WASHINGTON -- Going without health insurance next year won't come cheap: The penalty for breaking Obamacare's individual mandate to get covered will get a lot higher.
It's the least popular aspect of Obamacare, and it might become even more disliked when the penalties increase. In 2016, those who don't have health coverage and don't qualify for one of the many exemptions from the mandate will owe the IRS anywhere from $695 to more than $2,000 -- a big jump up from the minimum penalty of $95 in 2014 and $325 this year. For higher-income families, the number could be even bigger.
The purpose of the individual mandate is to provide a disincentive for people to avoid cover if they can afford it. The requirement often is referred to as the law's "stick," the counterpart to the "carrot" of the subsidies available on the health insurance exchanges to make policies more affordable for low- and middle-income households. The Congressional Budget Office and other analysts predicted that the penalty rise would drive more people to sign up for health insurance.
The mandate is especially important as a means to nudge younger, healthier people who aren't heavy users of the health care system to get covered anyway. Their premium dollars go to cover the costs of those who need more medical care. This is vital to the long-term success of the health insurance exchange marketplaces and the insurers that sell on them. Finding the right balance on the exchanges has been a challenge and it is partly to blame for higher rate hikes this year.
Whether the mandate will boost sign-ups or wind up being little more than a nuisance is a subject of dispute. Millions of people went without coverage last year and paid the fine instead. Consumer research suggests a bigger fine won't change consumer behavior, no matter the expectations of Obamacare's drafters.
Carrie Banahan, executive director of the Office of the Kentucky Health Benefit Exchange, which operates Kynect, said that they believed more people would enroll because of the tax penalty.
“You really need to take a look to see if maybe buying coverage is going to be cheaper than the penalty”
- Carrie Banahan, executive director of Kynect
"We will have messaging around that in early 2016, just reminding individuals that the penalty increased," she said. "It might be significant for your household, you really need to take a look to see if maybe buying coverage is going to be cheaper than the penalty."
Yet President Barack Obama's administration expects modest enrollment growth, despite the higher penalty and the millions of remaining uninsured who could be using the exchanges, during the open enrollment period that started Nov. 15 and runs through Jan. 31.
That partly may be because a bigger mandate fine isn't a significant motivator for people without coverage who are more concerned about whether the insurance is affordable, said Jon Kingsdale, a director at Wakely Consulting who oversaw the implementation of Massachusetts' first-in-the-nation individual mandate in 2006 when he was head of the state's Health Insurance Connector Authority.
"I don't think that the calculus of going from three-something- to six-something-hundred dollars is the magic bullet that's going to convert a whole lot of uninsured to insured," Kingsdale said.
Survey results the Robert Wood Johnson Foundation published in June appear to support this argument: Just over one quarter of uninsured people said a bigger fine would make them more likely to get health insurance, compared to 42 percent who said it wouldn't make a difference.
The Obama administration and the state-run exchanges downplayed the mandate and the fine during the 2014 and 2015 sign-up periods, in part because they believe promoting the financial assistance to Affordable Care Act offers for health insurance is a more effective way to attract customers.
"We found that the affordability message really hits home with Idahoans, so that's the message that we're really driving this year," said Pat Kelly, executive director of Your Health Idaho, the Gem State's health insurance exchange.
The federal and state-run exchanges generally have employed that same strategy, but the emphasis may shift now the penalty is higher.
HealthCare.gov CEO Kevin Counihan published a blog post Monday urging consumers to consider the costs they would incur from the fine -- and from exposure to high medical expenses -- if they opted to be uninsured. "Your best option is to learn about the tax credits that are available and to visit HealthCare.gov to enroll in a plan that meets their needs, rather than taking the risk of going without insurance and paying a fee," he wrote.

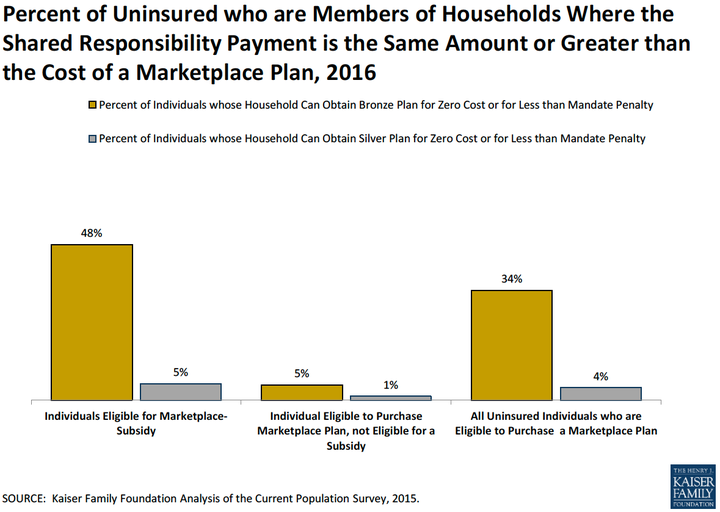
For about 65 percent of the nearly 11 million people estimated to be uninsured and eligible to use the exchanges, the mandate fine for next year would be less costly than the cheapest available health insurance plan, according to a Henry J. Kaiser Family Foundation report published Wednesday.
But that's heavily weighted toward people with higher incomes who choose to go without coverage and aren't eligible for financial assistance, the Kaiser Family Foundation reports.
Tax credit subsidies are available to people with incomes between the federal poverty level -- or about $12,000 for a single person -- and four times that amount. These subsidies are more generous for lower-income households.
About 7 million eligible uninsured people would qualify for tax credits, nearly half of whom could get a low-end "bronze" health insurance plan for less than the mandate fine, according to the report. Twenty-eight percent of that 7 million could sign up for bronze coverage at no cost because their incomes are low enough.
The individual mandate penalty for 2016 is calculated one of two ways: either a set dollar amount or a percentage of income, whichever is higher.
In the first case, a household would owe $695 for each adult plus $347.50 per child, up to $2,085. In the second case, the penalty is 2.5 percent of its income -- minus the first $10,000-$20,000, depending on age and family size -- up to the cost of the national average premium for the least-expensive bronze plan in a market, which the Tax Policy Center estimates is $2,676 for a single person, and would be higher for family plans.
The fine will be added to a household's tax bill, or deducted from its refund, when they file their income taxes for 2016, as the 2015 penalties will be next April.There is no fine for being uninsured up to three months in a year, and the penalty is assessed for each month beyond that a person doesn't get coverage. The Tax Policy Center provides a calculator that estimates how much a household would owe.
The average penalty for 2016 will be $969 per household, according to the Kaiser Family Foundation. The average amount owed by subsidy-eligible families will be $738. Those with incomes too high to qualify for tax credits will owe an average of $1,450.
For the 2014 tax year, when the minimum annual penalty was $95, 6.6 million people paid an average fine of $190, and 10.7 million people filed for an exemption, the National Taxpayer Advocate at the IRS reported in July.
The health insurance exchanges reopened around tax-filing time this year to accommodate people who owed the fine for 2014 and wanted to avoid it this year, but federal authorities won't do that this time, so consumers just have until the end of next month to make a decision.
"Where this could become really frustrating to folks is when they didn't understand that there was a fine, they didn't take action, and then come tax season, they've missed their chance to enroll," said Anne Filipic, president of Enroll America.
Also on HuffPost:

