All your fears, stresses and anxieties have one thing in common. They are sensed by a pair of pea-sized patches of neurons, called the amygdala, sitting deep inside your brain. So what if you could control your amygdala? What if you could change your brain and become calmer and braver?
That idea has a particular appeal for people suffering from depression, anxiety and post-traumatic stress disorder. But it’s easier said than done. The amygdala is an old part of the brain that does its job automatically, without much care for commands from more conscious parts of the mind. You can’t just tell an oversensitive amygdala to quiet down.
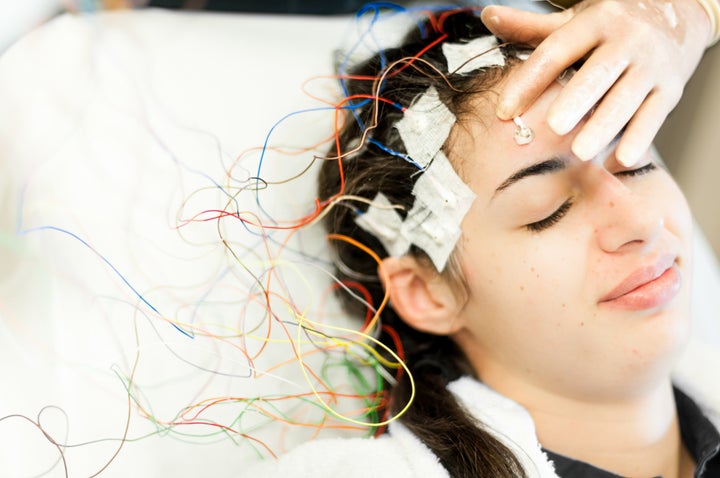
But a brain training technique known as neurofeedback might help people find a way to change such involuntary and automatic brain processes. In recent years, the technique is being developed and refined to address mental health issues. The treatment involves monitoring a person’s brain activity in real time using electroencephalography (EEG) or functional MRI brain scans, and showing those patterns of activity to the person so they can try to boost or reduce them ― basically, changing how their brain functions.
In a new study published last month in Biological Psychiatry, researchers set up a series of experiments to use neurofeedback to teach several dozen people how to regulate their amygdala activity.
“People were able to use this new EEG model to learn how to control their brain activity in a deeply located brain area, the amygdala,” said Dr. Talma Hendler, a psychiatrist and neuroscientist at the Tel Aviv Center for Brain Functions in Israel.
“This method "opens a wide horizon of treatment possibilities for the mentally ill, but also for everyone on a daily basis as an empowering tool for mental activity and well being.””
- Dr. Talma Hendler, Tel Aviv Center for Brain Functions
Reading brain signals from deep parts of the brain is difficult, especially with a cheap and accessible method. Functional MRI, or fMRI, can access these areas, but the device is a complex, gigantic magnet that you can’t just set up at home, even if you could afford it.
EEG, on the other hand, is cheaper and simpler. It mainly involves a few electrodes placed on the scalp. The downside of EEG is that it can’t accurately zoom in on structures deep in the brain.
So, the researchers combined the two methods. They used the detail provided by fMRI to tease out the amygdala’s signal from the electrical activity picked up by the EEG.
“[This method] enables home-based imaging that [targets] brain regions relevant for our mental health,” Hendler said. “It opens a wide horizon of treatment possibilities for the mentally ill, but also for everyone on a daily basis as an empowering tool for mental activity and well being.”
For the experiments, Hendler and her colleagues asked the volunteers to listen to a sound. They were then instructed to lower the volume of the sound by “exercising mental strategies.”
It sounds like a vague instruction. What are the mental strategies that can, seemingly telepathically, control the volume of a sound? No one really knows, and that’s sort of the point. People have to try many different ways of thinking ― thereby changing their brain activity ― until they stumble upon a desired activity pattern.
What the participants didn’t know was that the volume of the sound was programmed to change based on the electrical activity of their own amygdala, and it would lower if the participants managed to dial down that activity. In other words, they were listening to their own amygdala’s firing, disguised in a sound.
A series of tests afterward showed that this game seemed to help participants become more capable of regulating the activity of their amygdala. In response to viewing a series of images, for example, the participants’ amygdalas seemed less sensitive compared to those of people in another group given a fake neurofeedback treatment.
The participants in this study were healthy. But Hendler believes that people with mental health problems, too, would respond to training with neurofeedback.
“We already have indication for this (unpublished yet) that people suffering from depression, chronic pain and post traumatic disorders are able to learn and greatly benefit from such training,” Hendler said.
If the method proves useful in treating mental health conditions in the future, this low-cost, personalized treatment could be used at home to complement and sometimes substitute medications, Hendler said.
