Nearly five decades after the first HIV cases were reported in the United States, an epidemic persists. Despite effective antiretroviral medications for both treatment and prevention, new cases continue to mount, with nearly 39,000 new HIV diagnoses in 2017 alone. But experts agree the country has the tools to finally end the epidemic at home by 2025.
“Our national HIV strategy to this point has actually not called for an end to the epidemic,” William McColl, vice president for policy and advocacy for AIDS United, told HuffPost.
That’s exactly what McColl and other public health advocates are doing. AIDS United spearheaded a report, along with more than 250 other organizations, outlining a plan for Congress to take “decisive action” to reduce HIV incidence and mortality. “Right now we have a historic opportunity” to put an end to the epidemic in the U.S., McColl said.
The roadmap for collective national response to the HIV epidemic, released Friday, on the eve of World AIDS Day, calls on Congress to enact legislation and allocate resources to achieve what the report calls a 95/95/95 framework for HIV care: ensuring that 95 percent of people living with HIV receive a diagnosis, 95 percent of people diagnosed with HIV receive treatment, and 95 percent of those in treatment become undetectable, or unable to pass on the virus, through antiretroviral therapy.
“If we’re able to implement this 95/95/95 cure framework with 40 percent PrEP coverage, we know that we can reduce the number of new HIV cases during the years 2019 to 2030 by nearly 353,000 people,” McColl said.
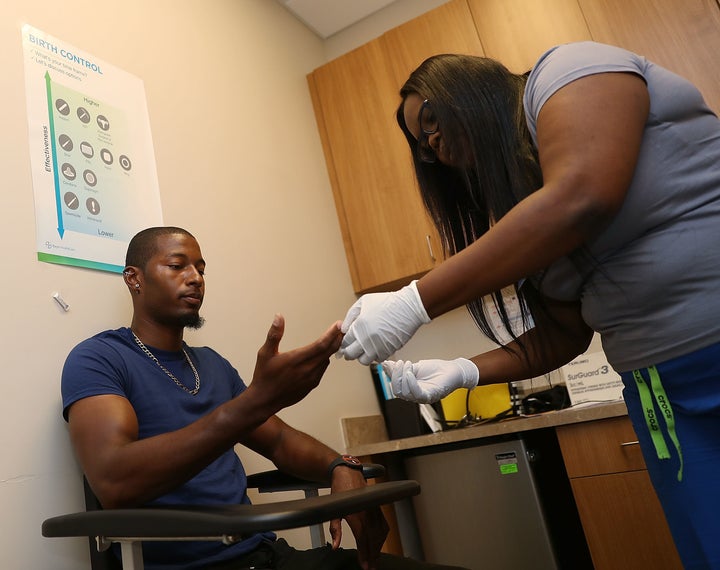
PrEP, or pre-exposure prophylaxis, is a once-daily oral pill that reduces a person’s risk of contracting HIV through sexual contact by more than 90 percent.
While experts and advocates are confident it can be done, they agree that one of the biggest challenges for the country will be addressing higher rates of HIV among communities of color, particularly LGBTQ communities of color, which are disproportionately impacted by the virus.
““[If] we don’t address the specific disparities for African American and Latinx populations, in particular, it’s going to be more difficult for us to end the epidemic any time soon.”
- Sable Nelson, a policy analyst for National Minority AIDS Council.
“If we don’t bridge those gaps and we don’t address the specific disparities for African American and Latinx populations, in particular, it’s going to be more difficult for us to end the epidemic any time soon,” Sable Nelson, a policy analyst for National Minority AIDS Council (NMAC), one of the organizations endorsing the report, told HuffPost.
Putting Marginalized Communities At The Center
“Social and economic marginalization leaves certain communities to bear the brunt of the U.S. epidemic,” the report’s authors said, adding that poverty, racism, sexism and homophobia also influence the likelihood of HIV exposure. Eliminating health disparities is a crucial part of the report’s six-pillar plan.
While nationally the number of new HIV diagnoses fell 18 percent between 2008 and 2014, some subgroups ― like queer Latinx men ― have actually seen a rise in that same time.
In 2017, black Americans made up 43 percent and Latinxs made up 26 percent of all new HIV diagnoses nationally ― with black queer men being most affected overall. Similarly, cisgender black and Latinx women are at higher risk of contracting HIV compared to their white counterparts.
Despite being at higher risk, black and Latinx are less likely than white Americans to use preventive measures like PrEP. A Centers for Disease Control and Prevention report released in March found that while half of the 1.1. million Americans who could benefit from PrEP were black, only 1 percent of people filling PrEP prescriptions were black Americans.
Disparities in housing, income and other structural factors among people of color also make it more difficult for these communities to receive the treatment needed to suppress the virus. And new HIV cases are increasingly concentrated in the suburban and rural South, a region with a high concentration of black Americans.
“Social and economic marginalization leaves certain communities to bear the brunt of the U.S. epidemic.”
- A new report on ending the HIV epidemic
“The challenge is getting drugs to people who need them ― whether it’s drugs for prevention or treatment ― and [the root of those] challenges range from resource issues to disparity and stigma issues,” McColl said.
To close these gaps, the report suggests ― among other policies ― expanding Medicaid and other federal health programs to ensure equitable access to effective HIV prevention and treatment.
But Nelson said it’s not enough to take a top-down approach; she insists the solution to the problem will come with both federal and grassroots efforts working collectively to reach vulnerable communities.
‘Meeting People On Their Terms’
Dr. Andrew Goodman, associate director of medicine at Callen-Lorde Community Health Center in New York City, an organization dedicated to serving the LGBTQ community, told HuffPost that the structural racism present in health care represents a major barrier to care for many people of color.
“Historically we’ve had a health care system that I think as much as it has wanted to help people, has probably traumatized people,” Goodman, an HIV specialist who was not part of the new report, said. And “part of our challenge is that we are one agency functioning in a health care system and culture that is just structurally racist and biased at its core.”
Stigma is also a big obstacle. “I know in spite of all the success that we’ve had with HIV treatment at this point in 2018, a lot of people still carry a lot of stigma and shame around with them around their own status or feel that from their community,” he adds. This keeps people from seeking testing, treatment and prevention options.
Breaking down these barriers, Goodman said, means being mindful about the physical locations of health services and creating outreach programs and interventions that are authentic and affirming.
For example, Callen-Lorde’s primary location is based in Chelsea, an LGBTQ-friendly Manhattan neighborhood that is overwhelmingly white. But in 2016, the nonprofit opened a location in the South Bronx, and it is planning another in Brooklyn to reach more communities of color.
And Goodman said the city’s Department of Health and Mental Hygiene has been instrumental in lowering HIV stigma by implementing sex-positive public health campaigns to normalize and raise awareness about PrEP among HIV-negative individuals. Several campaigns, including subway and bus ads, have been designed specifically to reach women of color and Latinxs.
On Thursday, the department announced that new HIV diagnoses in New York City had reached an all-time low for the second year in a row ― dropping 5.4 percent from 2016 to 2017.
Dr. Demetre Daskalakis, the department’s deputy commissioner for disease control, told HuffPost addressing health disparities among communities of color was crucial to achieving decreases in new HIV cases across all races.
“It’s a testament to the fact that being sex-positive, being person-focused and really trying to meet people on their terms changes an epidemic,” he said.
Nelson applauded New York City for their progress, particularly their work in breaking down stigma, but pointed out that many strategies that work for urban cities can’t always be successfully implemented in rural or suburban areas.
“No one should be dying from AIDS anymore. The science and the medicine is at a place where that does not have to happen.”
- Dr. Andrew Goodman, HIV specialist at Callen Lorde
“New York has incredible resources, they have incredible advocates...[and] it’s difficult to replicate what happens in New York in other states and other regions across the country,” she said. “It’s a completely different playing field in rural and southern areas, and you have to adapt your model for where you’re trying to provide those services.”
Nelson said stigma is compounded in rural and suburban areas, where people are afraid to be seen going to centers dedicated to HIV treatment. In these cases, National Minority AIDS Council has found that telehealth programs ― through which remote patients can connect with providers via video chat ― have been effective in engaging people in HIV care and retaining those with an HIV diagnosis in treatment.
Daskalakis agrees that the New York City model is not easily translated to those regions, but some lessons can certainly be applied to rural areas. This includes New York City’s move to introduce PrEP in sexual health clinics and combine HIV testing, treatment and prevention efforts ― so that individuals who test positive for HIV will be directed to treatment and those who test negative will be offered a prescription for PrEP.
“What we were seeing is that the very people that were accessing our clinics every day were the exact people that folks say are hard to reach,” he said. “So rather than recreating the wheel and trying to have them come to PrEP, we brought PrEP to them.”
For Goodman, it’s these interventions that cement his belief that ending the epidemic is not only achievable but well within reach with the appropriate resources and legislative support.
“In 2018, and this has been true for many years, no one should be dying from AIDS anymore,” he said. “The science and the medicine is at a place where that does not have to happen. So when it happens it is all because of these structures that we have in place that are failing people.”
