My dad passed away in March from lung cancer that had lain dormant for eight years after his initial diagnosis. The unstoppable force of his final illness was a painful blow for my entire family, but it hit me in a highly personal way to which I don't think anyone else in my family could relate. It didn't just steal the robust health my dad had been enjoying or the decades of life we began to come to expect for him. It was also a stinging reminder of cancer's power to reach well into the future and steal quality life from the clutches of the best laid plans... and not just in ways that we expect.
Many of us think of cancer as a parasite that grows and spreads until it "eats up" the body. But it doesn't always progress that way. Sometimes cancer's final assault arrives in a manner that seems fairly attenuated from the initial diagnosis. My dad went from pumping iron in the gym in January to having trouble swallowing in February. By the end of March he passed quietly in his sleep: Lung cancer cells had invaded the membrane surrounding his brain. This is rare, but not entirely unexpected in lung cancer. Also uncommon but still not unexpected is a new cancer (leukemia, for example) caused by long-ago cancer treatment.
But sometimes, the cause of death can appear almost completely disconnected from the origin diagnosis. One woman I know died in her 50s as a result of complications from a heart transplant, but the reason she needed the new heart was that her own had been damaged by treatments she received in her 20s for Hodgkin's Lymphoma. Or theoretically, one could die from a blood clot, caused directly by immobility as a result of a broken hip, where the broken hip may be traced back to osteoporosis brought on by chemotherapy -- from a cancer long ago put into remission.
In my own case, 11 years after my breast cancer diagnosis at age 36, people tell me that it is almost impossible to imagine me sick and fighting for my life. My own memory is selective; I have lost count of the sheer number of surgeries and days logged in the hospital over the past 11 years, all of them directly or indirectly attributable to the treatment I received for my breast cancer. But after the initial fog lifted after my father's death, I began to consider my own vulnerability to more and more complicated complications that might arise out of my initial diagnosis, my treatment and all of the surgeries and hospital stays that followed.
My mastectomy in 2002 was not optional, nor was chemotherapy and radiation. But the bilateral mastectomy was my choice, as was reconstruction. In 2003, the chemo left me depleted of white blood cells such that I had to spend a week in the hospital in "neutropenic isolation," taking an assortment of antibiotics. When I recovered, one of my implants ruptured, and I had to have surgery to replace it. That year, I also had my ovaries removed to keep me in the menopause that chemo had induced (enabling me to take an anti-cancer drug available only to women in menopause) and to prevent ovarian cancer in the future.
When my first reconstruction completely failed (due to the overgrowth of scar tissue), I had another reconstructive surgery in 2005. In 2010, my second reconstruction failed, presenting as a staph infection in a full-depth burn attributable to radiation damage. This led to a total of five more surgeries, including my third (and successful) reconstruction, as well as my being given an intravenous infusion of the antibiotic Clindamycin. The infusion of Clindamycin led to my developing a life-threatening and sometimes chronic intestinal complication caused by an overgrowth of a bacteria known as "C. Difficile."
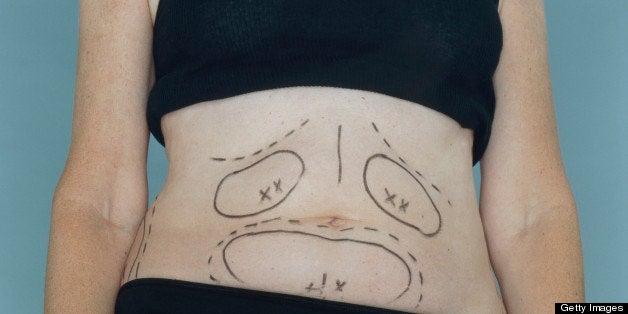
Optional but still related to my initial diagnosis were the plastic surgeries I had to help me cope with some of the aesthetically displeasing side effects of my treatment. In 2003, liposuction jumpstarted the loss of the 20 pounds of fat I gained while on chemo (a not uncommon side effect in young breast cancer patients). In 2005, my tummy tuck addressed the sagging skin on my abdomen after I lost the chemo weight (after menopause, the skin tends to sag). In 2007, at the age of 40, I had the bump on my nose shaved down because that same skin-sagging caused by the menopause was causing that bump -- which I had once thought of as "cute" -- to protrude in a decidedly "witchy" manner.
Far less obviously connected to my breast cancer -- but connected nevertheless -- was the allergic reaction I suffered this month after a week in the hospital for an infection that colonized a surgical incision I got as a result of the surgery that I had a week before that, which was a rather routine removal of my Fallopian tubes.
But how can I blame this on breast cancer? Please allow me to connect the dots:
In 2003, after the removal of my ovaries, I woke up in the recovery room to my surgeon bragging that she was so good that she managed to get at my ovaries without touching my tubes. Yay, I thought! I still have my tubes! Two years ago, my new OB/GYN thought I was kidding when I told her this (but really, is there such a thing as a joke about a fallopian tube?). Turns out that 20 percent of ovarian cancers begin in the tubes. I was not pleased at the prospect of having yet another surgery, but after taking some time to weigh the costs and benefits, I decided to go ahead and have my tubes removed via robotic-assisted laparoscopic surgery.
Waking up, my doctor told me that it was an easy surgery and everything looked healthy. I looked forward to an easy recovery. But it was miserable. I felt drained and foggy and unbearably swollen. Within three days, I noticed a doughnut-shaped hardness around my belly-button. On day four, I rushed to the emergency room when I realized that it was leaking some sort of murky fluid. I was terrified that it was my intestines coming out through my belly button, so I was relieved to learn that it was "merely" an infection.
Having caught the infection before it became systemic, I should have been able to leave the hospital within a few days, except that my blood cultures took longer than expected to reveal the responsible bacteria. I had to stay until the doctors knew what antibiotics would best target the bacteria. For the six days I was in the hospital, I was on three different antibiotics. When I left the hospital, I remained on those three. The morning after going home, I woke up scratching at some reddened skin on my abdomen. I was told to take two Benadryl. When I woke up again four hours later, the red skin had turned into dots, hives and welts that were spreading across my abdomen and reaching around my waist to my back. I could hardly stop scratching long enough to drive to the ER.
As I waited for my doctor to examine my rash, I was terrified that the verdict would be that I was now allergic to three new antibiotics (in addition to the two I had been allergic to since childhood), and that eventually, I would develop an allergy to every antibiotic and unable to fight even the most minor of infections. Therefore, I breathed a sigh of relief when my doctor took one look at the shape of the rash and told me that I was having a cumulative reaction to the adhesives in my wound dressings. And by "cumulative," she meant from all of the hospital-grade adhesives on all of the dressings that had ever been used on my skin -- and there had been a lot, particularly during all of my surgical and hospital adventures during 2010.
So, to review: First there was breast cancer that required surgery, reconstruction, chemo and radiation. Then there was neutropenia and an implant rupture. Then there was implant failure because of the radiation. Then there were surgeries and more surgeries, each one leading to surgical dressings that irritated my skin in a way my skin could never forget.
But wait, there's more.
It's entirely possible that this most recent post-surgical infection, which led to the placement of the adhesive-containing wound dressings that caused my allergic reaction, could have been avoided in the first place had I taken Clindamycin, which is routine in many operating rooms. However, remember I said that the last time I took Clindamyicin, I contracted C. Difficile? That meant no Clindamycin for me.
And there was still another wrinkle. My doctor explained that the tummy tuck -- which I underwent because my treatment-induced menopause had rendered my skin unable to bounce back after I gained and lost 20 pounds as a result of the chemo I took to treat my breast cancer -- compromised the blood flow to the skin around my belly button, which might have been a factor in allowing the bacteria to colonize in the incision there.
If you're confused, it's understandable. It's like "The House That Jack Built," except with reconstructed breasts, a flat tummy and a sculpted nose. I am: "The House My Rack Built." And it haunts me sometimes in my dreams.
Last night I dreamt of an Ingmar Bergman-inspired tennis game between me and a breast-cancer-shaped devil. We played as the years passed, and every time that beast hit the ball, I smacked it back... until eventually I was 105 years old. Although I felt amazingly spry for my advanced age, I failed to return a ball that landed near -- or on -- the line.
Next thing I know, I'm hurtling into space on a rocketship to Mars, and this same breast-cancer-shaped beast is whispering in my ear that soon we would crash -- it was time to kiss my life goodbye. I laughed in his face -- 70 years after my initial diagnosis, how could anything that happened now have anything to do with breast cancer?
The beast that was breast cancer laughed heartily and then stopped to look me straight in the eye as he deadpanned: "The only reason you're on this doomed flight is because you want the vaccine that will keep your breast cancer from ever coming back. And it's only available on Mars."
"That's completely out of bounds!" I screamed at him.
"Thanks for playing," he sneered.
"I demand an umpire!" I shot back.
"Happy trails," he smiled.
I closed my eyes as the turbulence picked up, and the floor seemed to shift under my feet.
When I opened them again? That's when I woke up.
So, yeah, maybe I've become a bit preoccupied with the long-term complications upon complications that come from surviving cancer at a relatively young age. But choice do I have but to keep smacking that ball?