Since moving to Boston from Chicago for residency, the public health focus and awareness regarding the opioid epidemic has been staggering. In Chicago, focus was split on gun violence, infectious diseases, and chronic disease disparity. It is impossible to spend a day in New England without coming across a sign about Naloxone (Narcan) for overdose or a headline about the latest opioid taskforce.
New medical residents are required to undergo additional training in prescribing opioids. It is standard practice to check the online prescription monitoring program “MassPAT” prior to writing any prescription for controlled pain medication and to counsel patients on addiction resources. I have noticed the reticence of many providers to prescribe narcotics, even for patients for whom it would probably help in the immediate setting.

The latest hashtag campaign by the State of Massachusetts
The narrative surrounding the opioid epidemic begs the question of our country’s moral consistency regarding substance abuse and race. The current epidemic has predominantly harmed White communities. Ironically, African-Americans may have been spared the absolute worst of this epidemic because physicians have historically undertreated pain in African-American patients.
There is finally recognition, both within and outside of the medical community, that the criminalization of substance use is counterproductive. Law enforcement has been at the frontlines of utilizing Narcan to resuscitate victims of overdose. Diversion programs, such as LEAD, have become ubiquitous.
This empathy towards victims of substance use disorders is a relatively new phenomenon. Back in 2015, Eric Adams, a former undercover narcotics detective said, “the way I look at addiction now is completely different. I can’t tell you what changed inside of me, but these are people and they have a purpose in life, and we can’t as law enforcement look at them any other way.”
The reasons for the change are clear. One, the War on Drugs targets the African-American community. For decades, politicians and medical professionals have viewed and portrayed Black America as pathologically susceptible and morally at fault for drug addiction. For many, Danny from the Cape is a more relatable victim, and more deserving of empathy, than Deshaun from Chicago. Two, there is more sympathy because many victims of the opioid crisis are viewed as innocent. They became addicted or overdosed because they were initially introduced to the drug through legal, medical means. Anyone ever prescribed Vicodin after a root canal can relate to someone who is struggling with opiates after first getting them from their family doctor.
-
“For many, Danny from the Cape is a more relatable victim, and more deserving of empathy, than Deshaun from Chicago.”
-
If only politicians and health policy makers had demonstrated a fraction of the empathy towards to the African-American community in the 1980’s and 90’s as they do towards victims of the opioid epidemic today. An entire generation of incarcerated individuals and their families could have had vastly different life trajectories. The characterization of young, African-American men as super-predators, 100-1 sentencing disparities, and misguided “three strikes laws” have and continue to exacerbate health and socioeconomic disparities.
There is an emerging double standard evident in the Trump administration. Last October, within the same campaign speech, he supported addiction services for opioid use while denouncing President Obama’s efforts to shorten sentences for low-level drug offenders. There is a disturbing divergence where there is public empathy regarding the opioid crisis just as Attorney General Jeff Sessions threatens to rekindle disastrous, counterproductive, and disproven War on Drugs tactics.
The two tiered approach to drug epidemics is problematic. Awareness of fentanyl (a synthetic opioid) has significantly increased over the past year. Very early on the opioid epidemic, many non-pharmaceutical fentanyl deaths disproportionately impacted African-American and Hispanic-Americans. Yet, this was largely ignored by policymakers.
Today, African-Americans and Hispanic-Americans are less likely to enroll in or to complete addiction treatment programs. This is likely contributed to by socioeconomic disparity, but also due to the significant stigma and distrust of the medical system. Even in death, some minority families are less likely to be forthcoming about stating the cause of death as overdose due to cultural stigma.
Yes, the opioid epidemic has had its biggest mortality impact on White communities, but the harm of overdoses also decimate other communities. Rates of heroin death have been rising among all racial groups, including African-Americans, Hispanic-Americans, and Native-Americans. For example, according to the CDC, the rate of death among Native-Americans and Alaska Native people was almost twice that of the general population between 2007 and 2009. Beyond treatment programs, there is concern that access to Narcan, the life-saving overdose reversal drug, is limited in minority communities. Moreover, there is evidence that African-Americans and Hispanic-Americans are less likely to actually fill prescriptions for Narcan and to utilize it for reversal of overdose.
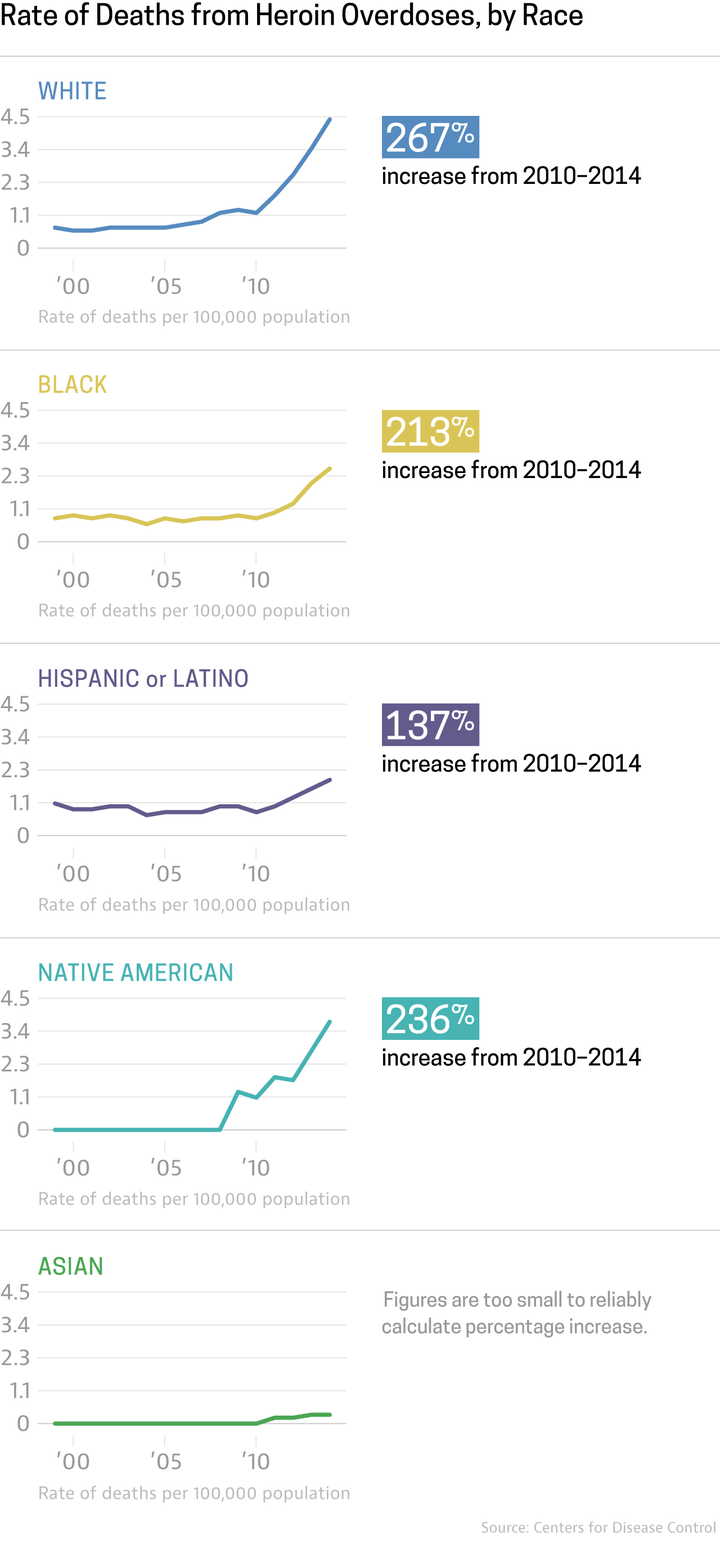
Minority groups have not escaped from Heroin deaths
The unavoidable racial dynamic of the opioid epidemic has helped to frame substance use as a public health issue. Billions of dollars have begun to flow towards harm-reduction efforts instead of incarceration. This is a much needed step for the United States.
Yet, policy initiatives, even with good intentions, that fail to specifically account for the impact on marginalized communities, have consistently led to disproportionate harm to the most vulnerable. We must remain vigilant in identifying ways that treatment programs, diversion initiatives, and allocation of funding can best help minority communities impacted by opioids and other drugs.
It is both fascinating and depressing that since the election of Donald Trump, the media has often focused on the plight of White America. Vann R. Newkirk II recently compared media coverage of the opioid epidemic to the “crack baby” fears of the late 1980’s, juxtaposing today’s warm empathy with the cold judgement of yesterday.
Study after study show that minority communities continue to face the brunt of healthcare disparities, substance use, and pending Medicaid cuts. Let’s not let the opioid epidemic become another example where minority lives are relegated to secondary status.
Akshar Rambachan, M.D., M.P.H. is a resident physician in internal medicine at Massachusetts General Hospital/Harvard Medical School. Follow him on Twitter @RambachanAkshar
