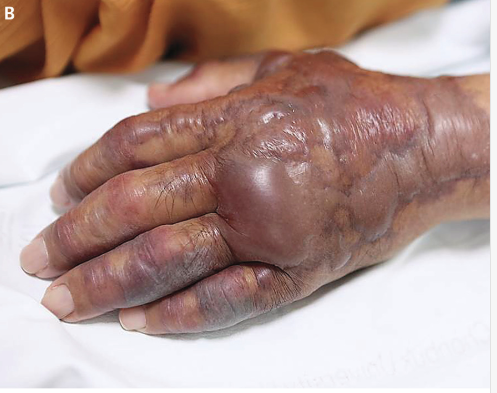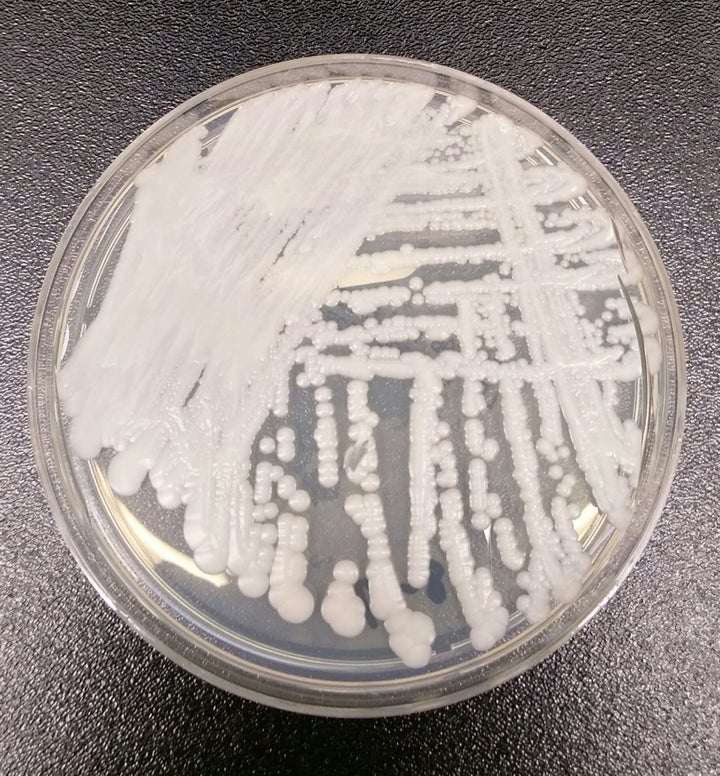
A drug-resistant fungus that first emerged in the U.S. only a few years ago has been linked to four deaths, and health officials are on guard about its potential to spread in healthcare facilities throughout the country.
C. auris, a yeast that has sickened people around the globe and caused potentially deadly infections, appears to have arrived in the U.S. a few years ago, according to the first report on C. auris released by the U.S. Centers for Disease Control and Prevention.
Because C. auris cases have cropped up in other countries, the CDC decided to alert all U.S. clinics, labs and public health authorities about the potential danger in June. The alert also called on these facilities to start collecting information about any potential cases of C. auris, which resulted in the CDC’s first study on the fungus.
Thanks to the request for reporting, the CDC found that since 2013, there have been only 13 cases of the fungal infection in the U.S. Between 2013 and August 2016, there were seven cases of the fungal infection reported in the U.S., and these seven are the focus of the first CDC study on C. auris. Since August, six more were reported and are currently being investigated.
While these U.S. cases have been confined to hospital-linked infections and aren’t circulating in the community, public health experts are worried that it could grow into a major threat. There are only three classes of medications that can cure fungal infections, and there have been cases of C. auris in other countries that have resisted all three treatments.
“We feel we need to take it very seriously, be aggressive and get out in front and try to see what we can do to prevent its spread.”
- Dr. Tom Chiller
“When you’re dealing with a multidrug resistant pathogen that we know is causing a lot of disease in countries where it is more widespread, then we worry about it causing similar problems in the United States,” said Dr. Tom Chiller, chief of CDC’s Mycotic Diseases Branch. “We feel we need to take it very seriously, be aggressive and get out in front and try to see what we can do to prevent its spread.”
Here’s what you should know about the new fungus.
1. All the U.S. cases are linked to a healthcare setting
The seven cases of C. auris occurred in healthcare facilities in New York, Illinois, Maryland and New Jersey and struck hospitalized patients with serious underlying medical conditions. Four people died, but it’s unclear whether they died of their pre-existing medical condition or the new C. auris infection.
Five of the cases were resistant to at least one antifungal medication, but unlike strains from other parts of the globe, they were not resistant to all three classes of antifungal drugs doctors have at their disposal.
While the fungal strains are genetically related to strains isolated in South Asia and South America, none of the people who had C. auris infections had ties or had traveled to those regions, the CDC notes, which means they were probably infected locally.
2. C. auris is relatively new, and mostly affects severely sick people.
C. auris was first isolated in 2009 in Japan and was so-named because it came from the discharge in a patient’s ear canal (auris means ear in Latin). It has since popped up in South Korea, India, Pakistan, South Africa, Kenya, Kuwait, Israel, Venezuela, Colombia, the United Kingdom and Canada. It can cause serious bloodstream, wound and ear infections, and has struck patients of all ages. Based on the limited information they’ve gathered on these cases so far, researchers have observed that 60 percent of people with C. auris infections have died, but it’s unclear what, exactly, caused them to die, as people who get this infection are already severely ill.
Risk factors for C. auris infection include surgery, diabetes, the use of antibiotic and antifungal treatments, and use of a central line catheter in the arm or chest.
3. How to protect yourself from drug-resistant microbes
If you’re a patient in the hospital, one way to protect yourself from drug-resistant microbes is by asking everyone who enters your room to wash their hands. If you have a catheter in place, you should also ask your healthcare provider every day if that catheter is necessary, advises the CDC.
Scientists are generally most concerned about antibiotic-resistant bacteria, which is the biggest group of drug-resistant microbes. About two million people will get infected with an antibiotic-resistant bacterium every year in the U.S., while an estimated 23,000 people will die of their infection.
There is no national mandatory reporting for antifungal-resistant infections, so the CDC doesn’t have comparable figures, Chiller explained. But in a report outlining the most concerning drug-resistant pathogens, other species of Candida yeasts resistant to the anti-fungal medication fluconazole are characterized as a “serious” threat because it’s the fourth-most common cause of healthcare-linked bloodstream infections in the U.S.
CORRECTION: This story’s headline was changed to reflect that these are the first cases of the drug-resistant fungus Candida auris, but they are not the first cases of drug-resistant fungi in the U.S. We apologize for the error.