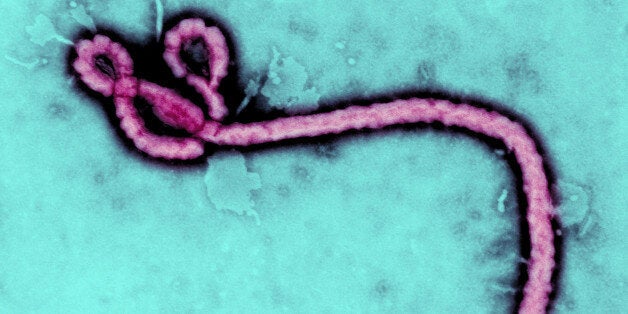
Luckily, the two Americans who received ZMapp, the new experimental drug for Ebola, seem to be improving, which holds great promise and hope for thousands of other people but also raises broader ethical issues and questions.
The virus was first discovered by scientists in 1976, and several outbreaks of Ebola in the developing world killed 1,000 people through last year. Since April of this year it has killed over 900, and hundreds more are sick. Frighteningly, the epidemic is rapidly rising. Thousands are at risk.
Developed largely through U.S. government grants, ZMapp has cured monkeys, but until this week it had never been tried in humans. Ordinarily, carefully controlled clinical trials would first investigate the safety of the drug in healthy volunteers, and then in patients, to evaluate its effectiveness, toxicity, and appropriate dosing in humans.
Instead, two Americans received it. Whether their improvement is due to the drug is not yet known.
The World Health Organization (WHO) will be convening a meeting to discuss whether efforts should be made to distribute the drug widely in Africa. If the two Americans continue to improve, ideally the drug could then be given in an expedited way to a somewhat larger number of patients, with the results observed. If the drug continues to show promise, efforts could then expand to offer it more broadly. That approach would best balance humanitarian concerns with the limited scientific knowledge about the medication's effects.
Yet if the drug shows promise in these ways, deeper questions then emerge: whether much wider distribution is possible in the near future, how it should be given, and who should pay for it. Some observers have already asked why the only two patients to receive it thus far have been Americans rather than Africans.
Hopefully, if continued results are positive, the federal government will fund efforts to disseminate the drug, as well as to develop, manufacture and test it. Though it remains unclear whether large quantities of the drug can be manufactured in the near future, we can certainly try. Hopefully, too, Congress will support such a mission. At a time when U.S. prestige abroad is low, providing the drug could help demonstrate several of our nation's strengths: that we can advance science in the service of helping citizens of the world.
Still, even if the medication works and is provided abroad, obstacles will remain to educate patients adequately about it and obtain appropriate informed consent. The fact that the drug is experimental and may still fail or make patients sicker -- even if it seems to offer benefit to a few patients -- needs to be explained in a way that patients in Africa, many of whom have little education, can understand. Barriers exist in part for cultural and linguistic reasons. In some African languages, for instance, there is no word for "placebo" or "experimental treatment," only for "cure. Questions remain regarding whether the drug should first be tested against a placebo or simply given to everyone. Use of a placebo will help scientists understand the drug's effectiveness. But if the medication turns out to work, patients who were randomized not to receive it will have lost out. These quandaries are complex, and WHO needs to explore and address them very carefully.
The epidemic and its potential treatment should remind us of enormous underlying disparities in health care and resources between wealthy and poorer nations. The current Ebola outbreak has received far more worldwide attention than previous ones, partly, I suspect, because patients this time, unlike in many past outbursts, include Americans.
This drug's potential benefits also represent a potential success for science, and for government investment in medical research. At a time when science is under potent political threat in this country, and when the NIH budget has been flat (and decreased in real dollars), ZMapp illustrates the benefits of such funding.
This outbreak should thus remind us, too, of how much we live and die in a fragile, interconnected world. A patient can be exposed to Ebola in Africa in the morning and land in New York that evening. That fact should help unite us against this common enemy, but it instills fear in many people. We will need to combat excessive anxiety and fear. Already one patient was admitted to a New York Hospital with fever and pains -- symptoms that could indicate Ebola or many other diseases. Since he had recently returned from Africa, doctors placed him in intensive hospital isolation, concerned that he might harbor the virus. Fortunately, he turned out not to have it, but in upcoming weeks other such cases will no doubt emerge. Such fears need to be addressed appropriately, to avoid hysteria that new outbreaks of infectious diseases -- such as HIV -- have unfortunately triggered in the past.
Ebola should remind us that in our ever-more-interconnected world, we all face similar threats but can, ideally, work together to solve them.
