
Another far-fetched lawsuit against the Affordable Care Act won a victory in the lower courts on Wednesday. And while few members of the legal establishment have taken this lawsuit seriously, few members of the legal establishment took the last one seriously. That case, King v. Burwell, made it all the way to the Supreme Court before failing.
So what happens if this latest legal assault does that -- and more? What if it actually prevails? At the moment, it's really hard to tell.
A ruling for the plaintiffs could have little or no effect. Or it could mean higher prices and deductibles for several million people now buying insurance on their own, and maybe even a less stable market. Ultimately, the answer would depend on reactions -- by insurers, the courts and Congress -- that are simply impossible to predict right now.
At stake in this latest case, House v. Burwell, is the special financial assistance that President Barack Obama’s signature health care law provides to some people buying coverage through the Obamacare marketplaces, in order to reduce their out-of-pocket expenses. Few people know the law even provides such assistance, even though it makes a big difference for those who benefit from it.
Here’s why: The insurance plans available through the law’s marketplaces, like most private insurance plans, come with deductibles and co-payments. If you pick up a prescription, for example, you probably have to pay some money out of your own pocket before your insurance coverage kicks in. It could be just $5 or $10 -- or much higher, like $50 or $100, for some specialty medications. You might even have to pay the full cost, which could be hundreds of dollars, if you haven’t met your overall deductible for the year. You’ll also have to pay out of pocket when you visit the doctor, go to the emergency room, or get tests and procedures. These, too, can get expensive.
The health care law puts a maximum on those out-of-pocket expenses -- something that didn’t exist before. But those limits are $6,600 for individuals and $13,200 for families this year -- expenses that could cripple consumers without wages or savings to cover such bills. That’s why the law requires that insurers offer more generous "silver level" policies, with no additional costs, to consumers with incomes below two and a half times the poverty line -- which, for a family of three, is about $50,000 a year.
The difference is substantial. According to an analysis from the Henry J. Kaiser Family Foundation, a family with the most protection available would owe, on average, just $168 in out-of-pocket expenses for an emergency room visit -- roughly half what that family would owe with a standard silver-level policy. The details can vary, from household to household and from plan to plan. But, overall, the extra financial protection can translate to savings of thousands of dollars a year.
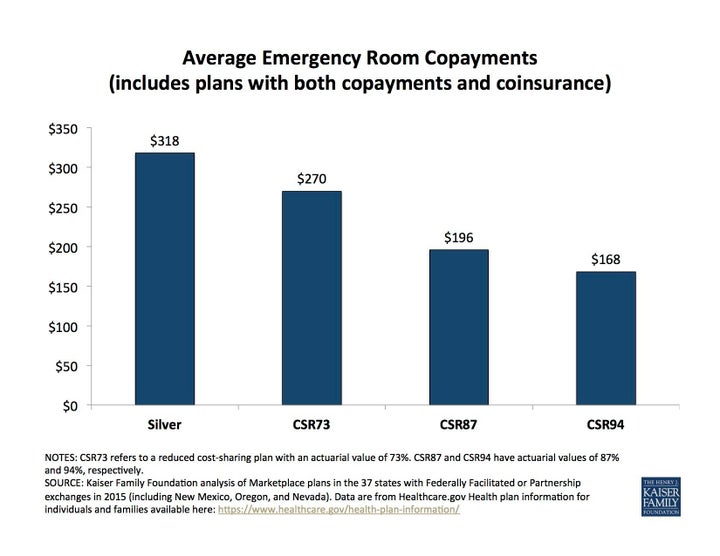
Lower-income consumers buying coverage through Affordable Care Act marketplaces can qualify for plans with less cost-sharing. Here's what the emergency room co-payments look like in three of those plans, relative to the standard silver-level policy.
To compensate insurers for reducing out-of-pocket expenses, insurers get special payments from the federal government. Money flows directly from the Treasury Department to the Blue Cross, Aetna and other private insurers. It's the propriety of those payments that the plaintiffs in the lawsuit, the Republicans who control the House of Representatives, are challenging. Congress never appropriated money for those payments. As a result, House Republicans say, the federal government has no right to spend it. The Obama administration contends the spending is mandatory, much like Social Security checks are. That would render a separate appropriation unnecessary.
