
By Lee Romney
ANCHORAGE, Alaska – Tina Cramer Showers keeps one vomit bucket on the narrow stairway of her Anchorage townhouse, another at her bedside. It was there, during a grueling course of cancer treatment last year, that the Air Force veteran settled in for marathon phone sessions with “Health Choice.”
That’s what Cramer Showers calls Veterans Choice, Congress’ hastily crafted response to the scandal of veterans dying while awaiting appointments at Veterans Affairs medical facilities. The goal: to farm out veterans to private care providers when VA waits are too long or travel distances too great.
Sole-sourced to two private companies to administer, the program has been criticized nationwide for not living up to its promise. Many veterans call it “No Choice” or “Bad Choice.”
In Alaska, an investigation by Reveal from The Center for Investigative Reporting found it took a hard-won system with identical goals that was working better and made it worse. Far worse.
Under the Choice program, seeing private medical providers through the VA got a lot more complicated in Alaska. The VA’s own nationwide analysis says the program is costing taxpayers more money. And the volume of care in Alaska declined – the opposite of what Congress intended.
Cramer Showers was diagnosed in 1999 with amyloidosis, a rare and often fatal disease, outliving by a long shot her doctors’ expectations. She had survived an earlier bout with cancer and once drove herself to the hospital while having a stroke. She brought her push-through-it attitude to navigating her latest health challenge.
But the rules of the game at the VA had changed dramatically.
Before showing up for a chemotherapy regimen she hoped would keep her stage 4 lymphoma in check, she had to ensure the visits had been approved and a paper confirmation faxed to her doctor. Otherwise, she could get stuck with the bill.
“One person at Health Choice would tell you yes, and one person would tell you no,” Cramer Showers, 54, said of hours of monthly conversations with call center workers from TriWest Healthcare Alliance, which carries Alaska in its portfolio of states.
“I’d be puking and still trying to communicate,” she said, “because I knew, ‘I gotta have this thing.’ ”
Cramer Showers had seen the very same oncologist before the rollout of Veterans Choice. And it was a near-seamless experience. This time was different: long calls to strangers in distant cities, lost authorizations that prompted her to skip a course of treatment, bungled bills that threatened to leave her on the hook for thousands of dollars in out-of-pocket costs.

Alaska has no full-service VA hospital, so veterans for years had to travel to Seattle or farther afield for treatment at VA facilities. Fierce advocacy by the state’s congressional delegation changed that. In 2010, Alaska’s VA Healthcare System began sending veterans out “on the economy” for a growing menu of treatments.
The initiative pushed Alaska into the top tier of VA systems nationwide that were leaning on the private sector to care for ailing and injured veterans. It even made Alaska a model of sorts, a precursor to Veterans Choice.
So when President Barack Obama signed the $10 billion Veterans Choice program into law in August 2014, Alaskans watched from the sidelines. Plenty of veterans tossed their Choice Cards in the trash. The plastic cards were sent to millions of veterans across the country who might be eligible for the program, but they guaranteed no care. Instead, they instructed veterans to call a number for more information.
Most seemed to pay little attention until national officials directed all VA medical centers to use Choice funds first before turning to other means of buying outside medical care.
As complaints about the program flooded in from across the U.S. in fall 2015, Dr. Baligh Yehia – a young Princeton-educated VA physician – was tapped to overhaul the agency’s approach to buying private care.
Long wait times, unexpected bills, appointments with the wrong doctors – all were common themes. And nationwide data indicates that veterans in states administered by TriWest’s counterpart, Health Net Federal Services, fared even worse.
But Alaska, where the scarcity of VA services made all veterans eligible for Veterans Choice, had the bitter distinction of watching its ambitious gains erode.
At back-to-back town hall sessions in an Anchorage high school auditorium in May, Yehia, a soft-spoken infectious disease specialist with wonkish enthusiasm for the workings of managed care, assured frustrated veterans and medical providers that things would change – again.
“You’re describing what I hear a lot. Community care was just fine before,” he told them. “We want to do a little ‘back to the future.’ ”
TriWest, he explained then, still would be critical to the Choice program. But beginning this summer, the company would no longer schedule veterans’ appointments. That workload began to revert to the same Alaska VA staffers who used to help Cramer Showers with her appointments.
If the hybrid approach goes well, the rest of the country may follow, making Alaska a pioneer once again, this time for the unraveling of Choice.
The changes are meant to stem the damage while the VA works on an ambitious proposal to reinvent its approach to community care – and reduce the role of private third-party administrators. The Choice program is due to expire next summer. But crafting its replacement won’t be simple, as key pieces will require buy-in – and substantial funding – from a divided Congress.
Meanwhile, TriWest remains responsible in Alaska for authorizing care, gathering medical documentation after appointments, paying claims and enticing medical providers to accept the program.
“The VA proposes to fix one facet of the problem,” said U.S. Sen. Lisa Murkowski, R-Alaska, who points out that fix falls far short of reinstating the successful system she fought to put in place for more than a decade. “I’m still not sold that the Choice Card provides meaningful choice for Alaska veterans.”
***
One in 10 Alaska residents is a veteran – the highest per-capita rate in the nation. Alaska Airlines pilots welcome veterans home to applause upon touching the tarmac at Ted Stevens Anchorage International Airport. Veteran discounts abound, even at fast-food franchises.
Some veterans choose to stay after stints at one of the state’s nine military bases; others come to this wild state more than twice the size of Texas for solitude and camaraderie with those who might share their demons.
“We’re trained to do unspeakable things at a moment's notice and be fine with it, and that catches up to you after awhile, so you like the serenity,” said Darrell Walker, 54, of Fairbanks, who suffers from post-traumatic stress disorder after serving as an Army sergeant in Panama and the first Gulf War.
The VA first turned to private doctors to help care for veterans after World War II. Maj. Gen. Paul R. Hawley, then the VA’s chief medical director, called it the hometown program. By 1950, the onetime Indiana country doctor who had overseen medical services in the European theater had recruited 100,000 physicians to the cause.
In Alaska, veterans tapped such partnerships for years to receive treatment in the community on the VA’s dime.
But in the 1990s, the political winds shifted. Veterans would remain within the VA system wherever possible – and for Alaska’s vets, that often meant flights to the Lower 48.

Cramer Showers endured months of lonely motel living in Seattle in 2005 as she underwent chemotherapy and radiation treatments at the VA hospital there. She says she was grateful for the care, grateful that she never saw a bill.
But Murkowski heard from plenty of frail and infirm veterans who she believed were suffering needlessly. She recalls the case of one elderly Anchorage man who in 2000 begged to stay home with his family while receiving care for advanced cancer. The answer from VA officials: No.
“We were pushing a rock up a hill,” Murkowski said. “There was such intransigence. … We had a VA system where we were basically being told one size fits all.”
The next wave of change came after retired Army Gen. Eric Shinseki took the VA helm in 2009 and gave the nod to new Alaska VA leadership to experiment. An arrangement with the Department of Defense allowed the VA to buy care at Air Force and Army hospitals. A first-of-its-kind agreement with the Alaska Native Tribal Health Consortium provided VA-funded services to veterans Native and non-Native alike in remote corners of the state.
In 2010, a program called Care Closer to Home offered private oncology treatment in Anchorage and Fairbanks. Other specialty care soon followed. And when a waiting list for primary care at the Anchorage VA clinic ballooned to 900, those services also were outsourced, bringing the wait list down to just a handful.
By the time the public learned that veterans had died while on secret wait lists in Phoenix and elsewhere, Alaska finally was in good shape. On June 1, 2014, there were 24 veterans on the state’s electronic wait list – compared with 2,005 in Phoenix and 4,240 in the Middle Tennessee Healthcare System, the highest in the nation.
“I couldn’t tell people enough how great my experience was,” said Lawrence Chapin, 43, of Fairbanks, who as an Army sergeant constructed operating bases and other war infrastructure in Iraq. “I said I was just lucky.”
