It's late June, a golden-blue day wrapped in soft, honeyed rustles hinting at untold promises and glories of the summer at hand. My small children are gliding into a friend's home, their goodbye kisses and laughter floating through tousles of hair. The sparkles fade to dust, swallowed by a mean swath of darkness. It dives fast from an unseen cloud that seems to hover only in my space, as my husband drives me to the hospital. The grimy mass fuddles my sight, blocks the sun, drenches my thoughts in dread and fear. It's a known entity, this cloud: a singular menace called the MRI breast biopsy.
Inside the hospital, the MRI prep-area smells of metal and medicine. Glassy air turns my fingers purple, and my jaw stiffens into a jittery semi-clinch. The nurse struggles with a faulty IV needle as bright-red streams spill from my left arm, sending my stomach into an unstoppable churn. My kind-faced radiologist peeks in and moves fast to help stanch the blood flow. I grab a bit of his calm and make it my own. The nurse wraps me in warm blankets and beckons a colleague. With ease, he slips a new needle into my unwounded arm.
With the nurse, the technician and the radiologist, I drift into the MRI lab. The nurse and the tech help me climb atop a narrow table, jacked up to give the radiologist access to me from below. We begin the sordid process of positioning my body. I lie on my stomach, facing the ground from an opening in a circular headrest. My torso shifts into a veritable vise, where it'll be hostage for an hour. Both of my breasts are smashed against waffle-like grids.
The table inches me into a hole that feels smaller than it looks. I'm at the center of a massive, doughnut-shaped spaceship: the MRI machine. I shift in and out several times, while the tech snaps pictures to help the radiologist gauge precisely where to insert the needles and perform the biopsies. It's a pivotal part. Without accurate images, the placement of a needle could be off, rendering inaccurate results. Inside, the maddening clatter of magnets is a welcome distraction from the searing screams of my crushed ribs. Never before have I wished for larger breasts. I do now. Better to torture fatty breast tissue than unforgiving bone.
Soon the radiologist plunges needles into my breasts at awkward angles, to numb them. The suspicious tissue in my left breast is burrowed deep, so he uses the maximum dose of the numbing agent. Scarier needles swoop in later, sounding like bike tire pumps. They suck out my tissue. My sternum seethes. My blood flows, and the radiologist warns the nurse.
I see nothing. I feel everything.
My arms, outstretched like Superman's, fall into a sea of pins and needles. Warm blankets still swaddle most of my body, but the icy claws of the lab press in hard. In minutes I'm pushing myself up from the table. The nurse and the radiologist clamp down on my breasts, driving back blood clots.
Soon I'm in a wheelchair, heading for the mammogram lab, to get more pictures of the torture I just endured. When the mammogram is done, a nurse bandages my upper body into an Ace corset and places tiny cold packs against each breast.
I realize I'd been riding an adrenaline wave. It breaks, leaving me awash in pain and hunger. I eat.
I go home to hugs and peals of joy: my babies.
I sleep.
When I'm awake again, I know. I'm not taking another lap around that monstrous circle of hell. Cancer or not, I'm finding a way out.
Grateful for Choices, Even When They're Tough
The biopsy I just described was two months ago. Showing benign results, the pathology report afforded me a brief dip in a shallow pool of relief. No cancer. This time. Maybe it'd creep up in the next six months. Maybe in a few years. I'm a high-risk candidate for developing breast cancer, something I learned last year, after a raft of MRIs, mammograms and biopsies revealed that my breasts were riddled with calcifications and cysts. Most of the activity was considered normal for a 40-year-old woman who'd recently stopped nursing. But cells in my lower-left breast showed two conditions considered markers for an increased risk of breast cancer: atypical ductal hyperplasia (ADH) and flat epithelial atypia (FEA). Both are characterized by abnormal cell growth.
My doctors suggested an excisional biopsy to remove the ADH and the FEA. I complied. My surgical oncologist removed all of the questionable tissue, submitted it for a full evaluation, and determined that nothing was cancerous.
