The percentage of Americans without health insurance has fallen again, according to a government study released early Thursday.
But whether that progress continues will depends greatly on what happens in Congress in the next few weeks.
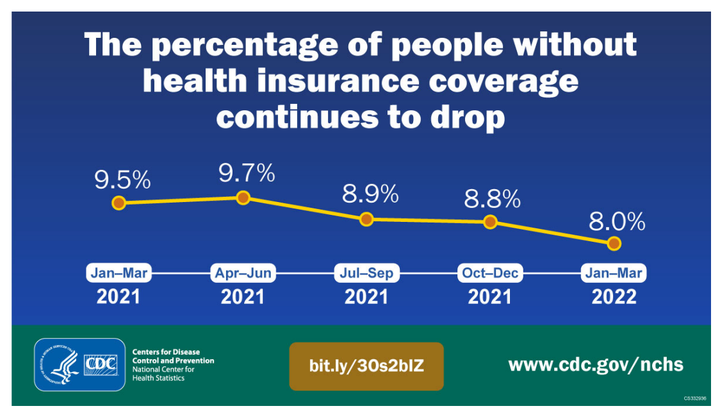
The study was a long-planned, regular update to the National Health Insurance Survey, one of several tools that government and independent researchers use to assess health coverage in America. The study found that the percentage of Americans without health insurance has declined by 1.5 percentage points in the past year, from 9.5% in the first quarter of 2021 to 8% in the first quarter of 2022.
That’s a pretty big drop, and it may have brought the level of “uninsurance” in the U.S. to a new, historic low. It’s hard to be certain, because the NHIS is not that precise and because the government modified the questionnaire in 2019, making direct comparisons to previous years difficult.
But there’s little dispute among experts that the percentage of Americans without health insurance has come quite down a lot ― first with the rollout of the Affordable Care Act in 2014 and, more recently, with the enactment of some temporary, pandemic-related measures to expand the law’s reach while shoring up other federal health programs.
The best-known of these recent measures was a boost in the financial assistance available to people buying insurance on their own, through HealthCare.gov or state-managed online marketplaces like “Your Health Idaho” and “New York State of Health.”
The new assistance has made it cheaper to buy coverage through these official government-run markets ― lowering costs by hundreds or even thousands of dollars a year. But the funding was part of the COVID-19 relief bill that Democrats passed and President Joe Biden signed in early 2021. It’s set to run out at the end of this calendar year.
Another, less-publicized recent measure was a rule prohibiting states from requiring people on Medicaid to reestablish their eligibility for the duration of the pandemic, on the theory that people who qualify for the program frequently lose their coverage anyway because they can’t manage the notoriously cumbersome verification process.
That prohibition will end whenever the Biden administration declares an official end to the COVID-19 public health emergency.
If the two temporary measures end, the number of people without health insurance is likely to go back up, while many others would remain insured but face higher prices.
“The progress in health insurance coverage could all come crashing down,” Larry Levitt, executive vice president for health policy at the Henry J. Kaiser Family Foundation, told HuffPost.
“These two pandemic-era provisions have measurably reduced the number of uninsured since their enactment, and will send the number higher again if and when they expire,” said Sara Collins, a senior scholar and vice president at the Commonwealth Fund, a New York-based foundation that focuses on health care.
Biden and Democratic leaders have been working feverishly to keep that from happening. And their best hope right now is what’s left of the legislation that started out as their Build Back Better plan.
Biden and Democratic leaders had to drop many of the bill’s key elements, including its child care provisions, because their legislative majorities are razor-thin. Republicans want nothing to do with the agenda, and a small number of Democrats had objections ― chief among them Sen. Joe Manchin (W.Va.).
“The progress in health insurance coverage could all come crashing down.”
- Larry Levitt, Henry J. Kaiser Family Foundation
But Manchin on Wednesday announced that he’d come to an agreement with Democratic leaders over a narrower bill with climate and health care policies, including a three-year extension of those Affordable Care Act subsidies.
That same bill could also include provisions to make sure states don’t cull their Medicaid rolls too hastily or clumsily after the public health emergency. Several Democrats have called for such measures, although it’s not clear whether that aspect has the support it needs to pass.
“During the course of the pandemic, we know that many people moved due to financial or other circumstances, so it will be challenging to reach many people once they need to have their eligibility redetermined,” Linda Blumberg, institute fellow at the Urban Institute, a Washington-based think tank, told HuffPost.
“A big fear is that people who remain eligible for Medicaid will not be aware, once the [public health emergency] ends, that they need to re-verify their eligibility and that they will lose their coverage for administrative (data) reasons, not because they are no longer eligible,” Blumberg added.
It remains to be seen whether the legislation will come together and pass.
The proposal has already drawn opposition from conservatives and Republicans, who object to the substantial new spending it would require and, more generally, to the support for a greater federal role in health care. They may have stopped crusading to repeal “Obamacare,” but they’re not about to take action that would support it.
That means, as usual, Democrats have only a handful of votes to spare in the House and zero in the upper chamber, creating huge challenges for Senate Majority Leader Chuck Schumer (D-N.Y.) and his team. But if Democrats needed extra incentive to push this bill through, the new study ought to provide it ― by demonstrating how many people have benefited from their temporary programs, and how many will lose out if those programs don’t keep going.
