Senate Republicans desperately want you to believe their health care bill is something it’s not.
They want you to believe that it protects the financially and medically vulnerable, that it won’t “pull the rug out” from people now depending on the Affordable Care Act for insurance, that ― as President Donald Trump has promised ― it will have “heart.”
Reality is different.
The Senate bill, which GOP leaders unveiled Thursday, looks an awful lot like the bill that the House passed in May. It would roll back the expansion of Medicaid that has allowed millions of people to get health insurance, then change Medicaid’s structure and reduce its funding going forward. It reduces the financial assistance available to Americans who buy coverage on their own and scales back guarantees of what insurance covers.
It would feel like an improvement to some people, for sure, particularly young, healthy people who would end up paying less for coverage than they do today, as well those who want less-comprehensive coverage or are angry about paying the individual mandate penalty. The wealthy Americans now paying taxes that finance Obamacare’s coverage expansion would get to keep that money. But the net effect would be more exposure to crippling medical bills for many millions of Americans.
It’s possible that Senate Majority Leader Mitch McConnell (R-Ky.) and his allies have deluded themselves into thinking this won’t happen. It’s more likely that they grasp the consequences and simply deem them worthwhile, for some combination of personal, political and philosophical reasons.
But they can’t come out and make that argument ― in part because, as polls indicate, the public almost surely disagrees. And so McConnell and his allies have written the Senate bill in a way that’s designed to obscure some of its harshest effects and give skittish members plausible-sounding reasons to vote yes.
Big Medicaid Cuts, But Pushed Into The Future
The House bill would change Medicaid in two main ways. It would end the Affordable Care Act’s Medicaid expansion, cutting off the extra federal matching funds that 31 states plus the District of Columbia used to expand eligibility. And then, going forward, the House bill would change Medicaid’s underlying funding formula, tying future federal contributions to an inflation rate likely to fall below what states would need to maintain existing levels of coverage.
Many senators objected loudly to these changes, usually because their states were among those that expanded coverage, or because their states rely on Medicaid to finance treatment of raging opioid epidemics or both. GOP leaders in the Senate purported to address these concerns by changing the timing of the expansion repeal ― specifically, by reducing the federal matching funds over three years rather than in just one year, as the House bill proposed to do.
But this change is a lot less significant than it sounds. The House bill also had a phase-in of sorts, because it had what amounted to a grandfather clause: It preserved the extra funding for people who had enrolled in the expansion for as long as they stayed on Medicaid. This would have effectively stretched out the transition over two or three years, as people in the program found jobs with enough pay to push their earnings out of the eligibility range.
More important, the Senate bill took the long-term cuts in the House bill and made them bigger, tying the federal matching formula to an even lower level of inflation. As a result, any gap between federal matching funds and what states need for Medicaid would grow over time ― most likely forcing them to make bigger cuts.
The more years that pass, the bigger the cuts would get ― which means, literally, that the worst damage would come after the 10-year window that the Congressional Budget Office uses for its projections of the bill’s effects.
Small Tax Credits But Distributed In A Progressive Way
The significance of the Senate bill’s changes to the private insurance market are similarly easy to miss, particularly when it comes to the financial assistance available to people buying coverage on their own.
The House bill would have wiped away completely the Affordable Care Act’s scheme of tax credits, which are bigger for people who have low incomes or face higher premiums ― in other words, the people who would struggle the most to pay for coverage on their own.
The Senate bill actually keeps that basic structure, more or less, adjusting tax credits based on income and insurance cost. In that respect, it resembles a version of “Obamacare lite,” as many commentators have noted.
But the word “lite” does a lot of work there. For one thing, the Senate bill is designed to buy a skimpier plan than the Affordable Care Act’s credit scheme does ― specifically, a plan that pays only 58 percent of the typical person’s medical expenses (roughly equivalent to a “bronze” plan in today’s system) rather than one that pays 70 percent of the typical person’s medical expenses (a “silver” plan in today’s system).
That translates roughly into a 15 percent, across-the-board reduction in subsidies, according to Larry Levitt, senior vice president at the Henry J. Kaiser Family Foundation.
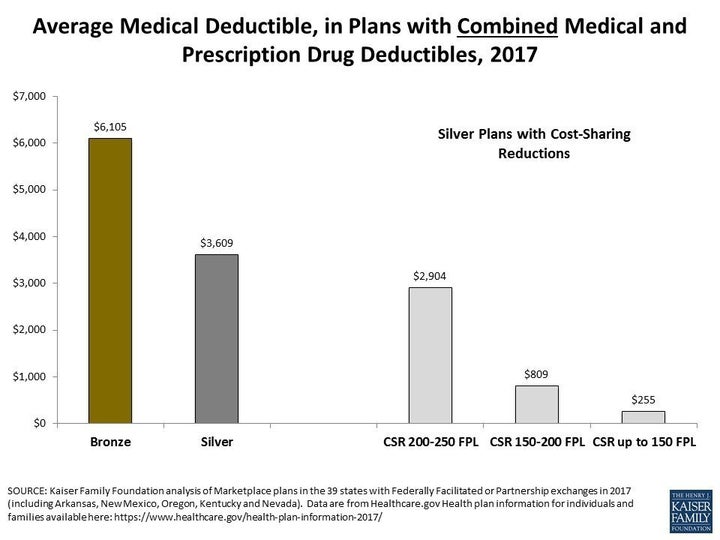
Lower-income consumers would lose even more money, because the Senate bill would not guarantee access to special, low-deductible plans that the Affordable Care Act makes available. The vast majority of people buying silver coverage through healthcare.gov or one of the state exchanges, like Covered California, enroll in one of these plans, which reduce total out-of-pocket spending to as little as a few hundred dollars in some cases.
It’s actually possible that the CBO will find the Senate bill leaves fewer people uninsured than the House bill did, just because of the way the different features would interact. And if that happens, Senate Republicans are sure to tout the CBO coverage number as proof they made the bill less severe.
But if the coverage number is higher, it would likely be because Senate Republicans have shuffled the pieces of their plan to distribute the impact a little differently ― disguising the damage rather than averting it.