A large man with a quick smile and graying goatee, Chapin was medically discharged in 2011 after two parachute malfunctions from his early career caught up with him. At first, getting cleared by the VA to see outside physical therapists, acupuncturists and osteopaths was quick and easy, he said. Radiology appointments to assess his degenerating shoulder and spine came particularly fast.
“They cut the authorization, and you could go down to the imaging center the same day,” he said. “I thought everything was as good as I could get it.”
Not so once the Veterans Choice program hit. Bills piled up. TriWest erroneously told him that his wife’s private insurance would have to pay first for his care. Then, last December, Chapin’s VA doctor sent him for a cardiac stress test. On a Sunday soon after, he got a call from a VA nurse.
“We saw something, “ she said. “We need to get you in right away for a CT scan.”
Choice, she said, would follow up to schedule. But several weeks passed before Chapin got the call from TriWest. He waited until March for the scan, his anxiety mounting. Luckily, it turned out his condition was not serious.
“If it had been an emergency, I would be dead,” he said. “That was my breaking point.”***
Veterans Choice was not supposed to destroy what Alaska had built. Murkowski, the Alaska senator, said she was assured that the program would offer “yet one more tool” for purchasing care. But then, “we learned, nope, it’s not another tool. It is the tool.”
Unbeknownst to Alaska VA officials, the use of private care had spiked across the country in the wake of the dying-while-waiting scandal. But VA facilities weren’t using Choice. The program wasn’t ready. Instead, they ran the VA budget $3 billion into the red.
So early last summer, Alaska VA officials said, spending on non-VA care was frozen abruptly. With rare exceptions, the only way to send veterans to private doctors was to use the dollars Congress had set aside for Choice. And that meant going through the program.
Veterans found their surgeries postponed or canceled. They scrambled to switch doctors. A number of them had difficulty finding providers willing to accept patients under the Choice program.
The VA’s urgent fiscal crisis passed. But the VA – and Congress – wanted the allocated Choice money spent. On Oct. 1, another nationwide memo reiterated the directive: The program should trump older methods of buying care whenever possible.
Veterans Choice doesn’t cover emergency services. The VA uses other dollars for that. Alaska’s VA also successfully scrambled to secure funding to continue sending veterans to partner military hospitals and Native health clinics. Most other private care – radiology, physical therapy, orthopedics and so on – goes to Choice.
In May 2014, as top executives left the VA in the wake of the Phoenix scandal, James Tuchschmidt was tapped to step in as the agency’s No. 2 health official. He oversaw the implementation of the Choice program before himself leaving for private industry last fall. And it was Tuchschmidt who signed the memo that made Choice mandatory. Today, he says the goal was to simplify the VA’s various ways of buying care and make sure that the $10 billion Congress set aside for the program got spent.
“Congress intended veterans to have this Choice program,” he said. “They gave them this new benefit.”
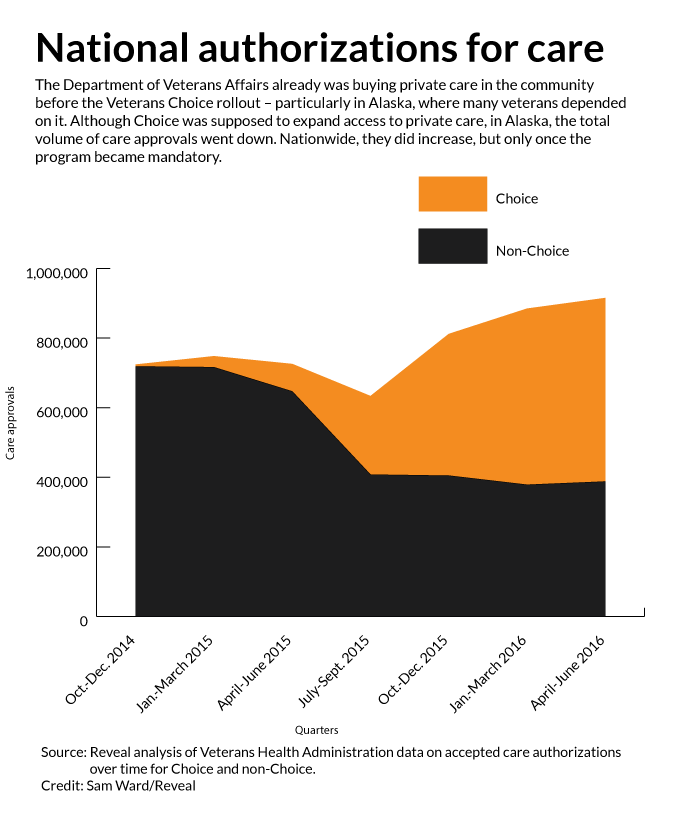
But data show that mandating the use of Veterans Choice did not expand access to private medical appointments for Alaska veterans. Instead, overall authorizations for community care decreased.