The nature of the case -- specifically, one branch of government suing another -- is its key legal vulnerability. As HuffPost’s Cristian Farias has noted and many legal scholars have pointed out, courts generally refuse to consider such cases on the merits, because branches of the government lack “standing.” If lawmakers have a beef with the president, the thinking goes, they have plenty of constitutional and political tools at their disposal. They don’t need to sue.
In Wednesday’s ruling, Rosemary Collyer, a federal district judge in the District of Columbia, nevertheless agreed to let the lawsuit proceed. The government has already indicated it will appeal Collyer's decision on the standing question. The case could wind up at the Supreme Court, where Chief Justice John Roberts has already hinted he is exasperated with health care lawsuits from fellow conservatives trying to undermine the health care law. That is one reason so many legal scholars, even those hostile to the Affordable Care Act, think Collyer’s decision is unlikely to prevail.
If the scholars are wrong and the lawsuit somehow succeeds, on the merits as well as on standing, then a variety of scenarios are possible -- and it’s tough to figure out which one is most likely.
Under the terms of the health care law, consumers who qualify for that extra assistance are entitled to it, with or without congressional appropriations. So if your income is below 250 percent of the poverty line and you buy a silver plan through the marketplace, then you get that extra help with out-of-pocket costs -- no matter how the courts rule.
In addition, the law also entitles the insurers to their money, regardless of congressional action. “What that means in non-legalese is that Congress has promised to pay them money -- whether or not there’s an appropriation,” said Nicholas Bagley, a University of Michigan law professor and regular contributor to The Incidental Economist blog. “And health plans can sue the government in the Court of Federal Claims to make good on that promise.”
According to Bagley,
...the question isn’t whether the government will pay the cost-sharing reductions. It’s when. If the government is right, Treasury can pay health plans on a “periodic and timely” basis. If the House is right, health plans have to file thousands upon thousands of duplicative lawsuits to get the money.
That legal process, naturally, could be slow and cumbersome -- enough that insurers might have to take other actions. The most extreme would be to pull out of the insurance marketplaces altogether. Alternatively, they could raise premiums to cover their new losses.
Some would feel the effects more than others; a separate set of subsidies dictate the premiums for consumers in households with incomes of less than four times the poverty line. But there's always the possibility that higher premiums could create more serious instability, by scaring away some of the relatively healthy consumers whose premiums offset the cost for beneficiaries with serious medical problems. Jed Graham, of Investor’s Business Daily, has a piece contemplating such an outcome.
Richard Kogan and Edwin Park, analysts at the Center on Budget and Policy Priorities, argued that the damage from a ruling could be real -- but limited:
To be sure, marketplace enrollees with incomes above 400 percent of the poverty line could be hit hard with substantial premium increases, as could people enrolled in individual-market coverage outside the marketplaces. Some likely would drop their coverage; the ranks of the uninsured would rise. In addition, the risk pool in the marketplaces likely would experience some adverse selection (with the risk pool becoming less healthy, on average), and some insurers could withdraw from the marketplaces. Yet even in this very unlikely scenario, the outcome would not be a wholesale collapse of the ACA’s structure, as would likely have occurred if the plaintiffs in King v. Burwell had prevailed and premium subsidies were unavailable in the federal marketplaces.
Timothy Jost -- a law professor at Washington and Lee University and, like Bagley, a close student of the law -- was less sanguine in an assessment he wrote for Health Affairs:
Burdened with this cost without reimbursement through the CSR payments, many insurers would cease to offer marketplace coverage. Those that remained would have to raise rates dramatically to ensure solvency. Although much of the increase would be covered by the premium tax credits for low-income individuals, higher-income enrollees could face unsustainable increases. This could well put the marketplaces into a death spiral, where healthy people would drop coverage leaving only high cost patients behind.
One last possibility is that Congress could react to a ruling for the plaintiffs by formally appropriating the money that the law already promises and that the federal government is already spending. But cases take a long time to work through the courts and a final ruling, on the merits, is likely at least two years away. By that point, Republicans might control the presidency as well as both chambers of Congress. They might be willing to do nothing, and say the ensuing problems are merely more proof that the law is a “fiasco.”
Of course, more than just out-of-pocket assistance might be at stake. The whole health care law could face full repeal -- and that, without a doubt, would be devastating to millions.
