This article is part of HuffPost’s Project Zero campaign, a yearlong series on neglected tropical diseases and efforts to fight them.
Imagine that you wake some mornings to find you’re so weak you can barely rise from your bed. Sometimes there are aches in your joints, too, or pounding in your head. Sometimes your stomach is in knots.
These symptoms have been coming and going for months, and you know something’s wrong. It usually takes hours to travel to the nearest medical clinic, but you don’t feel strong enough to go. Luckily, a group of health workers arrives in your village ― they call over a megaphone, asking people to come for checkups. You stagger to the big tree near the market where the health workers have set up their equipment in the shade. They say they need to run some tests, and they draw blood from your fingertip.
Later, they run more tests and push a three-inch needle into your spine ― the pain is excruciating. You try not to scream.
The tests reveal there is a parasite lurking in your blood and inside your brain. (You were infected when a fly bit you. It happened so long ago, you don’t remember when.) You have a disease called “sleeping sickness,” the health workers inform you. But you’re very lucky, they say, because they have medicine that can treat it. If you hadn’t discovered this in time ― and many people don’t ― the disease would have progressed until you began hallucinating, then slipped into a coma and died.

Today, sleeping sickness ― also known as human African trypanosomiasis ― is endemic in 36 sub-Saharan African countries, putting about 13 million people at risk of infection. For centuries, it was a mysterious disease that killed people by the hundreds of thousands during its worst outbreaks.
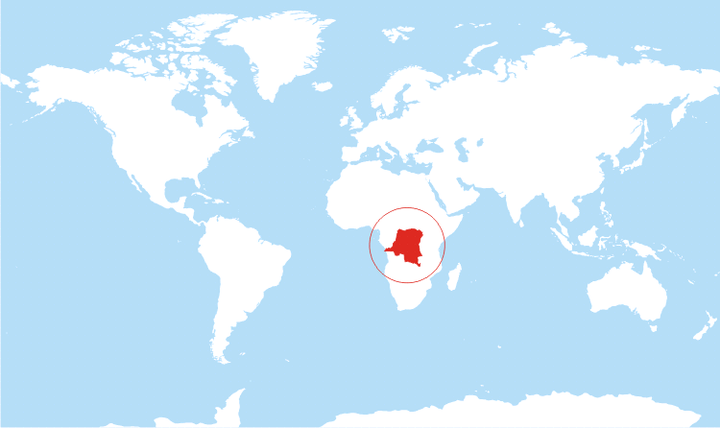
The last big surge of sleeping sickness started in 1970 and lasted until the late 1990s. The disease tends to strike in rural or isolated areas, making it difficult to bring treatment to people who need it. Regional instability is another factor fueling the spread of the disease. In the last decade, over 70 percent of reported cases of sleeping sickness occurred in the Democratic Republic of Congo, according to the World Health Organization.
Modern surveillance and treatments have helped dramatically lower the number of cases in recent years. In 2009, the number of cases of sleeping sickness reported to the World Health Organization dropped below 10,000 for the first time in 50 years. In 2015, there were fewer than 3,000 new cases.
We are now at a critical time: With the low number of infections and the introduction of new treatments that are easier to administer than ever before, there may finally be a chance to eliminate the disease in the next few years.
“Important advances have been made in the control of this disease in the Democratic Republic of Congo — something no one would have imagined a few years ago,” Ashok Moloo, a spokesperson for the WHO told The Huffington Post.
What makes sleeping sickness so deadly?
Sleeping sickness is caused by the microscopic parasite Trypanosoma brucei, which is carried by the blood-sucking tsetse fly. When the fly bites a human, it transmits the parasite. Unlike most other pathogens, the parasite can pass the blood-brain barrier and infiltrate the nervous system. At this point, the disease begins to wreak havoc on the brain and becomes deadly if untreated.
Early symptoms include fever, headaches, joint pain and itching ― very similar to symptoms of many other diseases. Treating sleeping sickness at the early stage includes a blood test to confirm the diagnosis and administering medication. People living far from medical care might not get tested or treated before the disease progresses and begins to harm the nervous system.
Once the parasite reaches the brain — which, in the case of the more common strain of the disease, can take months or years after infection — the second stage begins. At this point, the symptoms become more severe and the disease becomes harder to diagnose and treat. The symptoms include headaches, tremors, confusion, violent behavior, paralysis, seizures and bouts of extreme sleepiness at unlikely hours — hence the disease’s name. Eventually, without treatment, coma and death follow.

