Ticks transmit numerous viral, bacterial and protozoan pathogens that cause severe diseases in humans and animals, including Lyme disease.
Lyme disease is probably the most widely known tick-borne disease in the US. Ixodes, the genus of ticks that carry bacteria responsible for Lyme disease, have also been found in other parts of the world.
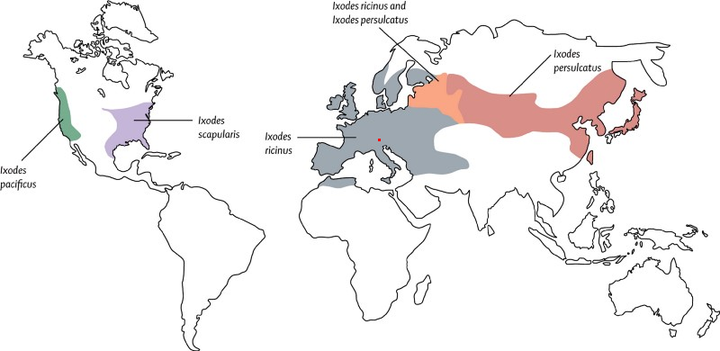
Global distribution of the vectors (Ixodes ricinus species complex) of Lyme borrelia (courtesy Stanek et al. The Lancet). The red dot indicates region where remains of the Iceman were found in the Alps
If you live in the northeastern United States, the very mention of ticks likely gets your neurons firing and you begin to recall pictures of bulls-eye rashes that are considered the hallmark of Lyme disease, and tragic stories that go with it. If you are a Connecticuter, then you have the dubious distinction of having Lyme disease named after a small town in your state. In the 1970s, several children and adults in and around Lyme, CT reported symptoms that appeared to be non-specific — swollen knees, skin rashes, headaches, general aches and pains, and severe chronic fatigue. Local physicians were unable to diagnose and treat the symptoms adequately. Frustrated, two women who were mothers of affected children finally went to the Connecticut State Department of Health, and the Yale School of Medicine to see if they could help their children. After systematic interviews and laboratory investigations, it became clear that a tick bite had precipitated these symptoms, and since there was an accretion of these symptoms in Lyme, CT, the disease came to be called Lyme disease.
Name and shame
It was not until 1982 that the bacteria that causes the disease was identifiedby Dr. Willy Burgdorfer and his colleagues — the bacteria were isolated from adult blacklegged deer ticks collected between September and October 1981, on Shelter Island, NY. In his honor, the bacteria are now called Borrelia burgdorferi.
With the expansion of the molecular biologist’s toolbox, in 2012 we learnt that Ötzi, the 5,300 year old Tyrolean iceman, had almost 60% of B. burgdorferi’s DNA associated with his remains. Irrespective of whether Ötzi was plagued by the symptoms of Lyme disease, it meant that the parasite identified by Dr. Burgdorfer was not a newly evolved species.
While Lyme disease has gained increasing notoriety, with it being one of the most rapidly expanding vector-borne diseases in the United States — more than 300,000 cases in 2015/2016 — ticks are also vectors for other diseases, some more severe than Lyme.
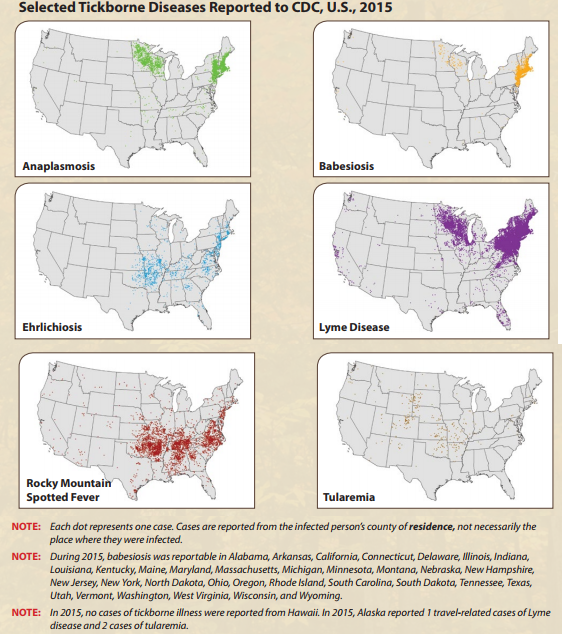
Life, size, and purpose of existence
The life cycle of the blacklegged (deer) tick is two years, and is made up of four stages — egg-larva-nymph-adult. White-footed mice are reservoirs for the bacteria that cause Lyme, and when the tick larvae (smaller than a pin head) and nymphs (size of a poppy seed) feed on infected mice, the bacteria enter the tick’s digestive tract. These infected ticks then find a human host, and during the process of feeding on the human host, they inject the nefarious bacteria acquired from the mouse, into the human.
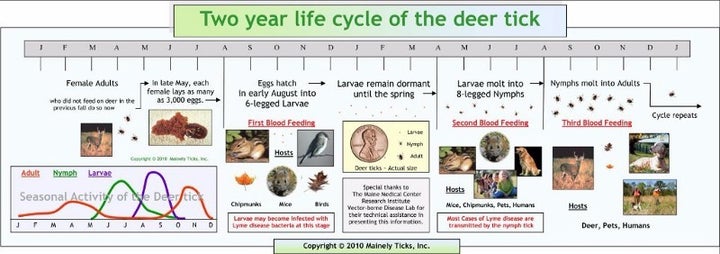
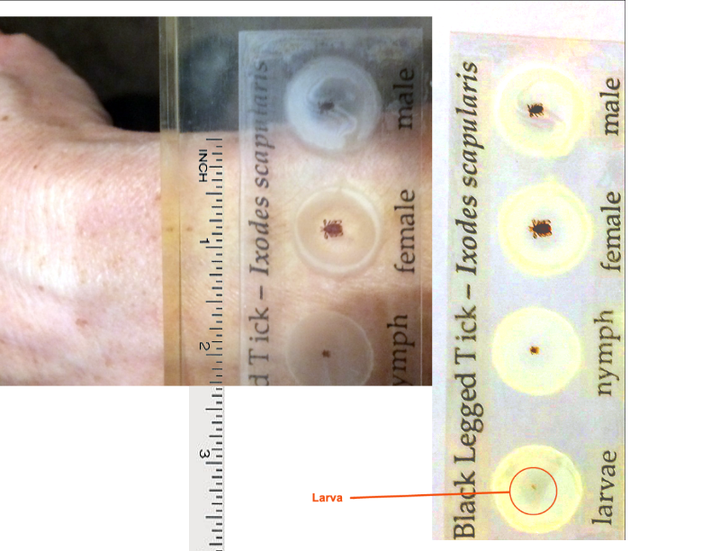
Right: Stages of tick life cycle. Left: nymph and adult female against an average human wrist.
The human host’s immune system then kicks into high gear and starts making antibodies to fight the bacterial infection. But these bacteria are not like the ones you’ve probably heard of, E.coli, Salmonella and their ilk, that can be treated by a quick dose of antibiotics. Antibiotics stop an infection by typically disrupting the multiplication of bacteria — the faster the rate at which a bacterium multiplies, the greater the number of opportunities for the antibiotic to kill it off. If the bacterium multiplies very slowly, stopping an infection takes longer. E. coli divide every 20 minutes, B. burgdorferi multiply every 24–48 hours! This explains why treating run of the mill bacterial infections requires an antibiotic regimen sometimes for only 3 days, whereas treating Lyme infections requires as many as 3 weeks.
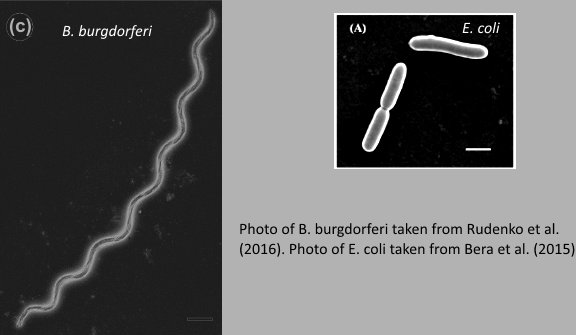
Comparison of the Lyme bacteria and more commonly known E. coli
Transmission and reduction
While all tick-borne diseases are transmitted only via ticks, there have been a few reports of transmission via blood transfusions. To eliminate this mode of transmission, the American Red Cross is working to develop tests to evaluate blood supplies for tick-borne parasites. Maternal-fetal transmission is less common, because in most instances administering antibiotics to an infected pregnant woman can kill the bacteria, if the disease is diagnosed in the early stages.
This year has seen a record number of ticks/tick bites reported to the Connecticut Agricultural Experiment Station (CAES). The larger number of tick bites is a consequence of a milder winter: mild winters mean more ticks survive and make it to the closest human; mild winters also mean that reservoir hosts are available in larger numbers for ticks to feed on — the population of white-toed mice and chipmunks has also increased this year.
Although it may not be possible to immediately address the issues of climate change that might result in milder winters, there are more immediate ways to reduce the possibility of falling prey to a tick-borne disease. CAES has a useful booklet that can be accessed online with five simple recommendations to prevent tick-borne diseases. The CDC also has a comprehensive resource with suggestions for reducing exposure to ticks. For example, those impressive walls you might have around your property, or even the pretty Japanese barberry you may have planted, are great venues for ticks and their smaller hosts to congregate! And of course, Bambi, the great tick host, might be endearing on screen, but in your yard Bambi is a Trojan deer, causing untold damage.
Prevention is better than cure; and definitely better than the bite!
