from those data they were able to identify the most common combinations of drugs that led to fatal overdoses.
Though it’s impossible to tease out what specific effect one drug had versus another used at the same time (or what other medical factors may have contributed to the deaths), better understanding these drug combinations “helps us identify potential areas of risk,” Hedegaard said. For instance, about 40 percent of cocaine deaths also involved fentanyl.
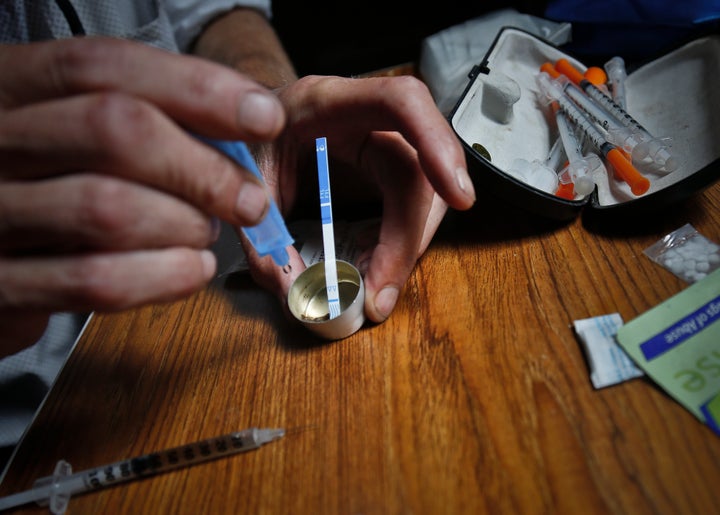
Hedegaard and her co-authors used the same death certificates that the CDC typically uses for overdose reports but went deeper in their analysis, scouring the records for drug misspellings, chemical names, brand names and street names recorded by coroners and medical examiners.
The amount and quality of information on the reports varied widely. Death investigations, resources and reporting requirements differ from county to county and state to state, and medical examiners and coroners are a patchwork of officials and an unregulated group. In some municipalities, coroner is an elected or appointed position, not necessarily a medical doctor.
Though reporting by medical examiners and coroners improved over the course of the report, Hedegaard noted, in 2016, 15 percent of drug overdose death certificates still didn’t include any specific drug.
After an in-depth analysis of the information, the researchers also found that certain drugs were more likely to be the cause of death in unintentional overdoses, while others were more likely to be implicated in death by suicide. In 2016, the street drugs fentanyl, heroin and cocaine were most frequently recorded in unintentional fatal overdoses, while prescription and over-the-counter medicines, including oxycodone, diphenhydramine, hydrocodone and alprazolam, were most frequently recorded in deaths by suicide.
Better understanding those patterns could help experts and policymakers who are working to end the nation’s suicide and overdose crises.
“For folks who work in prevention, having information helps them think about what prevention tactics to use or approaches that might be effective,” Hedegaard said.