The three months ending in December 2014 would prove a high-water mark for private care approvals in Alaska: More than 19,000 came through that quarter. Hardly any were handled through the nascent Choice program.
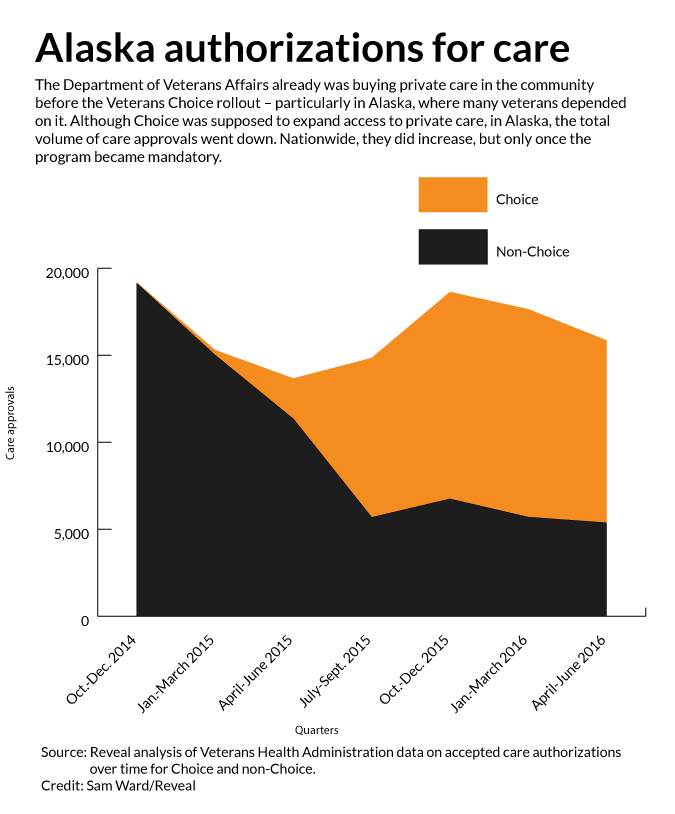
A Reveal analysis of approvals since shows a downward trend. Totals for the most recent quarter, ending in June, were 17 percent lower. Nationally, results are brighter: a 26 percent increase between the same two quarters.
But, as in Alaska, the use of Choice rose significantly only after the VA curtailed the use of the older method of buying care, without the middleman.

“We really didn’t get a choice,” Micki Millecam, 31, said in a shaking voice as she sat stiffly in a hospital emergency waiting room on the Kenai Peninsula in late April.
The Army veteran and mother of two had broken her upper back while stationed in South Korea and was used to flare-ups. But this one was different. She could barely breathe. It was her second trip to the ER since a VA nurse had sought an urgent MRI for Millecam through the Choice program nine days earlier – with no result.
“VA,” Millecam said, “chooses for you.”
***
On a warm day in late April, the volunteer executive committee of the Alaska chapter of Disabled American Veterans trickled into a Fairbanks hotel conference room for the group’s annual gathering.
While Veterans Choice wasn’t on the agenda, it was on everyone’s mind. In a show of hands, 8 out of 10 said they were waiting longer for their outside appointments than they had before they were directed to use the program. Eight of 10 also said they were receiving unexpected bills.
Leading the convention with mischievous bangs of his gavel was Darrell Walker, the combat veteran who moved to Fairbanks for the soothing isolation. He stood and occasionally paced in physical discomfort through much of the two-day meeting.
After undergoing surgery last fall to rebuild a damaged shoulder, Walker received approval from TriWest for physical therapy sessions to limber his muscles. As those wrapped up in mid-January, he said, he watched as his physical therapist faxed a request for the second phase: strengthening.
Two months passed, and Walker heard nothing. Then he slipped on ice and hurt his back, requiring more care. He followed up with TriWest in late March and finally got his physical therapy scheduled for his shoulder and spine – in May.
Air Force veteran Pam Beale, 63, recently had faxed bills totaling $9,000 to her favorite nurse at the Alaska VA’s Integrated Care Service, begging for help to make them go away.
Before the Integrated Care Service department became a de facto crisis resolution center to help navigate Choice nightmares, it had won the trust and gratitude of many veterans by coordinating their private care. Under the back-to-the-future pilot Dr. Baligh Yehia helped negotiate, that department now is assuming some key TriWest responsibilities: taking calls from veterans, directly scheduling their appointments and sending their medical documentation to providers.
Beale’s bills were for treatment approved through the Choice program. But in an experience common among Alaska veterans, the bills had come directly to her, followed by aggressive predawn phone calls from a collection agency.

Elaine Williams, a 67-year-old retired VA addiction therapist, said the care she was receiving hadn’t gotten worse, but the process had.
In April, Williams was at the tail end of a five-month wait for knee replacement surgery. She ended up going twice for the same appointment – a preoperative chest X-ray, blood work and EKG. She initially had pressed to delay because the surgery was more than a month off. The TriWest worker insisted. Williams went, but turned out to be right: Several weeks later, she had to go again.
The following day, she said, three TriWest workers called, all pressing to arrange another surgery-related appointment – one she’d already scheduled.
“Nobody’s communicating with anyone,” the Air Force veteran said.
One possible clue to why Williams’ phone kept ringing is buried deep in the contract the VA negotiated with TriWest: The VA agreed to pay $10.56 for every outbound call. And in interviews, former and current call center workers described heavy pressure to meet quotas of 60 or more calls a day, even as they scrambled to analyze medical documents, find willing providers and meet other appointment-scheduling quotas.
Jacquelyne McElwee-Brown, 60, who worked at a call center in San Diego County, said managers “just wanted to push the authorizations through, push ’em through.”
McElwee-Brown comes from a proud family of veterans and was drawn to the job because of the program’s mission. But she said she and many others quickly became disillusioned.
“These fundamental call center strategies of making calls, calls, calls,” she said. “I think our morals and values and beliefs were compromised.”
TriWest CEO David McIntyre said staffing call centers on such a tight timeline – legislation required the Choice program to be up and running in 90 days – led to hiring mistakes. But he said the centers now are making a greater effort to find workers with health care experience.
He did not dispute the claims of call center quotas but said: “While it may appear to some that there is an objective to get more fees, the fact of the matter is the quota we care about is making sure a veteran gets placed with care.”
***
In unveiling Alaska’s Care Coordination Pilot in June, VA officials said the state would test-run improvements for the rest of the country by putting to use its “long history of coordinating with community providers to serve veterans.”
The national plan is to decrease reliance on TriWest and Health Net and jury rig Veterans Choice into a program that matches Yehia’s new mantra: “easy to understand, simple to administer and meets the needs of veterans, community providers and VA staff.”
Under the VA’s plan for the new and improved version of Choice, for instance, veterans will no longer deal with private call centers.
But for Alaska, the ride “back to the future” is fraught with complications and unknowns. The process of getting care that Williams complained about has been simplified only slightly. While local VA staff now will make appointments, they must then notify TriWest, which remains responsible for giving the provider the final nod.
A TriWest letter addressed to providers and posted on the company’s website warns: “Like before, providers should not administer care to a Veteran without an authorization; otherwise, they risk losing reimbursement.”
Those faxed authorizations are the very ones that veterans such as Tina Cramer Showers say often have failed to make it into the hands of their doctors – and that providers complain often arrive riddled with errors.
In April, Krista Selan, rehabilitation office coordinator for South Peninsula Hospital in Homer, said TriWest’s authorizations required multiple calls to fix, as they were “never correct the first time … and I’m not exaggerating.” The back and forth delayed care, sometimes for weeks.
Alaska’s pilot program formally launched July 18, though the full handoff will not happen until at least mid-October. A week later, with TriWest web training scheduled for medical providers the following day, neither South Peninsula Hospital nor two Anchorage providers contacted by Reveal had received the company’s letter or any details about the changes.
“It’s disturbing that nobody has this information,” said Cynthia Morse, who manages an Anchorage neurosurgery practice.
McIntyre said his company sent a “blast fax” before the mid-July launch, along with letters to all providers. He suggested that because the letters likely were addressed to doctors and not practice managers, they may not have been opened promptly.
“I don’t work in their office,” he said. “I can’t say what they do with their mail.”
Contacted in late July, Selan said she had “noticed no significant changes, better or worse.”
TriWest also still is charged with building the network of Veterans Choice providers, and paying them, at a time of eroded trust.
Data provided by the VA show only a slight dip in Alaska primary and specialty care providers accepting Choice between January and March of this year. But some providers who stayed on the list say they capped their patient loads.
Morse let TriWest know early this year that one of the two surgeons at the practice would keep seeing veterans she already had accepted under the program. But she would restrict new veteran patients to only the most serious cases, involving brain surgery, for instance.
“Our issue – and that of just about every provider in the state of Alaska that I’ve spoken to – is that it’s very difficult to get reimbursement,” Morse said.
According to McIntyre, more than a third of claims that TriWest receives from medical providers contain errors, which drags out the reimbursement process. He said 90 percent of what he called “clean” claims now are paid within 30 days throughout the company’s 28-state territory.
Meanwhile, taxpayers are taking a hit.
The VA initially contracted with TriWest and Health Net in part because such companies can impose standardized rates on their networks of providers that often are lower than those paid under direct agreements with local or regional VAs.
With the Choice legislation in hand, the VA hastily scheduled an industry day for potential vendors. But James Tuchschmidt, the former VA health official, said, “We learned from virtually everybody there that they thought the timeframe was unrealistic.”
“They weren’t really willing to risk their reputation and their resources on trying to stand something up so quickly,” he added. “They just didn’t think it was possible.”
That left Health Net and TriWest. Both had won bids in late 2013 to administer a similar, less ambitious program – one harshly criticized by the VA’s Office of Inspector General for some of the same inadequacies that came to plague Veterans Choice.
Although Tuchschmidt was not privy to the negotiations, he said the VA’s bargaining position when those contracts were modified to include the Choice program was “not a very good one. We didn’t have any options.”
Obtained through a public records request, the contracts show that administrative fees tripled and implementation fees quadrupled compared with the smaller program the companies had been running. Those fees make the program expensive.
An internal cost analysis commissioned by the VA concluded that buying medical care through Choice nationally was cheaper than purchasing it directly from providers – the approach that had worked so well in Alaska. But the analysis’ five-year projection shows that high fees paid to the companies erased those gains, making it impossible for Choice to break even.
Yehia called the analysis flawed for not factoring in the cost of VA staff time and said improvements to the Choice program earlier this year have resulted in lower fees.
As for McIntyre, he says fees climbed because Choice is more complex to administer than the prior smaller program. His company invested “$70 million of our own money” to get the program up and running nationwide, he said, and has yet to turn a profit. Health Net said in a statement that the company doesn’t comment on contract terms.
In Alaska, the end result was upheaval. But opinions differ on cause and effect.
Tuchschmidt says the Alaska VA had created a stellar system of buying private care that the one-size-fits-all Choice program clearly disrupted. He calls the unfortunate journey “probably one of the casualties of trying to do something in 90 days.”
