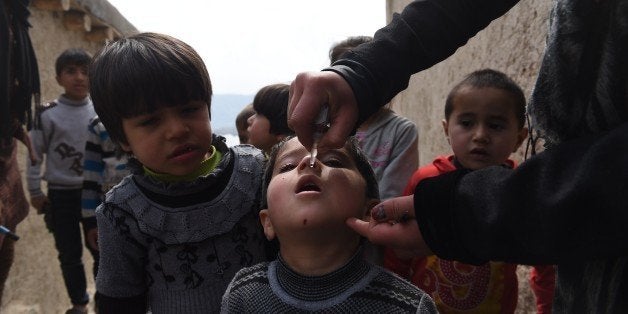
Polio, the contagious viral disease that can cause paralysis, breathing problems, even death, is no longer present in the United States. At its peak, polio was reported to occur in over 350,000 people every year around the world. By 2014 there were only 359 cases reported, according to the Center for Disease Control and Prevention. This was accomplished by a massive polio vaccination effort that continues today, using the two polio vaccines -- a live oral vaccine and a killed, injectable vaccine. By 2018, the World Health Organization hopes to have eradicated polio throughout the world.
But in 2000, an unexpected problem arose that could hamper that timeline. One of the two types of polio vaccines -- the live, oral version -- can actually cause paralysis itself, just like natural poliovirus. In rare instances -- about one in a million doses -- the live oral poliovirus vaccine, which has been altered to be harmless, can mutate and cause the same symptoms as natural polioviruses.
The dilemma for those who track polio around the world is that the oral polio vaccine is still very effective, although its mutated version can be spread into the environment through feces, infecting other people. Since 2000, the mutated viruses that come from the oral polio vaccine have caused 18 separate outbreaks of paralysis worldwide, mostly in populations where polio vaccination levels are low. Adding to this problem is the fact that intestinal infection with the oral polio vaccine produces no symptoms, so that spread of this virus and its mutated version is difficult to track.
Now that we are so close to eradicating all poliovirus infection from the face of the earth, the risk of spreading mutated oral vaccine polioviruses is very concerning. So concerning, that we and others around the world are conducting extensive research on how the oral polio vaccine strains are spread from person to person and into the environment. With a $3.6 million grant from the Bill and Melinda Gates Foundation, I am heading up a study as the Director of Stanford University School of Medicine's Global Child Health Program and with colleagues at the National Institute for Public Health in Mexico. In this study, we are investigating the rate and duration of person to person transmission and environmental spread of the live, oral polio vaccine in Mexican communities. The results of the study could affect public policy not only in Mexico, but all around the world.
Why are developed countries such as the United States so successful in eliminating polio infections? In part, this is due to the high vaccination levels in developed countries. Also, only the killed, injected form of the polio vaccine is used in developed countries, whereas most other countries rely on the oral version. This is because the oral vaccine is cheaper and doesn't require supplies of clean needles. Also, because it is a live vaccine, the oral version provides better intestinal immunity than the injected vaccine. Unfortunately, many areas of the world which still depend on the live, oral polio vaccine are places where the mutated oral vaccine virus is more likely to flourish and spread because open sewage and poor sanitation are commonplace.
In countries such as Pakistan, Afghanistan and Nigeria, which still use the oral polio vaccine and where natural polio infections still occur due to poverty, a lack of health services and misgivings about vaccination, the spread of the live, oral poliovirus vaccine could be an added source of poliovirus infections.
That is why it is imperative to explore how countries can start phasing out the oral, live virus vaccine in favor of using the injectable form of the vaccine, which is composed of a killed virus incapable of mutating.
The Gates Foundation grant is funding our two-and-a-half-year study, investigating the ability of oral polio virus to spread within households and cause community transmission. The country's current vaccination policy provides an ideal environment for studying this as well as the effect of the killed, injectable vaccine on the spread of the oral polio vaccine. Children there get both vaccines -- routine injections of the killed vaccine and twice-a-year doses of the live, oral vaccine. No other country in the world currently uses both the killed and live polio vaccines in this way. My team is trying to determine whether using the injectable killed vaccine could reduce subsequent doses of the live oral vaccine from being transmitted in households and into the environment. This information would be critical in understanding the best strategies to reduce and eventually eliminate all vaccination with the live, oral vaccine.
Ultimately, when all poliovirus infections are eradicated, the oral vaccine can be phased out worldwide. Understanding how well the injected vaccine works, and whether it is potent enough to prevent natural and vaccine poliovirus paralysis, will help us reach our goal of eradicating poliovirus paralysis around the world. We have already come a long way in reducing the total number of polio cases globally, and it is just a matter of time before polio is a disease of the past.