This is the second of a three-part series on how sleep apnea affects behavior and learning in children. Part I of this article addressed the signs and symptoms of sleep apnea in children. This portion addresses the origin and factors that can lead to sleep disorders and the next, are possible treatment plans to consider.
The origin and factors that contribute to sleep apnea are varied and the onset of symptoms can be as early as birth. Since the Temporomandibular Joint (TMJ), Cervical Spine, and the Autonomic Nervous System (ANS) are interrelated, a dysfunction can contribute to sleep apnea or Temporomandibular Dysfunction (TMD). Dysautonomia, which is a dysfunction of the Autonomic Nervous System (ANS) can include accidental injury. A child passing through the birth canal can have spinal misalignment, especially if complications or assisted vaginal delivery was required, such as forceps or vacuum extractor, and unusual delivery or maneuvers to rotate a breech baby . The ANS is responsible for the body’s automatic functions breathing, heart rate, blood flow, digestion, etc. The nerves that travel through the vertebrae of the cervical spine serve all of the body’s organs, so any dysregulation may result in serious illness or disability. This can happen slowly over time such that an individual will adapt to the discomfort until it becomes too painful or disabling to ignore. One of the most common causes of spinal misalignment problems is poor posture e.g. sleeping, working, sitting, or standing. Without relief, symptoms can lead to long-term exhaustion, fatigue and sleep disorders. Dysautonomia cases are unique and require individualized treatment.
TMJ disorders involve the muscles that move the jaw or can involve the jaw joints as well. Many people clench and grind their teeth, but those experiencing severe stress, airway problems, and those in chronic pain will clench and grind their teeth more than normal. Two major causes of TMJ dysfunction are extensive clenching or grinding of teeth and whiplash injuries. Whiplash accidents that can injure the neck can also injure the jaw muscles and joints.
The muscle-dura connection may transmit forces from the neck muscles to the pain sensitive dura. Traction on the dura overlying the autonomic nucleus results in many of the symptoms of craniofacial, myogenic, and cervicogenic pain. Cervicogenic pain is usually the result of trauma to the neck and can include motor vehicle accidents, childhood falls without obvious injury, and sports-related trauma.
Other common factors that increase the risk of sleep apnea:
- Problems with muscle tone: Children can have trouble breathing during sleep because the throat muscles relax and block the airway. This can happen in any child, but especially in conditions such as Muscular Dystrophy and Cerebral Palsy.
- Genetic syndromes: Children with genetic diseases such as Down syndrome and Prader-Willi
- Abnormal Face or Throat: Children who have an abnormal shape to their face or throat
- Additional thickened tissue or excessive fat stores surrounding the airway.
- Supine (flat on back) sleeping
- Obesity Excess weight – the risk for sleep apnea is higher if overweight with a body mass index (BMI) of 25 or more or obese with a BMI of 30 or higher.
- Chronic sinusitis
- Large neck circumference risk for sleep apnea is higher. A large neck has more soft tissue that can block your airway during sleep.
- Large tonsils or adenoids
- Recessed chin or large overbite
- Family history of sleep apnea

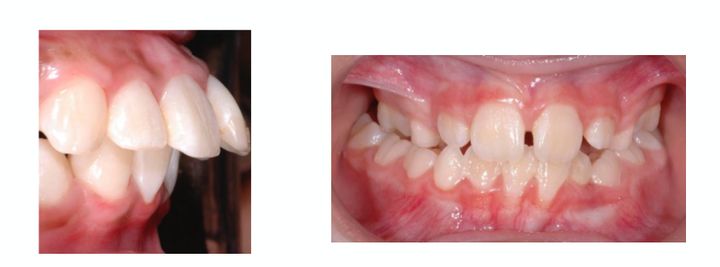
Jaw abnormalities found in children: mandibular retrognathia, enlarged over-jet, lateral crossbite
Below are some signs of sleep apnea that children may experience:
- Mouth breathing
- Dark circles underneath the eyes
- Chronic congestion
- Overweight or obese
- Snoring
- Enuresis
- Hyperactivity (ADHD)
- Developmental delay
- Poor concentration
- Nightmares
- Night terrors
- Headaches
- Restless sleep
- Large tonsils
- Noisy breathers
- Chronic runny noses
- Frequent upper airway infections
- Earaches
- Bruxism
If your child has any symptoms of sleep apnea, see your family physician or otolaryngologist (ear, nose and throat doctor) so testing such as a sleep test can be conducted. A sleep study or polysomnography (PSG) monitors breathing, brain waves, oxygen levels in the blood, muscle tension, and eye movement. The test is painless and although home sleep tests are available and highly accurate, for children the sleep test is still generally performed in a sleep laboratory or hospital.
Co-authored with Lily Mai