But Sen. Lisa Murkowski said the turning point came later, with the VA’s decision to make Choice mandatory.
“I blame the VA,” she said, noting that “Alaska had demonstrated ably prior to this that you don’t need the middleman. In fact, the middleman complicates it.”
***
Whatever comes next, some damage cannot be undone.
Since June 2015, Cramer Showers’ cancer care at Katmai Oncology Group – affiliated with Providence Alaska Medical Center – was authorized and handled through Veterans Choice, her records show. Yet the Providence billing office told her TriWest directed it to bill Medicare, despite the fact that the VA cannot legally compel Medicare to pay first under Veterans Choice.
Earlier this year, Cramer Showers received statements tallying her portion at $18,000. She said a Medicare representative recently told her the balance has been zeroed, but no one has been able to explain to her what happened.
Meanwhile, bills keep coming. She recently received a Providence Imaging Center invoice for $351 for a mammogram approved under Veterans Choice, which noted that TriWest was billed more than 60 days earlier and had not yet paid.
She’s added it to her pile. But her priorities are elsewhere. Cancer-free in the spring, Cramer Showers in recent months has found herself in agonizing pain as her lymph nodes swell, then shrink, on the side of her neck, face and right shoulder.
Her oncologist has rushed her in for several scans, urging her to use Medicare instead of Veterans Choice to avoid the wait for an authorization.
Reveal asked the VA about Cramer Showers and several other veterans in late June and provided medical releases so it could probe their circumstances. Last week, a VA spokeswoman said the agency still was looking into the cases.
For Darrell Walker of Fairbanks, Veterans Choice delays had physical consequences. After a surgeon rebuilt his right shoulder last fall, Walker completed initial physical therapy to regain movement. But he could lift only 5 pounds. It was time to work on strengthening. He waited, then waited some more.
An airplane mechanic at the small city airport, he was unable to lift, bend and crawl – all essential to his work. His employer kept him on part time on special duty.
In March, Walker said, his employer “dropped me.”
“Choice, they’re not responsible for your injuries, but they are responsible for the consequences of what happens when they say, ‘Oh, well, we can't get you in for 90 days. We can’t get you in for four months,’ ” he said. “Or when they say, ‘We have no provider in our network here.’ ”
“What do I do now?” he asked. “How am I supposed to survive? How am I supposed to make my living?”
When the day in early May finally arrived for his shoulder therapy, he endured another two-week delay because TriWest failed to transmit the authorization to his provider. Once in, he discovered his shoulder “had atrophied back to where it was right after surgery, so I had to start all over again.”
In mid-August, Walker flew to Anchorage at the VA’s expense for a presurgical consultation for his neck and back. But TriWest, still handling scheduling, had booked him on a Monday – surgery day. The physician wasn’t there. Walker flew home, irate and in pain, only to learn the next available opening is in October.
Then there are veterans who gave up on the VA health care system altogether because of Veterans Choice and have vowed not to return.
After waiting at the ER for nine hours for an MRI of her injured neck and back in late April at Soldotna’s Central Peninsula Hospital, Micki Millecam went home instead with a few pain pills.
Two days after she told a VA nurse she had talked to a reporter, she got the scan. It revealed three herniated disks in her upper back and neck.
Soon, she got a call from a TriWest representative, telling her the orthopedic specialist she had requested would be contacting her within minutes. That call never came, Millecam said. A letter from TriWest a few weeks later said the medical office had tried in vain to call her. It listed the wrong phone number.
By then, Millecam had given up. Using Medicaid instead, she got a referral from an ER doctor to Kenai Spine and an appointment six days later. She has been able to avoid surgery and is undergoing physical therapy, also using Medicaid.
“I’ve pretty much had it with the VA,” she said.
This story was edited by Amy Pyle and copy edited by Stephanie Rice and Nikki Frick.
Lee Romney can be reached at leoraromney@gmail.com. Follow her on Twitter: @leeromney.
