By: Harriet Miller, CPN, Winnie Palmer Hospital for Women & Babies
Published: 06/01/2015 04:42 PM EDT on LiveScience
Harriet Miller, CPN, a nurse scientist at the Center for Nursing Research at Winnie Palmer Hospital for Women & Babies at Orlando Health, contributed this article to Live Science's Expert Voices: Op-Ed & Insights.
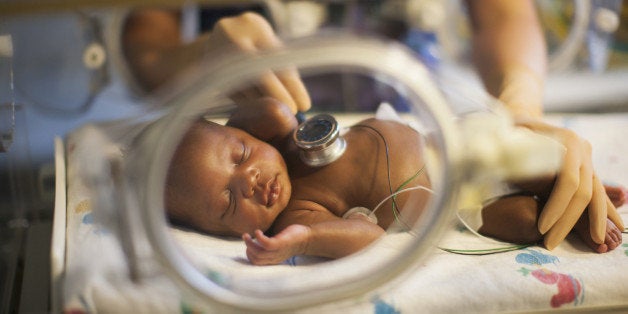
Not long after I became a nurse in a neonatal intensive care unit (NICU), I began to notice something disconcerting: The infants in my care, like all babies, cried when they were tired, scared or in pain. But unlike other babies, I couldn't hear them.
The problem was their endotracheal tube. This tube is necessary to provide these newborns with oxygen, but because it passes between their vocal cords, it prevents them from making audible sounds when they cry — something that newborns need to do quite frequently. It's estimated that in the first two weeks after admission, the average baby will undergo 16 painful or stressful situations each day.
Managing pain for preemies
Blood tests from painful heel sticks are common in neonates, but even routine events such as a physical examination or changing a diaper can induce stress, and these babies may actually perceive such events as painful.
If pain isn't managed properly, it can lead to negative long-term consequences in growth and development, but options for dealing with this pain are limited. The use of morphine for pain appears to be safe when it comes to the baby's development, but it has not been proven to prevent morbidities associated with pain, and therefore continuous use is not recommended.
Another option for providing comfort and managing pain in babies is the use of a pacifier. The sucking reflex is vital to newborns. Not only does it allow them to feed instinctively, but non-nutritive sucking (the use of a pacifier) is a powerful coping mechanism. It's hypothesized that the mere act of sucking on a pacifier may actually block the body's ability to transmit the sensation of a painful impulse back to the brain.
In an effort to help comfort the babies in my care and better manage their pain, I would give them pacifiers. But this rarely helped. I noticed that either their mouths were too small to accommodate both the endotracheal tube and the larger nipple of a standard-size pacifier, or the pacifier's flange would press against the tube and force the nipple out of the mouth. That only led to more stress and frustration.
Enter the preemie pacifier
So, I decided to create my own pacifier, one specifically designed for intubated babies. I cut a notch in one side of the pacifier's flange to make room for the endotracheal tube. The design allows for the tube and the pacifier to sit side by side in the baby's mouth — and I noticed a difference immediately. The babies were calmer and quieter, and appeared much more content, even in painful or stressful situations.
But I didn't want to rely on observations alone. So, I conducted a research study to see just how much these preemie pacifiers were helping.
At Winnie Palmer Hospital for Women & Babies at Orlando Health, I performed numerous routine heel sticks on 14 babies and recorded their reactions with and without the pacifier. The results were impressive.
Every baby who was given a modified pacifier during heel sticks had heart rates considerably lower than the babies who did not get the modified pacifier. And the oxygen-saturation levels of the babies with pacifiers were significantly higher. Those who got the modified pacifier also scored better on the Neonatal Infant Pain Scale (NIPS), which tracked crying, breathing patterns, facial expressions, limb movement and arousal. Simply put, the preemie pacifiers worked.
A new standard of care
I first started redesigning pacifiers for intubated babies as part of my master's thesis in the late 1980s and made the physiological effects of non-nutritive sucking the subject of my doctoral dissertation in 2009. It's been my passion to help these babies for decades, and today, I'm proud to say the modified pacifiers are the standard of care in many NICUs across the country.
But I think we can do more.
This month, I wrote a letter to the American Academy of Neonatal Nursing urging them to support my efforts to make these pacifiers more readily available. Hospitals have done a great job incorporating the pacifiers into NICUs, but the devices should also be available anywhere an infant might be intubated, including in emergency departments and in medical transport vehicles like ambulances and helicopters.
It’s rare that babies are intubated at home, but even in those cases, I would like parents to be made aware that the pacifiers are being manufactured and sold by a range of companies.
Medical emergencies that require intubation are scary and stressful for any patient, especially for babies and small children. It's time we consider what these children are going through during these frightening situations and take one simple step to give them the comfort they deserve.
If you agree, you can sign my online petition. Just go to http://myilluminateblog.com/pacifier/ and add your name to give these tiny patients a voice.
Follow all of the Expert Voices issues and debates — and become part of the discussion — on Facebook, Twitter and Google+. The views expressed are those of the author and do not necessarily reflect the views of the publisher. This version of the article was originally published on Live Science.