To diagnose the second stage, doctors need to find evidence of the parasite in the spinal fluid. This requires a procedure known as lumbar puncture, which involves inserting a large needle into the spine. The test is painful and expensive and requires expertise to conduct.
Treatments can be complicated, even dangerous.
Anti-microbial medications such as pentamidine can treat the early stage of sleeping sickness. The second stage of the disease requires stronger ― sometimes deadly ― medications.
For decades, the main drug used for treating the second stage of the disease was an old compound called melarsoprol. This drug, made of arsenic and dissolved in antifreeze, is highly toxic and kills 1 in 20 patients within minutes of injection. The extreme pain it causes led doctors to call the treatment “fire in the veins.” This medicine has been phased out in the past 10 years, but it’s still used to treat a rarer form of sleeping sickness that makes up about 2 percent of cases.

Another treatment option that replaced melarsoprol is eflornithine, which was under investigation as an anti-cancer drug in the 1970s and was used to treat excessive facial hair in the 1990s. Later, scientists discovered that eflornithine is also effective in killing the sleeping sickness parasite. Thanks to advocacy efforts and pressure from the WHO and Doctors Without Borders, researchers resumed developing a version of this drug to treat sleeping sickness.
It’s not the most ideal option, though: Eflornithine must be administered by IV in a hospital setting, something that’s often difficult to execute in rural areas where the disease is more common.
A new medicine has brought new hope.
A few years ago, in search of a better treatment option, researchers found an old anti-infective drug that seems effective in killing the parasite that causes sleeping sickness.
Subsequent research and clinical trials have shown the drug, called fexinidazole, is nontoxic and could indeed cure the disease. What’s more, the drug comes in pill form, making it much easier to use than existing options.
Fexinidazole is in the last phase of clinical trials and could begin to replace existing treatments by next year. It works for both stages of sleeping sickness, which means it removes the need for the painful and costly lumbar puncture to diagnose the second stage of the disease.

“This drug seems likely to be approved for sleeping sickness, and is an excellent example of drug discovery scientists ‘rescuing’ a compound that was otherwise in the dustbin of a large drug company,” Michael Pollastri, an associate professor at Northeastern University, told HuffPost. (Pollastri, an expert in the discovery of new therapeutics for neglected tropical diseases, wasn’t involved in the development of this new drug.)
The Drugs for Neglected Diseases initiative, a nonprofit drug research and development organization that collaborates with labs and universities around the world, helped developed this new pill with global pharmaceutical firm Sanofi. When the last phase of trials ends in 2017, DNDi and its partners will seek approval to use the medication for both stages of sleeping sickness. (HuffPost is raising money to support DNDi’s efforts to eliminate sleeping sickness.)
The end could be in sight.
With an easy-to-use medication around the corner and a historically low number of infected people, it now seems more possible than ever to stamp out sleeping sickness. Experts at DNDi believe the disease can be eliminated by 2020.
But there are still some steps left.
Fexinidazole still needs to be tested on children, pregnant women and other vulnerable populations. It also has to be tested for a less common but harder-to-treat variant of sleeping sickness.
Moreover, fexinidazole still requires patients to carefully follow the course of treatment.
“The new oral candidate-drug, fexinidazole, which is still under clinical development, could be helpful,” the WHO’s Moloo said. “But, even with fexinidazole, treatment will have to be spread over 10 days and in different dosage, as absorption of this medicine is related to food intake.”
Therefore, DNDi and its partners are working on an even stronger, simpler treatment, dubbed SCYX-7158. This new compound would require patients to swallow three pills in a single sitting. It will go into last stages of clinical trials soon, and could become available to patients by 2018.
“We are confident that these new therapies will be a key part of the global effort to eliminate sleeping sickness within a matter of years,” Bernard Pécoul, executive director of DNDi, said in a statement.
DNDi is a recipient of grants from the Bill & Melinda Gates Foundation, which also funds HuffPost’s Project Zero series. All content in this series is editorially independent, with no influence or input from the foundation.
If you’d like to contribute a post to the series, send an email to ProjectZero@huffingtonpost.com. And follow the conversation on social media by using the hashtag #ProjectZero.
More stories like this:

