Part 3
Following is the final story in a three-part series delving into the challenges, and potential hope, nonetheless, of living with sickle cell disease.
The fact that Tosin Ola-Wiessmann is still alive is no small feat.
A 36-year old wife and mother, she was born in Nigeria, where the more than 150,000 babies born there every year just like her, with sickle cell disease, give that country the world’s largest population of people with this genetic disorder. Sadly, only 5 percent of these children are said to live past the age of 10.
Periodically moving to the United States to pursue their higher education as Ola-Weissmann and her three younger sisters were growing up, her parents decided to settle in the states for good after doctors in Nigeria pronounced that she would likely die before her sixth birthday.
And, according to her, the medical care for sickle cell disease is indeed better in the U.S., where Ola-Weissmann says she can get much stronger pain medication — namely opium, morphine or Demerol — when she gets sick enough to go to the hospital. As opposed to the “fluids and Panadol, which is essentially like Motrin in an IV,” that she says she would get whenever her parents rushed her to the hospital in Nigeria with a sickle cell crisis.
In fact, cites Dr. Michael R. DeBaun, “many of the recent advances in sickle cell disease available in the U.S. to prevent early childhood deaths, strokes and pain have not been implemented in a systematic fashion in Africa or India.” Both regions where more than 90 percent of the world’s babies born with sickle cell disease are the black and brown newborns in these low- and middle-income parts of the globe. So adds DeBaun, director of the Vanderbilt-Meharry-Matthew Walker Center of Excellence in Sickle Cell Disease, in Nashville, Tenn.
But the paradox, contrasts Ola-Wiseman, is that “there is more discrimination in the U.S. healthcare system than in Africa.”
For patients with sickle cell disease, every single one of them has some horror story,” she asserts of being struck with a pain crisis — and black — when seeking medical help at an American emergency room.
“When you go into the ER, you are automatically seen as a drug seeker,” Ola-Weissman says. “Then you’re in the waiting room for anywhere up to eight hours because it’s not regarded as an emergency.”
“One time I was discharged and I couldn’t even walk,” Ola-Weissmann goes on to share. “My sister had dropped me off and gone to work. The janitor came and stripped the bed while I was in it. Then she helped me get dressed. No one offered me a wheelchair. I crawled to the waiting room and sat there until my sister could come back.”
At other times, Ola-Weissmann says, she has been released from one emergency room, only to immediately go to another one still feeling ill, and found to have an infection. And even been asked, “Why are you crying?” by nurses while in pain.

Tosin Ola-Weissmann.
To be fair, when it comes to sickle cell disease the medical community is up against a genetic malady that can manifest itself vastly different from person to person. Vastly different in terms of morbidity, frequency of crises, degree of associated anemia and impact on organ systems.
Even within one family. Like the eldest and youngest of Al and LaTasha Jordan’s three children, both of whom were born with sickle cell disease. A genetic outcome among this suburban Detroit household, their mother shares, that has only intensified the emotional, mental and spiritual rollercoaster that living with this disease can be.
Before it finally took the life of her 5-year-old son, Algernon III, on January 30, 2011, “his pain episodes were extremely bad,” says LaTasha Jordan, who, like her husband, wasn’t aware that she carried the sickle cell trait until they began to have children. In fact, she says, she didn’t even know what sickle cell disease was.
Jordan learned about it the hard way. She and her husband’s only son would have sickle cell crises that tormented him for days with excruciating back pain. Crises, in fact, that resulted in him being hospitalized three or four times a year. And — before the profound silence that, she says, woke her one Sunday morning to find him in bed with her and her husband from not feeling well the night before, dead — given the only thing that ever eased his pain. Morphine.
Algernon’s older sister, Lauren, now 13, doesn’t “have many painful crises,” Jordan contrasts. “But she’s more prone to developing pneumonia and acute chest syndrome. And she seems to catch every virus you can think of.”
Understandably, having two children with sickle cell disease was, Jordan admits, at times overwhelming, “especially the one time they ended up in the hospital at the same time.”

Lauren Jordan, her little sister, Katie, and late brother, Algernon III.
It was November of 2010, and pain crises landed both children at Beaumont Hospital in Royal Oak, Mich., for five days.
“My husband cared for my son on one side of the room, as I cared for my daughter on the other,” details Jordan, crediting both her Christian faith and the support of relatives and close friends for helping her family get through such an ordeal.
“Times like that are difficult because there's no sense of normalcy,” she shares. “My husband needed to go to work, outside [family] business needed to be done, and we had another child to care for. Even now, just dealing with one child having the disease, it can be very trying, expensive and frustrating during the hospital stays.”
Je’Lisa Glass, Tamea Harris and Palishia Turner are three young women who grew up in Detroit to find their lives interconnected by the sickle cell disease that afflicts all of them. Yet so uniquely as well.
“We all have sickle cell, but we are all completely different,” notes Glass, who, at 26, is a regular with her friends at the yearly awareness walk-a-thon hosted by the Michigan Chapter of the Sickle Cell Disease Association of America. She, Harris and Turner went on to describe just how different.
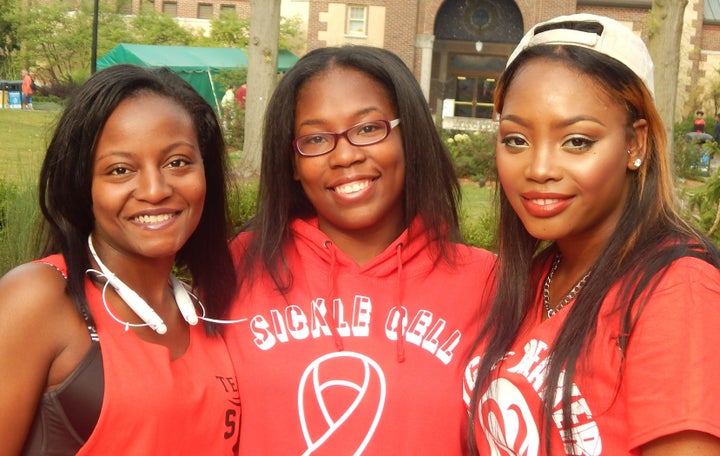
Palishia Turner, Tamea Harris and Je'Lisa Glass.
Like how Glass and Harris, friends since childhood, both have hemoglobin SS, the form of the disease also known as sickle cell anemia that is most common. And severe.
Glass says she finds herself having far more pain crises as an adult that send her to the hospital, sometimes for up to a week. This year, as often as twice a month, in fact, compared to the five or six times a year that she was hospitalized as a child.
“One minute I’m feeling better, and then the next moment I’m in pain and wondering why,” shares the aspiring professional make-up artist, who began a five-month program to become a certified cosmetologist back in February, but has yet to graduate. “That’s frustrating because I’m trying to finish school. I don’t let my sickle cell stop me, but I feel like I’m held back a lot because of it.”
At 28, Harris says she managed to avoid bad pain crises but spent “about 90 percent of my childhood” in and out of the hospital with “insanely high temperatures.” As an adult who now suffers from multiple other health challenges that include epilepsy and heart disease, her hemoglobin count defies doctors’ expectations of sickle cell patients in crisis.
The normal range of hemoglobin present in the red blood cells of healthy adult women is 12 to 16 grams per deciliter (100 milliliters) of whole blood. For patients with sickle cell disease, that number tends to be much lower: 8 gm/dL.
“For a normal sickle cell patient, when your hemoglobin is low you feel terrible and ultimately will end up in a crisis,” Harris notes. That’s certainly the case for her friend Glass, who says she gets dizzy, light-headed and even nauseous.
“However, for me the lower my hemoglobin the better,” says Harris. “Let’s say I go to the ER. My labs come back and my hemoglobin is a 10. Now that’s really good right?
“Not for me it isn't,” Harris continues. “That’s a clear indication that something is wrong. But because this doctor doesn't know me they send me home and hours or a few days later I'm back with even worse pain and a temperature now.”
“For me, my hemoglobin count tends to stay within [normal] range when in crisis,” Turner, 31, points out of her hemoglobin SC, a less aggressive form of sickle cell disease. “But my reticulocyte count is double, almost triple the normal range.”
A high level of these fledgling red blood cells produced by a person’s bone marrow — more than 1.5 percent of an adult’s overall red blood cell count — can mean they're overflowing into the blood stream much too soon, destroying mature red cells in the process. And, in turn, setting the stage for what's known as hemolytic anemia.
“Most people don’t know much about sickle cell disease, and what they do know is wrong.”
—Dr. Wanda Whitten-Shurney
This disparate pathology so characteristic of sickle cell disease has been just as confounding to those who practice medicine as to those they care for ever since the disorder was first identified in the U.S. more than a century ago.
“This is a very complicated disease,” Dr. Susumu Inoue, a pediatric hematologist/oncologist at the Hurley Medical Center in Flint, Mich., says of a genetic illness now costing more than $1.1 billion a year in patient care just in this country alone.
It’s not that scientists and doctors haven’t learned a great deal in recent decades about what causes sickle cell disease, how it affects the body and how to treat many of its complications.
Or that they don’t have an able comprehension of its multiple forms, from hemoglobin SS and SC, to the two variations of sickle beta thalassemia that obstruct a person’s hemoglobin production while also rendering that individual anemic. Plus a few additional rare forms of sickle cell disease.
Even so, “there are many things that we really don’t understand,” acknowledges Inoue. “One thing is that there doesn’t appear to be a straightforward correlation between the severity of pain and the lab values” of a person’s blood, reticulocyte and hemoglobin counts during a crisis.
“There is a truer correlation between the frequency of pain and lab values,” he adds. “But even that correlation is very poor. Sometimes people who have a milder form of sickle cell disease, come into the hospital every month. Sometimes people who are supposed to have a more severe form don’t go to the hospital much. We can’t figure out why that is the case.”
As for Glass, Harris and Turner, there’s no mystery to them about the one common denominator in their respective battles with sickle cell disease: the kind of treatment all three convey they’ve come to expect in the ER. Treatment that, to hear them tell it, mirrors what Ola-Weissmann has indicated can be a matter of course when winding up at the hospital black, and in crisis.
“They either don’t give you medicine, or give you too much to shut you up,” opines Harris.
Compare that with, “The kids in Africa manage their pain with Tylenol and water,” Glass shares of the reception her physical anguish has been met with.
Or, “You’re not as sick as our cancer patients,” adds Harris, who moved to Chesapeake, Va., at the end of March with the hopes that her health will fare better in that region of this country’s typically milder climate.
"Well, you're smiling so you can't be in too much pain," Turner says she once heard from an ER doctor when she managed to laugh at a joke told by a cousin who was with her. That was even though she had informed the doctor that, on a pain scale of zero to 10, with 10 being the worst pain imaginable, her pain level was at an eight.
“He was implying that I wasn't in as much pain as I had stated,” asserts Turner. “I shouldn't have to be stoic to be taken seriously. People with sickle cell have to be tough to go through the things that we have. I'm a strong believer in laughter being a form of medicine, especially if it can take your mind off your current state if only for a minute.”
All but just a few examples of the medical and social complexities that people with sickle cell disease grapple with over a lifetime, according to Dr. Wanda Whitten-Shurney. A 29-year pediatrician at the Sickle Cell Center in the Children’s Hospital of Michigan that comprises the Detroit Medical Center, Whitten-Shurney has known Harris, Glass and Turner since they were infants under her care.
“Most people don’t know much about sickle cell disease, and what they do know is wrong,” says Whitten-Shurney about “one of the most variable diseases on the face of the earth.” And that she, also chief executive and medical director for the SCDAA’s Michigan chapter, carries the trait for.
Throughout childhood, those with the actual disease face two major potential problems: missing a lot of school because of their health challenges, and the cognitive impairments that can develop from blood vessels getting blocked in their brain, Whitten-Shurney explains.
By adulthood, she continues, “you have a socially complicated patient” navigating yet another layer of challenges. From the stigma of being viewed as a drug seeker, to an overall mistrust of the medical community, to the toll that coping with years of arbitrary episodes of severe pain can exact. All of this is compounded by the fact that stress is a frequent trigger of sickle cell pain episodes.
Then there are the myths surrounding what it is to have sickle cell disease, Whitten-Shurney says. Like the notion that most people with it die by age 21.
In fact, at 86, Ernestine Diamond of Kansas City is believed to be the oldest American living with sickle cell disease. And Asiata Onikoyi-Laguda, a 90-year-old grandmother in Nigeria, is believed to be the oldest person in the world. Far more common, though, are those who survive into their 40s and 50s, divulges the National Heart, Lung and Blood Institute (NHLB).
Not the average life expectancy that extends into the 70s for the general population worldwide nowadays. But still a far cry from 40 years ago, when nearly 15 percent of children born with sickle cell disease died before the age of 2, and many more died in their teens, according to the NHLB.
ALONG COLOR LINES
Perhaps the most damning misconception about sickle cell disease Whitten-Shurney points out is that it is merely a black disease. Yet the genetic mutation that causes this life-threatening disorder actually evolved as a defense mechanism against malaria, which is prevalent in not only Africa, but the Middle East, southern Europe and South Asia as well. (All regions that are, now, or once were hot and humid, ideal conditions for the proliferation of malaria-carrying mosquitoes).
The spread of the mutated hemoglobin gene that causes sickle cell disease occurred “through population migrations to North and South America (especially the U.S. and Brazil) and the Caribbean as a result of the trans-Atlantic slave trade,” explains Dr. Isaac Odame, medical director of the Global Sickle Cell Disease Network.
“And to Europe mainly through economic migrations ” continued Odame, who is also a physician in the hematology/oncology division of The Hospital for Sick Children in Toronto. “The common link between peoples affected is that they have ancestry from areas of the world where malaria was or is endemic.”
That helps to explain how Giovanna Poli came to be the national poster child for the SCDAA from 2009 through 2011. Just 10 years old when she was first enlisted by the association to help publicize the reality that you don’t have to be black to have sickle cell disease, Poli, who lives in West Palm Beach, Fla., with her parents and brother, is of Italian descent.

Sophia Rose strikes a pose.
As is Lisa Rose; Greek and Italian descent, actually. Among her five biological and two adopted children with her husband of Irish descent, three of the biological ones carry the sickle cell trait like her. And while one of the biological children is both trait- and disease-free, the couple’s fourth child, 7-year-old Sophia, has sickle cell disease.
“Geneticists don’t even know what to do with us,” Rose shared right after another blood transfusion Sophia had just undergone at the Children’s Hospital Colorado.
“I found out that I had the trait, but I still didn’t know what it meant, when I was pregnant with my first biological daughter,” adds Rose, who now runs a nonprofit group to help disseminate better educational resources about sickle cell disease. Called Hope for SCD, Rose runs the group from the home in Raleigh, N.C., that she and her family recently relocated to.
“Because I was white, the doctor told me that the sickle cell trait didn’t matter and I could go on my merry way,” Rose continues. “They didn’t check my husband.”
In fact, he carries the trait for thalassemia, the related hemoglobin disorder that’s most common among those of Mediterranean ancestry. Combined with the sickle cell trait encoded within his wife’s DNA, that resulted in Sophia coming into the world with sickle beta-zero thalassemia.
Called into the doctor’s office two weeks after Sophia’s birth, “We were tested three times before they finally told us what was going on,” says Rose. And for the next three years, she shares, sickle cell disease “completely controlled our lives.”
“We were over protective,” Rose elaborates. “And Sophia wasn’t super sick at first. She had two blood infections, and they were serious, but that was over a period of four years. And she didn’t have pain.”
After Sophia had emergency surgery at age 4 to remove her spleen and gallbladder, “everything changed,” Rose continues. “She has been hospitalized for pain. She has asthma now. She has hypertension.”
Rose says her daughter, who somehow manages to remain “very stoic and very still” when in pain, has been doing better with monthly blood transfusions for the past year.
“Sophia’s illness is never pain free or without complications,” she points out, “but the transfusions lower her sickle cell percentages, which help with the frequency of her crises.”
Living with her daughter’s constant risk of infections, blockages and overall damage to her body has set Rose, as the white mother of a white child with sickle cell disease, on a full-time mission to better educate people about this genetic disorder that so many still know so little about.
“Our whole slogan is sickle cell is color blind,” Rose says, recalling the time Sophia had to go to the hospital in yet another crisis, and the doctor who ended up treating her announced, upon seeing her, “Well, you’re not black.
“And I said, ‘Well, you’re not either. Now can we get to the care of my daughter?’” says Rose. “It always seems to come back to race. We’ve had it taken off her chart when we come into the ER and she has a pain crisis.”
“Vitamin D deficiency is super common in people with sickle cell, but we were told we wouldn’t have to worry about that because she’s white,” Rose continues. “Well, her Vitamin D level got so low that she broke her femur once sliding out of a chair.
“It’s as if her blood is regarded as somehow different because her skin color is different,” adds Rose. And the kind of racial profiling that, she raises, could have dire consequences within the white community.
“All of the [white] people who carry the trait and are currently of baby-making ages have no idea they carry the trait,” Rose asserts.
“None of us were tested as children,” she goes on. “Yet testing along racial lines implies that [sickle cell disease] is restricted in some capacity and exclusively passed down through race, not genetics. Every person should be educated, tested and made aware of the possible outcomes with their partner regardless of race.”
Consider cystic fibrosis, another genetic disorder that, like sickle cell disease, can require strict daily drug regimens and frequent hospitalizations, get worse with age, and dramatically shorten life spans. Yet cystic fibrosis overwhelmingly plagues whites, a distinction that comes with a level of advocacy to battle this respiratory and digestive illness far outmatching that for sickle cell disease.
“Everybody’s heard of it, even if they don’t know what it is,” Rose cites of how effective the cystic fibrosis community has been in promoting their cause.
And even though cystic fibrosis only affects a third of the number of those with sickle cell disease, the National Institutes of Health (NIH) devotes 3.5 times more to the former in research funding. Private foundations provide about 400 times more in funding to the cause of cystic fibrosis than their less affluent sickle cell counterparts. And five new drugs were approved to treat cystic fibrosis between 2010 and 2013, versus none during that time for sickle cell disease.
“Because I was white, the doctor told me that the sickle cell trait didn’t matter and I could go on my merry way.”
—Lisa Rose
It’s against such contrasts that Rose embarks on projects like “Sickle What?” That’s her educational guide for parents of newborns diagnosed with sickle cell disease that Hilton Publishing released in April. Developed with Dr. Julie Kanter-Washko, director of sickle cell research at the Medical University of South Carolina, it’s an illustrated, spiral-bound booklet “written at a third-grade level with an adult background,” Rose details, to help lay the foundation of what it takes to understand and manage this genetic disorder.
Rose says “Sickle What?” echoes her actual reaction when first learning about sickle cell disease. Available online from Hilton and Amazon for community-based organizations and independent readers to pre-order, she discloses that it’s also being distributed among hospitals that she has relationships with.
“We are working on a larger scale nationally to gain ground with state newborn screening programs to provide either the hard copy or electronic version of the book to new families,” adds Rose. “Global Genes, a nonprofit rare-disease patient advocacy group, has supported this book with a grant to develop the E-book version to increase access to all families.”
In the meantime, Rose and her family continue to live out the irony of being among the minority in a community up against the prevailing regard for sickle cell disease as an unfortunate burden to bear as black folks. Such detachment only further highlights the history of racial bias in this country.
Even in the very discovery of sickle cell disease. Dr. James Herrick, a white physician out of Chicago, is given the credit for identifying this disorder in 1910. Yet it was his intern, a black physician named Dr. Ernest Edward Irons, who first called attention to the oddly shaped red cells he observed under a microscope in the blood sample of a dental student from Grenada. And who remains largely unknown for this find.
By the late 1960s, the only national nod to the treachery of sickle cell disease seemed to come with the U.S. military beginning to require black soldiers who even had the trait to wear special colored armbands. Or banning them from the service altogether. The singling out was prompted by the deaths of four Army recruits with the sickle cell trait during basic training exercises that were conducted at the Fort Bliss base in El Paso, Texas, between March 1968 and February 1969.
It wasn’t until 1972 when President Richard Nixon signed the Sickle Cell Anemia Control Act into law, with the goal of increasing funding the following year and expanding sickle cell disease-related activities at the Veterans Administration.
“Remember what life was like for black people in America in that time,” Gary A. Gibson says of the decades that passed before any tangible steps were taken from the seat of U.S. power to confront sickle cell disease.
“Here’s this disease that affects only black people,” the president and chief executive officer of the Martin Center Sickle Cell Initiative in Indianapolis maintains. “Who cares? It took 62 years for the American government to provide money for sickle cell research. And it was only $10 million.”
Even getting that took piggybacking on the fervor of both the civil and voting rights movements at the time to weave sickle cell disease into the national conversation on being black in America, says Gibson.
Founded by two now late black Indianapolis residents of renown — the Catholic monk and civil rights activist, Rev. Boniface Hardin, and orthopedic surgeon Dr. Raymond Pierce — the Martin Center emerged around then. Initially, as an advocate of social justice overall before becoming dedicated wholly to the plight of sickle cell sufferers.
The disease became such a part of the consciousness of that era, at least within the black community that it even emerged within popular culture. In “A Warm December,” the 1973 movie directed by and starring Sidney Poitier, Esther Anderson plays Catherine Oswandu, the African princess Poitier’s character falls in love with as a recently widowed American doctor vacationing in London with his young daughter. And whose sickle cell anemia tests the limits of how far their romance can go.
“It was great for Sidney to expose a disease whose sufferers were ashamed or afraid to come forward publicly,” says Anderson, whose performance in this drama earned her a NAACP Image Award for Best Actress. Unable to meet anyone who actually had the disease in time for production, she instead poured through medical books and files made available to her by friends in high places in Paris and her homeland of Jamaica to prepare for the role.
“Later on, I met people who came to visit me to see if I was still alive because they were sickle cell sufferers themselves,” Anderson shares of her portrayal.
Now 69, she still lives and works as a photographer and documentary filmmaker in London, where Anderson first moved to from Jamaica in 1961 to pursue acting and modeling.
“To a greater extent, we owed the advance of sickle cell screenings and treatment to the members of the African American community throughout the 20th century.”
—Esther Anderson
These days find the former promoter and girlfriend of Bob Marley busy in particular with screenings of the musical documentary, “Bob Marley: The Making of a Legend” that was compiled from footage she shot in the 1970s, and lost for 40 years.
But Anderson still finds time to continue the support she has given to various sickle cell causes since being in “A Warm December.” From a trip back to Jamaica after its U.S. release to organize a screening of the movie as a fundraiser that Michael Manley, the country’s prime minister at the time, and Dr. Kenneth McNeil, a prominent surgeon who was the minister of health, attended with their wives.
To visiting sickle cell patients as well at the Princess Mary Hospital in Nassau, Bahamas, a few years later. Plus helping to solicit additional funds and even facilities for the care and sustained pursuit of a cure for such patients. And guest appearing at sickle cell conferences and screenings of “A Warm December.” A movie that, according to Anderson, is shown somewhere around the world every year to raise money for sickle cell research.
“To a greater extent, we owed the advance of sickle cell screenings and treatment to the members of the African American community throughout the 20th century,” she says of sickle cell activism by and large. “The Civil Rights Movement was stirring people to stand up for their rights more, and sickle cell disease had already become a focus of attention among pioneering doctors like Charles Whitten and members of the Congressional Black Caucus.”
Fast forward to present times, with U.S. advocates still at the forefront of championing the sickle cell community.
Under the leadership of Whitten’s daughter, Dr. Wanda Whitten-Shurney, for instance, the SCDAA’s Michigan chapter is working to reverse the widespread unawareness of sickle cell disease through such undertakings as its annual summer walk-a-thon for the past three years. And to foster greater support for those directly affected by this illness through such programs as Project Enrich, an initiative pairing schoolchildren who have sickle cell disease with adult and teen tutors who have it as well.
Nationally, the SCDAA received a two-year, nearly $5.4 million federal grant to facilitate a broad, collaborative approach to serving the sickle cell community under the Sickle Cell Disease for Newborn Screening Program of the U.S. Health Resources and Services Administration.
Allied with 10 community organizations across the country like the Martin Center in Indianapolis, among the initiatives to come from this grant is Get Connected. This is a national patient-driven registry that the SCDAA launched this year to help link people with sickle cell disease and their families to education, counseling, health and other support services.
Joined by other groups such as the Centers for Disease Control and Prevention, American Society of Hematology, and American Public Health Association, the SCDAA is also pushing the National College Athletic Association to follow the Army in doing away with isolating measures for those under its jurisdiction who have the sickle cell trait.
Prompted by the deaths of dozens of student athletes with the trait over the past decade, the NCAA has required sickle cell testing for all its Division I athletes since 2010. But the NIH has been recommending that all babies born in the U.S. be tested for both the trait and disease, regardless of their race, since 1987 (though it took until 2006 for all 50 states to comply).
The NCAA’s mandatory screening as well has not only failed to prove to reduce training-related deaths among its athletes, Whitten-Shurney and other critics assess. It has put those who do have the trait at risk instead for stigmatization and discrimination.
“We had the same problem when my father was dealing with this in the military,” Whitten-Shurney recounts of the colored armbands for soldiers with the sickle cell trait. “I don’t want to see the same thing in sports. Athletes could lose scholarships, when the emphasis on determining who has the trait should be to help make child-bearing decisions and get counseling.”
Instead, the NCAA should implement a standardized program of safe training guidelines for all student athletes, says Whitten-Shurney. That would include gradually building up their exercise intensity, proactively helping them to avoid overheating and getting dehydrated during workouts, and educating coaches and trainers to better recognize and respond to athletes who report symptoms of physical distress.
Granted, Whitten-Shurney acknowledges the little-known reality even among African Americans that, in rare cases, sudden extreme exposure to such conditions as high altitudes, dehydration and physical exertion can indeed trigger sickle cell symptoms in people who merely carry the trait.
As has been the case in tragedies like Shanice Clark, a 21-year-old senior forward with the California University of Pennsylvania women’s basketball team who died in January 2015. And Dale Lloyd II, a 19-year-old freshman football player at Rice University whose death the day after collapsing during a conditioning workout prompted the 2008 lawsuit by his parents that led to the NCAA’s required sickle-cell trait testing.
For Ryan Clark, having the trait cost him his spleen and gall bladder. And nearly his career with the National Football League. The 36-year-old former tackling phenom’s health saga began with a 2007 game against the Denver Broncos that he played with the Pittsburgh Steelers.
Among the 3 million or so people in this country born with only one copy of the sickle cell gene and, thus, typically asymptomatic, Clark was taken to the hospital with an acute pain in his left side after the game. The mile-high elevation of the Broncos’ Sports Authority Field and exertion of playing safety for the Steelers had triggered a splenic infarction – meaning his spleen literally died – a common hazard among people with sickle cell disease.
As his physical well-being deteriorated, Clark’s spleen, then gall bladder was ultimately removed, ending that season for him. By the time he returned to play with his team again in 2008, he was 30 pounds lighter. And benched as a precautionary measure by Steelers head coach Mike Tomlin during any games played in Denver from then on.
“I think of those times when I had to train and would get dehydrated,” Clark, who learned that he carried the sickle cell trait while still playing football at Louisiana State University, recalls of his eventual near-death ordeal. “It was extremely hard. Now I understand why I probably got so sick.”
Yet the Bayou State native went on to play in two Super Bowls with the Steelers, winning the second match with his team against the Arizona Cardinals in 2009. He was also given an Ed Block Courage Award by his teammates, and named to play in the 2011 Pro Bowl before finally retiring last year.
“What I went through once, I went through for a month,” Clark reflected one afternoon from the Baton Rouge home he shares with his wife and three kids, the youngest of who, like him, has the sickle cell trait. “People with the disease go through this their whole lives. I could never have understood how difficult that is had I not gone through that.”
Or, perhaps, been as compelled as he was to launch his own personal offensive against sickle cell disease after his 27-year-old sister-in-law died from complications of this illness just two weeks after his Super Bowl victory.
“I want to find a cure for people who have this disease,” says Clark, who partnered with the University of Pittsburgh and its affiliated hospital to start the Ryan Clark's Cure League in 2012. The foundation has raised more than $2 million since, according to him, for continued research into sickle cell disease, patient-care support and endeavors to increase public awareness about this genetic disorder.
“We’ve made a lot of advances toward finding cures and developing medicines,” he says. “But we haven’t done anything concrete. I didn’t get into this to say, ‘Hey, we’re going to do a lot of nice work.’ My goal is to stop people from dying way too young.”
King is a writer, independent filmmaker and actress in Metro Detroit. A carrier of the sickle cell trait, she was inspired to write this special series by the loss of three sons, ages 5, 31 and 50, within two years in families she knows or knows of. Go here to access all of the stories in this series. To learn more about King, visit A Square Peg/Round Hole Creation, LLC.
