Bone is a living tissue and it responds to stress by making more bone. When the bone fails to respond adequately to stress, a fatigue fracture may occur (Figure 1). Stress fractures occur when the bone fails due to repetitive small stresses (microtrauma). Fracture can present itself early on as a minor injury with minor symptoms. If the fracture is not treated adequately it can become very disabling.
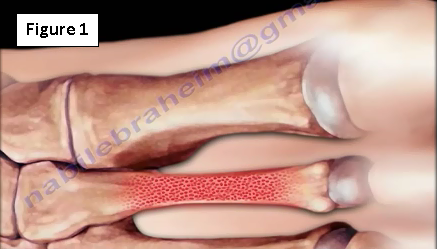
In athlete there may be localized pain that worsens with progressive activity such as increased training, increased running mileage, and a change in running surface or shoes (Figure 2). Early on, x-rays may be negative in the majority of patients. Bone scan is used frequently to detect early activity in the bone.

Usually the patient has vague symptoms. The patient may see different doctors in order to obtain different opinions, numerous tests will be performed. Female athletes who have decreased bone density and possible eating disorders will have an increased incidence of stress fractures. Female athletes with stress fractures should have a complete dietary and menstrual history. There is a correlation between eating disorders, amenorrhea and osteoporosis in female athletes (Figure 3).
In general, stress fractures may be treated conservatively. Sometimes stress fractures require surgery. There are four common areas for stress fractures in the foot; navicular, calcaneus, metatarsals, and the proximal fifth metatarsal.
Navicular
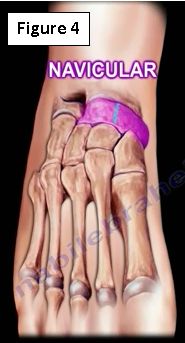
Stress fractures of the navicular bone are recognized with increased frequency especially in track and field, football and basketball athletes (Figure 4). It is more common in athletes with cavus foot. Pain from navicular stress fractures is poorly localized. Majority of navicular stress fractures are nondisplaced and occur due to chronic overuse. Symptoms include persistent, vague, diffuse midfoot pain that increases with activity and localized tenderness in the navicular area. These two symptoms draw the attention for the possibility of a navicular stress fracture. A delayed or misdiagnosis is common. The physician will need to rule out bipartite navicular.
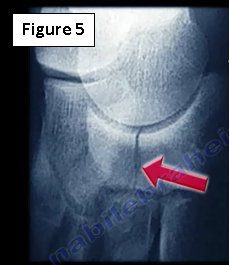
An x-ray is rarely helpful and is usually negative. An MRI or CT scan is usually obtained. The fracture occurs in the central 1/3 of the bone and it is usually vertical and incomplete (Figure 5). A bone scan is sensitive but high impact athletes may have multiple areas of increased uptake in the foot that decrease the value of the test. The diagnosis is usually delayed. If the clinical suspicion is high and the x-ray is negative, a bone scan or CT scan should be ordered. More recently, an MRI is used.
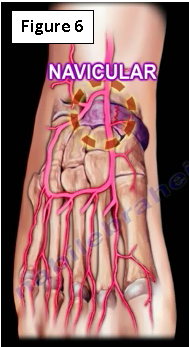
Vascularity of the Navicular Bone
The area where the fracture occurs is avascular (Figure 6). The center 1/3 of the navicular relatively avascular and has the greatest stresses. There is a risk of developing avascular necrosis, nonunion and delayed union when a stress fracture occurs in this area of the bone.
Treatment
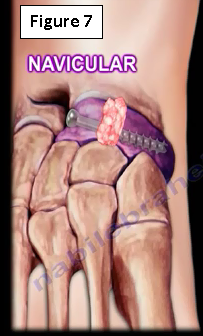
Treatment includes a short leg cast and non-weight bearing for 6-8 weeks. There is more success in healing of the fracture when the fracture is acute. Occasionally, the fracture requires internal fixation with or without a bone graft. If there is sclerosis of the stress fracture, surgery may be preferred. A small incision is made dorsally, to avoid disruption of the blood supply. The fracture is debrided and a local bone graft is used with a dorsal lag screw (Figure 7). In performing athletes, surgery is recommended to minimize the disability.
Calcaneus
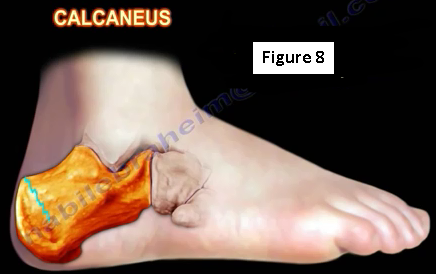
Stress fracture of the calcaneus is typically felt deep in the bone and produces a vague complaint of heel pain (Figure 8). These fractures are typically seen in athletes who are overtraining, using improper footwear or those with mechanical abnormalities. The pain from stress fracture appears suddenly and remains constant. Pain and swelling on both sides of the heel may be seen.