In the midst of all of that, I met with a team of genetic counselors and the doctor who'd become my oncologist. They encouraged me to get a blood test for the breast-cancer genes BRCA1 and BRCA2. In addition to my mom, both my maternal grandmother and my maternal great grandmother had breast cancer, and both had mastectomies. My dad's mom died of ovarian cancer in her 70s. My genetics spell risk. Thankfully, the test showed that I'm not BRCA-positive.
These discoveries ushered in a new era. The atypical cells combined with my family history meant I was a high-risk candidate for developing breast cancer. The average woman faces a lifetime risk of about 12 percent; mine is about 43-48 percent, depending on the scale used. My oncologist has summed up my case this way: "If those were your odds of winning the lottery, would you play?"
When I learned these odds a year ago, my first reaction was to have a double mastectomy. It was the surest way to prevent my mom's history from repeating in my life. On the other hand, it seemed an unnecessary fix for something barely broken.
I resolved to put the mastectomy debate on the shelf for a while, and change as many aspects of my lifestyle as possible. I started seeing a doctor of applied kinesiology. He's done masterful work of balancing my hormones. I no longer eat grains, sugar or dairy. I've kept up regular workouts, and started using essential oils more often. The changes would hopefully amount to a clear breast MRI the next time around. If they didn't, I'd revisit the mastectomy idea.
When the MRI this past June showed suspicious findings, I instinctively began thinking that preventative surgery was the best path for me. After the MRI biopsy, I spent an hour with my oncologist, reviewing my options, and I talked with my surgical oncologist, who last year performed my excisional biopsy. They outlined my choices:
- surveillance every six months, in the form of MRIs, mammograms and biopsies as needed;
- surveillance plus Tamoxifen, a medication that can reduce breast-cancer risk; or
- preventative double mastectomy.
None of my doctors have pushed any of the options, particularly not mastectomy. They've emphasized that I need to do what's right for me. A big part of this involves my stress threshold and what will give me the greatest peace.
As I leaned in favor of option three, my doctors suggested my husband and I meet with a plastic surgeon, to learn more about the surgery and recovery. I also spoke with a woman who had a preventative double mastectomy, and I've done considerable research.
In the days leading up to a biopsy, my nerves could power a high rise. My thoughts go something like this: "If the results show cancer, what happens to my kids? If I do get cancer, and I need a mastectomy anyway, why not just do it now, when I'm healthy? Enduring these tests -- and possibly biopsies and excisional surgeries -- every six months will leave my mind worn like an old sponge, and my body pocked with scars."
I'm afraid of the unknown. I'm afraid chemotherapy would scorch my throat and turn my skin blue and green, as it did to my mom. I'm afraid to become her, to leave my children stranded, living the rest of their lives without half of their hearts.
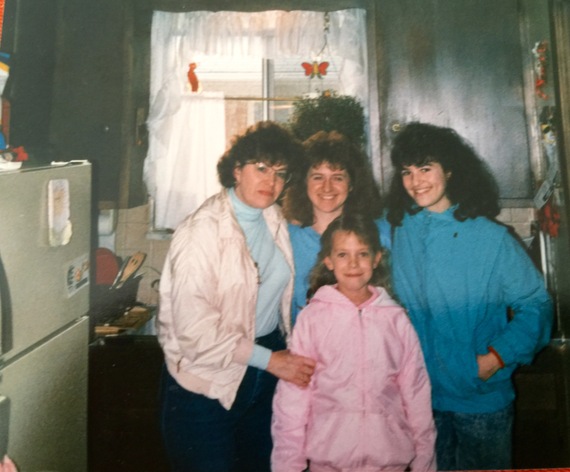
My mom, flanked by my sister-in-law, my cousin and me, far right, on the day we learned she had advanced breast cancer, in April 1988. She died in September 1989, at 46.
I must do the best, most responsible thing a mother can do. That means preserving my health, to the degree possible, and striving to get something right that my mom got wrong. She waited a year before she acted on a lump in her breast.
Looking at my kids, I cannot let that be their legacy. Whenever, however I die, I want them to know that their mom did everything she could to stay alive, that my main goal was to be healthy for them, in body and mind.
That's why I just scheduled my preventative double mastectomy.