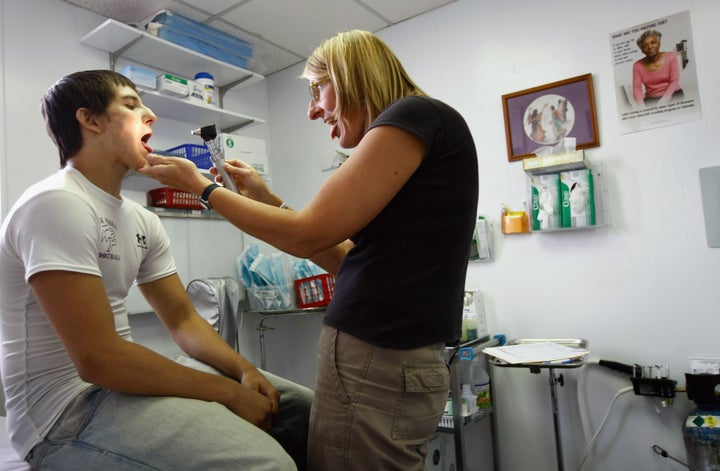
Patients living in areas with more primary care physicians have lower death rates and fewer preventable hospitalizations, new research suggests. But as the number of medical students pursuing internal medicine drops, a looming physician shortage could lead to a crisis in primary care.
"Simply put, medical students view internal medicine as working harder and getting paid less compared to other fields," said Dr. Mark D. Schwartz of NYU's Langone Medical Center, who has studied the phenomenon. "It's a very, very large concern."
To date, few studies have established concretely that more primary care physicians leads to better health outcomes. The new report, published Tuesday in the Journal of the American Medical Association, attempts to address that gap in research.
Researchers looked at local workforce populations and patient outcomes across a 20 percent national sample of Medicare beneficiaries over one year, taking pains to consider both the number of physicians who self-reported their speciality as primary care and the number of office-based, full-time equivalent practitioners (FTEs) per Medicare beneficiary. The differences in patient outcomes were pronounced.
Those living in areas with the highest quintile of primary care physicians per population had six percent lower rates of Ambulatory Care Sensitive Condition hospitalizations, or potentially preventable medical problems such as hypertension. Beneficiaries living in areas with the highest quintile of primary care FTEs had five percent lower mortality and nine percent fewer hospitalizations stemming from potentially preventable conditions.
Notably, differences in Medicare program spending were small. Chiang-Hua Chang, Ph.D., the study's lead author, said that could be due to patients in areas with high levels of primary care physicians simply being able to visit the doctor more often, leading to short-term spikes in clinicians' costs.
Overall, researchers concluded that a higher local workforce of primary care physicians results in positive benefits for populations. They also stressed that the benefits were more pronounced when specifically examining those practitioners who worked full-time in an office or clinic setting.
"Our study offers the cautionary note that having more physicians trained in primary care practicing in an area, by itself, does not ensure substantially lower mortality [or] fewer hospitalizations," they write. "The benefits of primary care workforce appear quite sensitive to the accurate discrimination of those physicians trained in primary care with those practicing ambulatory primary care."
The difference, Chang explained, is that many doctors work part time, devoting large portions of their working hours to teaching other clinicians or doing research. That results in fewer hours throughout the day during which they can actually see patients. And that issue could become more pronounced as fewer and fewer primary care physicians enter the field.
According to Schwartz, by the year 2016, the U.S. will experience a net loss of primary care physicians, as working primary physicians retire and fewer students take their place. Though other factors, like stress levels associated with primary care, could play a key part in dwindling doctors, he recently conducted research that suggests income disparities are at the heart of the matter. The estimated income gap between generalist and sub-specialist physicians is nearly $3.5 million over the course of a 40-year career.
But the study's authors say efforts to increase the number of students who enter the field comprises only half the battle.
"At present, medical student preferences are strongly directed toward subspecialties and family medicine programs are in decline, providing early warning signs of future serious shortages that could seriously impede health care reform efforts," they wrote. "[But] increasing the training capacity of family medicine and internal medicine may have disappointing patient benefits if the resulting physicians are primary care in name only."