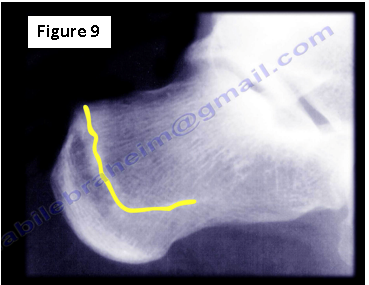
Imaging tests may be helpful to confirm diagnosis of a stress fracture. Stress fractures may be difficult to see on x-rays until the fracture begins to heal. X-rays at 4-6 weeks will show the fracture line on the posterior aspect of the calcaneus as a radiodense vertical line (Figure 9). The fracture is best shown on lateral x-ray. The pain associated with a calcaneal stress fracture can usually be reproduced by squeezing the heel from both sides. It is important not to confuse the pain of a calcaneal stress fracture with the pain associated with other conditions of the heel such as plantar fasciitis. The physician will need to rule out calcaneal stress fractures in heel pain. The pain from plantar fasciitis is most severe in the morning when the patient first stands on their feet.
Treatment
Treatment for a calcaneus stress fracture should begin with rest. The patient should avoid activities such as running and jumping. They should begin swimming to maintain conditioning and when tenderness is improved and subtalar motion returns, the patient can resume activity. Patients need to use proper footwear to cushion the heel (orthotics). They will be non-weight-bearing for 6-8 weeks.
Metatarsals
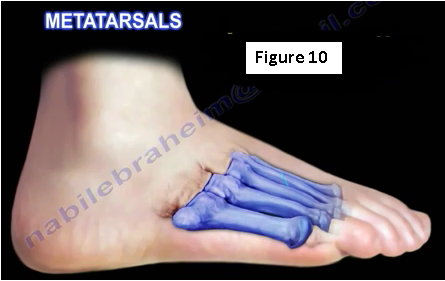
In runners, the fracture usually occurs in the metatarsal neck (Figure 10). In dancers, the fracture occurs in the base of the 2nd metatarsal. The fracture may result in delayed union. The patient will be non-weight-bearing for 6 weeks. The physician should look for anatomic causes of fracture in the 2nd and 3rd metatarsal neck such as heel cord tenderness, a short 1st metatarsal, or a long 2nd metatarsal. The physician will check for metabolic bone disease, osteoporosis or osteomalacia. During the examination the patient will have tenderness, induration, and a cavus foot. The bone scan is usually positive.
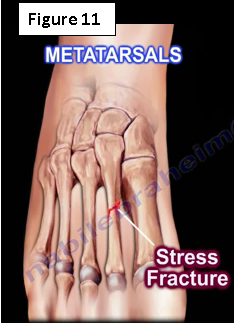
Metatarsal stress fractures occur due to the stress of weight bearing or prolonged walking (Figure 11). The fracture is sometimes called a “march” fracture that occurs in military recruits and in runners who increase their activity levels. It usually occurs in the 2nd metatarsal followed by the 3rd metatarsal. The fracture is diaphyseal in location and there will be localized tenderness at the fracture site. The 2nd metatarsal is the longest and most rigid of the metatarsal bones and it is usually exposed to greater repetitive stresses. The x-rays are usually normal and the patient may need a bone scan or MRI.
Treatment
Treatment includes the patient being placed in a walking boot and reducing activity level.
Proximal Fifth Metatarsal
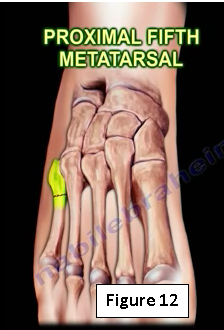
The fracture occurs in a watershed area of the blood supply that is susceptible to stress fracture nonunion (Figure 12). The blood supply in this area is tenuous. Healing is difficult with a high incidence of delayed and nonunion. The stress fracture occurs distal to the Jones fracture. The Jones fracture is an acute fracture and a stress fracture is a chronic condition that will require surgery.
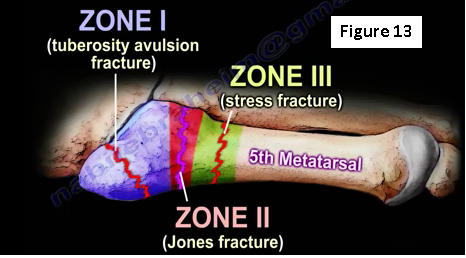
There are three types of fractures at the proximal fifth metatarsal: zone I (tuberosity avulsion fracture), zone II (Jones fracture) and zone III (stress fracture) (Figure 13). The stress fracture occurs distal to the ligament that connects the 4th and 5th metatarsal together. The stress fracture usually occurs in cavus foot due to increased ground reaction force over the 5th metatarsal. It will be overloaded on the lateral border of the foot. There will be dull pain activity related symptoms before the stress fracture shows up on x-ray. X-ray will show the fracture and its location. The x-ray will show varying degrees of sclerosis and widening of the fracture line.
Treatment
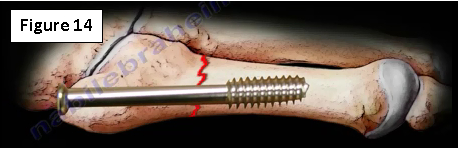
The treatment is usually conservative in avulsion fractures. Surgery is usually done for Jones fracture and stress fracture utilizing lag screw fixation with or without bone graft. (Figure 14).
For more information on stress fractures, follow the links below:
For more information, visit my YouTube Channel:
